Platelet Concentrates in Regenerative Medicine: A Comparative Review of Platelet-Rich Plasma, Platelet-Rich Fibrin, and Concentrated Growth Factors
DOI:
https://doi.org/10.48048/tis.2026.13160Keywords:
Platelet-Rich Plasma (PRP), Platelet-Rich Fibrin (PRF), Concentrated Growth Factors (CGF), Platelet concentrates, Regenerative medicine, Fibrin matrix, Autologous therapy, Platelet-Rich Plasma (PRP), Platelet-Rich Fibrin (PRF), Concentrated Growth Factors (CGF), Platelet concentrates, Regenerative medicine, Fibrin matrix, Autologous therapyAbstract
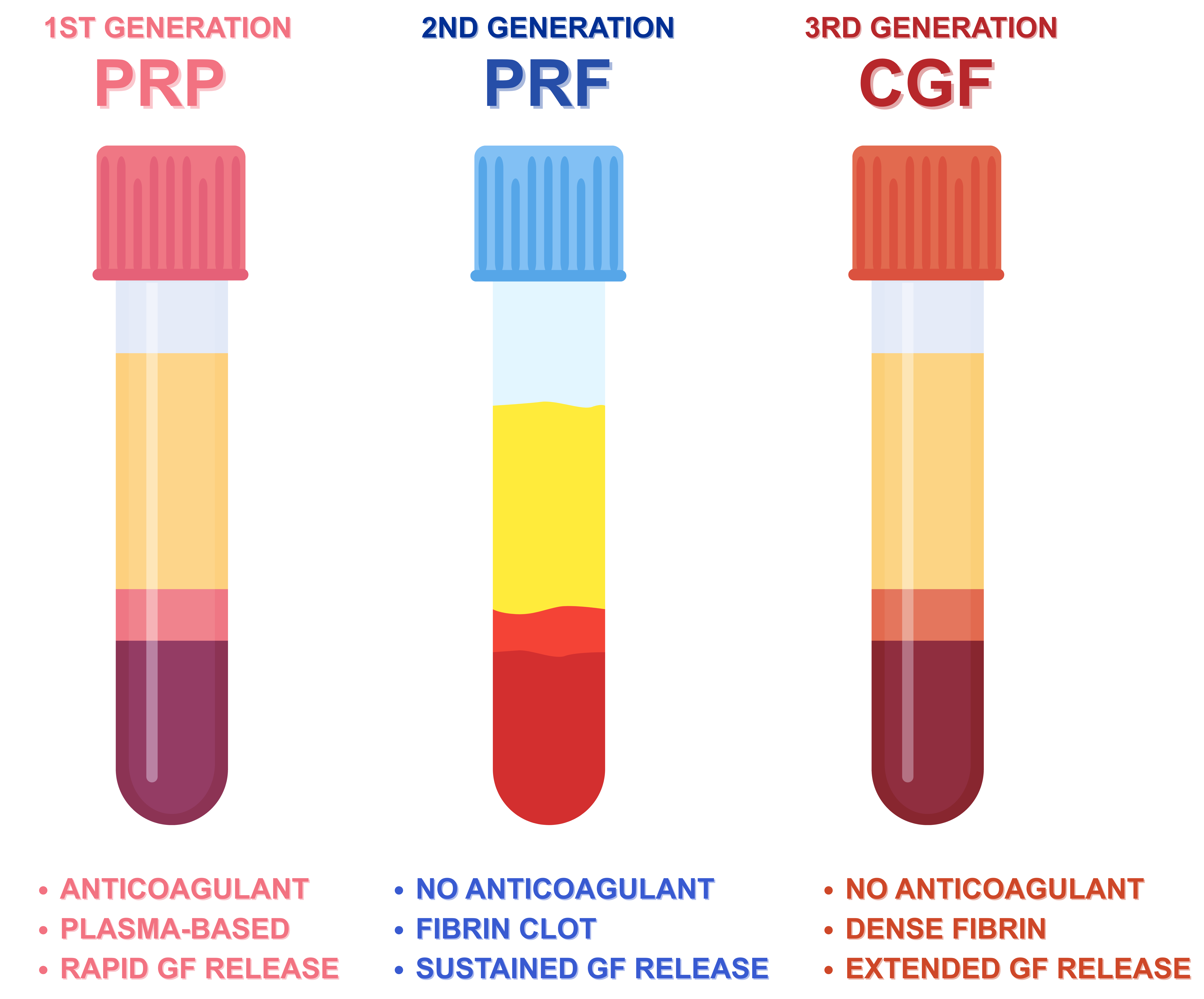
Platelet concentrates such as platelet-rich plasma (PRP), platelet-rich fibrin (PRF), and concentrated growth factors (CGF) are the Autologous Biomaterials of interest in regenerative medicine for their high growth factor content and simplicity of preparation. These products, which are obtained from peripheral blood by differential centrifugation protocols, represent a low-cost, biocompatible solution to tissue repair and regeneration for an extensive variety of clinical specialties from orthopedics, dentistry, and dermatology. This review contrasts and compares PRP, PRF, and CGF based on preparation protocols, cellular and molecular contents, growth factor release kinetics, and clinical applications. PRP, the first-generation concentrate, contains high platelet density but requires the addition of exogenous anticoagulants. PRF is a second-generation product with a fibrin matrix to provide slow growth factor release without additives. CGF, the newest development, uses variable centrifugation speeds to produce a denser fibrin matrix with a potentially higher regenerative potential. Current evidence suggests that the variations in preparation influence not just the biological activity, but also the clinical efficacy of each concentrate. While the most common, PRP is being progressively supplanted by PRF and CGF due to the fact that they are simple to use and additive-free. Nevertheless, standardization guidelines and comparative clinical studies are lacking, and therefore the optimization of treatment results is also challenging. In general, PRP, PRF, and CGF all possess distinct strengths in regenerative medicine. Additional understanding of their biologic profiles and handling during clinical practice is needed to individualize them in patient-tailored therapy and also to develop evidence-based guidelines for future application.
HIGHLIGHTS
- This review provides a structured comparative analysis of platelet-rich plasma, platelet-rich fibrin, and concentrated growth factors in regenerative medicine.
- Distinct differences in fibrin architecture and growth factor release kinetics underpin the biological and clinical behavior of platelet concentrates.
- Clinical evidence is strongest for platelet-rich plasma, while evidence for platelet-rich fibrin and concentrated growth factors remains limited and indication-specific.
GRAPHICAL ABSTRACT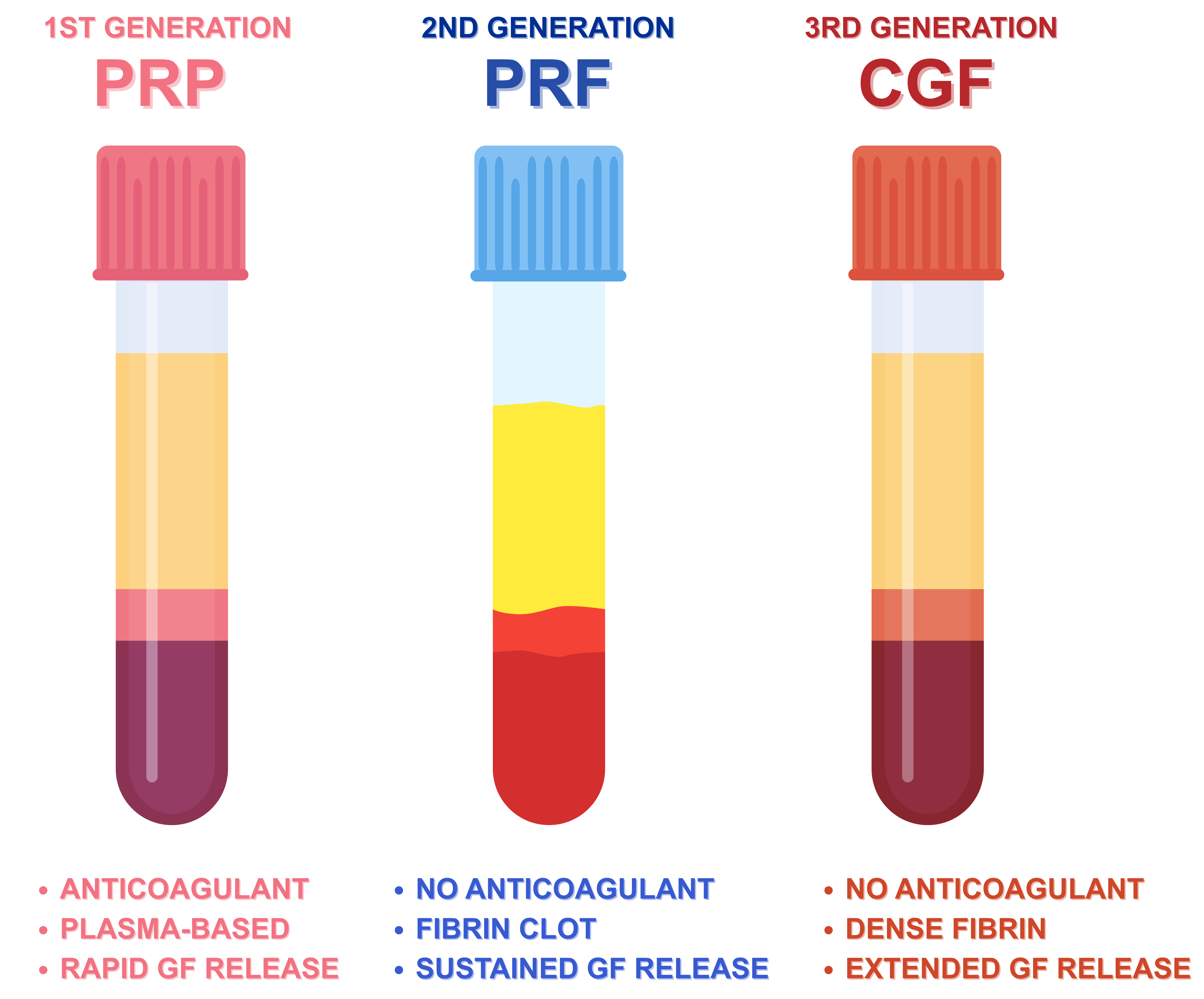
Downloads
References
PD Huynh, QX Tran, ST Nguyen, VQ Nguyen and NB Vu. Mesenchymal stem cell therapy for wound healing: An update to 2022. Biomedical Research and Therapy 2022; 9(12), 5437-5449.
N Saikia. Inorganic-based nanoparticles and biomaterials as biocompatible scaffolds for regenerative medicine and tissue engineering: Current advances and trends of development. Inorganics 2024; 12(11), 292.
V Bhutambare, C Kamble, S Khilari, D Bhalekar, P Gawari and A Kanase. Innovative strategies in regenerative medicine: Bridging science and clinical practice. International Journal of Advanced Research in Science Communication and Technology 2024; 4(3), 186-195.
ATM Nguyen. Regulatory T cells: From nobel prize foundations to engineered tolerance and next-generation immunotherapies. Innovative Medical and Biological Sciences Journal 2025; 1(1), 1-11.
J Ramos-Torrecillas, E de Luna-Bertos, O García-Martínez and C Ruiz. Clinical utility of growth factors and platelet-rich plasma in tissue regeneration: A review. Wounds: A Compendium of Clinical Research and Practice 2014; 26, 7207-7213.
CE Martínez, PC Smith and VAP Alvarado. The influence of platelet-derived products on angiogenesis and tissue repair: A concise update. Frontiers in Physiology 2015; 6, 290.
X Wang, MR Fok, G Pelekos and L Jin. In vitro and ex vivo kinetic release profile of growth factors and cytokines from leucocyte- and platelet-rich fibrin (L-PRF) preparations. Cells 2022; 11(13), 290.
M Schultze. Ein heizbarer objecttisch und seine verwendung bei untersuchungen des blutes (in Deutsch). Archiv für Mikroskopische Anatomie 1865; 1(1), 1-42.
G Bizzozero. Di un nuovo elemento morfologico del sangue e della sua importanza nella trombosi e nella coagulazione (in Italian). Fr. Wallardi, Italy, 1883.
S Murphy and FH Gardner. Platelet preservation. Effect of storage temperature on maintenance of platelet viability--deleterious effect of refrigerated storage. New England Journal of Medicine 1969; 280(20), 1094-1098.
CJ Oon and JR Hobbs. Clinical applications of the continuous flow blood separator machine. Clinical & Experimental Immunology 1975; 20(1), 1-16.
M Ferrari, S Zia, M Valbonesi, F Henriquet, G Venere, S Spagnolo, MA Grasso and I Panzani. A new technique for hemodilution, preparation of autologous platelet-rich plasma and intraoperative blood salvage in cardiac surgery. The International Journal of Artificial Organs 1987; 10(1), 47-50.
M Yang, B Deng, W Hao, X Jiang, Y Chen, M Wang, Y Yuan, M Chen, X Wu, C Du, DG Armstrong, L Guo, W Deng and H Wang. Platelet concentrates in diabetic foot ulcers: A comparative review of PRP, PRF, and CGF with case insights. Regenerative Therapy 2025; 28, 625-632.
J Choukroun, A Diss, A Simonpieri, MO Girard, C Schoeffler, SL Dohan, AJ Dohan, J Mouhyi and DM Dohan. Platelet-rich fibrin (PRF): A second-generation platelet concentrate. Part IV: Clinical effects on tissue healing. Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology 2006; 101(3), e56-e60.
SL Sacco. International Academy of implant prosthesis and osteoconnection. Lecture 2006; 12, 4.
SS Smyth. Platelet structure and function in hemostasis and thrombosis. In: JP Greer and DA Arber (Eds.). Wintrobe's Clinical hematology. Lippincott Williams & Wilkins, Philadelphia, United States, 2013, p. 389-410.
PE Stenberg, MA Shuman, SP Levine and DF Bainton. Optimal techniques for the immunocytochemical demonstration of beta-thromboglobulin, platelet factor 4, and fibrinogen in the alpha granules of unstimulated platelets. Journal of Histochemistry & Cytochemistry 1984; 16(9), 983-1001.
KE Johnson and TA Wilgus. Vascular endothelial growth factor and angiogenesis in the regulation of cutaneous wound repair. Advances in Wound Care 2014; 3, 647 - 661.
J Fang, X Zhang, X Chen, Z Wang, S Zheng, Y Cheng, S Liu and L Hao. The role of insulin-like growth factor-1 in bone remodeling: A review. International Journal of Biological Macromolecules 2023; 238, 124125.
X Zhang, FY Hu, J Li, L Chen, YF Mao, Q Li, C Nie, C Lin and J Xiao. IGF-1 inhibits inflammation and accelerates angiogenesis via Ras/PI3K/IKK/NF-κB signaling pathways to promote wound healing. European Journal of Pharmaceutical Sciences 2024; 200, 106847.
SH Shin, YG Koh, WG Lee, J Seok and KY Park. The use of epidermal growth factor in dermatological practice. International Wound Journal 2023; 20(6), 2414-2423.
M Farooq, AW Khan, MS Kim and S Choi. The role of Fibroblast Growth Factor (FGF) signaling in tissue repair and regeneration. Cells 2021; 10(11), 3242.
JT Rodgers, MD Schroeder, C Ma and TA Rando. HGFA is an injury-regulated systemic factor that induces the transition of stem cells into GAlert. Cell Reports 2017; 19(3), 479-486.
P Chandra, M Faizan, M Porwal, H Sharma and N Sachan. An overview and review of growth factors in wound healing: Emerging trends and innovations. Current Diabetes Reviews 2025. https://doi.org/10.2174/0115733998332692241202072249
H Luo, W Liu, Y Zhou, X Jiang, Y Liu, Q Yang and L Shao. Concentrated growth factor regulates the macrophage-mediated immune response. Regenerative Biomaterials 2021; 8(6), rbab049.
P Harrison and J Alsousou. The state of the art and future of PRP therapy. Platelets 2021; 32(2), 150-151.
CS Kingsley. Blood coagulation; evidence of an antagonist to factor VI in platelet-rich human plasma. Nature 1954; 173(4407), 723-724.
DM Dohan Ehrenfest, L Rasmusson and T Albrektsson. Classification of platelet concentrates: From pure platelet-rich plasma (P-PRP) to leucocyte- and platelet-rich fibrin (L-PRF). Trends in Biotechnology 2009; 27(3), 158-167.
M Dejnek, J Witkowski, H Moreira, S Płaczkowska, P Morasiewicz, P Reichert and A Królikowska. Content of blood cell components, inflammatory cytokines and growth factors in autologous platelet-rich plasma obtained by various methods. World Journal of Orthopedics 2022; 13(6), 587-602.
BW Oudelaar, JC Peerbooms, R Huis In't Veld and AJH Vochteloo. Concentrations of blood components in commercial platelet-rich plasma separation systems: A review of the literature. The American Journal of Sports Medicine 2019; 47(2), 479-487.
AJ Sheean, AW Anz and JP Bradley. Platelet-rich plasma: Fundamentals and clinical applications. Arthroscopy 2021; 37(9), 2732-2734.
L Atkinson and F Martin. Intraovarian injection of platelet-rich plasma in assisted reproduction: Too much too soon? Human Reproduction 2021; 36(7), 1737-1750.
K Mautner, GA Malanga, J Smith, B Shiple, V Ibrahim, S Sampson and JE Bowen. A call for a standard classification system for future biologic research: Trationale for new PRP nomenclature. PM&R 2015; 7(4), S53-S59.
JC Riboh, BM Saltzman, AB Yanke, L Fortier and BJ Cole. Effect of leukocyte concentration on the efficacy of platelet-rich plasma in the treatment of knee osteoarthritis. The American Journal of Sports Medicine 2016; 44(3), 792-800.
L Segabinazzi and G Podico. Three manual noncommercial methods to prepare equine platelet-rich plasma. Animals 2021; 11(6), 1478.
ES Machado, FP Soares, RS Yamaguchi, WK Felipone, R Meves, TAC Souza, R Topolniak, JP Caldas, EV Abreu, LS Rabelo Neto, PVS Pinchemel, and M Bredemeier. A simple double-spin closed method for preparing platelet-rich plasma. Cureus 2022; 14(1), e20899.
A Carvalho, AF Ferreira, M Soares, S Santos, P Tomé, J Machado-Simões and AS Pais. Optimization of platelet-rich plasma preparation for regenerative medicine: Comparison of different anticoagulants and resuspension media. Bioengineering 2024; 11(3), 209.
S Muthu, A Krishnan and KR Ramanathan. Standardization and validation of a conventional high yield platelet-rich plasma preparation protocol. Annals of Medicine and Surgery 2022; 82, 104593.
J Choukroun, F Adda, C Schoeffer and A Vervelle. PRF: An opportunity in perio-implantology. Implantodontie 2000; 42, 55-62.
TW Neal, SR Sullivan, S Cannon, W Spresser and T Schlieve. Platelet rich fibrin: A literature review of applications in oral and maxillofacial surgery. Journal of Oral and Maxillofacial Anesthesia 2024; 3(1), 1-10.
V Pavlovic, M Ciric, V Jovanovic, M Trandafilovic and P Stojanovic. Platelet-rich fibrin: Basics of biological actions and protocol modifications. The Open Medicine Journal 2021; 16(1), 446-454.
P Goswami, V Chaudhary, A Arya, R Verma, G Vijayakumar and M Bhavani. Platelet-Rich Fibrin (PRF) and its application in dentistry: A literature review. Journal of Pharmacy and Bioallied Sciences 2024; 16(S1), S5-S7.
K Karimi and H Rockwell. The benefits of platelet-rich fibrin. Facial Plastic Surgery Clinics of North America 2019; 27(3), 331-340.
J Choukroun and S Ghanaati. Reduction of relative centrifugation force within injectable platelet-rich-fibrin (PRF) concentrates advances patients' own inflammatory cells, platelets and growth factors: The first introduction to the low speed centrifugation concept. European Journal of Trauma and Emergency Surgery 2018; 44(1), 87-95.
RJ Miron, H Xu, J Chai, J Wang, S Zheng, M Feng, X Zhang, Y Wei, Y Chen, C Mourão, A Sculean and Y Zhang. Comparison of platelet-rich fibrin (PRF) produced using 3 commercially available centrifuges at both high (~ 700 g) and low (~ 200 g) relative centrifugation forces. Clinical Oral Investigations 2020; 24(3), 1171-1182.
DMD Ehrenfest, NR Pinto, A Pereda, P Jiménez, MD Corso, BS Kang, M Nally, N Lanata, HL Wang and M Quirynen. The impact of the centrifuge characteristics and centrifugation protocols on the cells, growth factors, and fibrin architecture of a leukocyte- and platelet-rich fibrin (L-PRF) clot and membrane. Platelets 2018; 29(2), 171-184.
RFD Santos, JAA Peres and MS Queiroz. Advances in separation methods for the use of platelet-rich fibrin in tissue repair: an integrative review. General Dentistry 2023; 71(2), 65-69.
PR Amable, RB Carias, MV Teixeira, I da Cruz Pacheco, RJ Corrêa do Amaral, JM Granjeiro and R Borojevic. Platelet-rich plasma preparation for regenerative medicine: Optimization and quantification of cytokines and growth factors. Stem Cell Research & Therapy 2013; 4(3), 67.
DA Gutierrez, CA Alfonso, S Jaramillo-Isaza, LA Gomez and AL Muñoz. Evaluation of platelet rich fibrin obtained using different centrifugation parameters as a tool for regenerative medicine. Clinical Laboratory 2021; 67(11), 2462-2468.
K Sneha, AJ Rani, RV Chandra, SP Kumar, RN Jannu and S Muppirala. The G-force conundrum in platelet-rich fibrin generation: Management of a problem hidden in plain sight. Contemporary Clinical Dentistry 2022; 13(2), 150-155.
S Ghanaati, P Booms, A Orlowska, A Kubesch, J Lorenz, J Rutkowski, C Landes, R Sader, C Kirkpatrick and J Choukroun. Advanced platelet-rich fibrin: A new concept for cell-based tissue engineering by means of inflammatory cells. Journal of Oral Implantology 2014; 40(6), 679-689.
M Fujioka-Kobayashi, RJ Miron, M Hernandez, U Kandalam, Y Zhang and J Choukroun. Optimized platelet-rich fibrin with the low-speed concept: Growth factor release, biocompatibility, and cellular response. Journal of Periodontology 2017; 88(1), 112-121.
CF Mourão, H Valiense, ER Melo, NB Mourão and MD Maia. Obtention of injectable platelets rich-fibrin (i-PRF) and its polymerization with bone graft: Technical note. Revista do Colégio Brasileiro de Cirurgiões 2015; 42(6), 421-423.
LF Rodella, G Favero, R Boninsegna, B Buffoli, M Labanca, G Scarì, L Sacco, T Batani and R Rezzani. Growth factors, CD34 positive cells, and fibrin network analysis in concentrated growth factors fraction. Microscopy Research and Technique 2011; 74(8), 772-777.
J Qiao, N An and X Ouyang. Quantification of growth factors in different platelet concentrates. Platelets 2017; 28, 774-778.
H Masuki, T Okudera, T Watanebe, M Suzuki, K Nishiyama, H Okudera, K Nakata, K Uematsu, CY Su and T Kawase. Growth factor and pro-inflammatory cytokine contents in platelet-rich plasma (PRP), plasma rich in growth factors (PRGF), advanced platelet-rich fibrin (A-PRF), and concentrated growth factors (CGF). International Journal of Implant Dentistry 2016; 2(1), 19.
SA Khalifah, M Noureldin and M Eldibany. A comparative study between the effect of platelet rich fibrin and concentrated growth factors on osseointegration of immediate implants (a randomized clinical trial). EKB Journal Management System 2023; 48(2), 39-45.
R Narayanaswamy, BP Patro, N Jeyaraman, P Gangadaran, RL Rajendran, A Nallakumarasamy, M Jeyaraman, P Ramani and BC Ahn. Evolution and clinical advances of platelet-rich fibrin in musculoskeletal regeneration. Bioengineering 2023; 10(1), 58.
A Takahashi, T Tsujino, S Yamaguchi, K Isobe, T Watanabe, Y Kitamura, K Okuda, K Nakata and T Kawase. Distribution of platelets, transforming growth factor-β1, platelet-derived growth factor-BB, vascular endothelial growth factor and matrix metalloprotease-9 in advanced platelet-rich fibrin and concentrated growth factor matrices. Journal of Investigative and Clinical Dentistry 2019; 10(4), e12458.
LH Lei, Y Yu, J Han, D Shi, W Sun, D Zhang and L Chen. Quantification of growth factors in advanced platelet-rich fibrin and concentrated growth factors and their clinical efficiency as adjunctive to the GTR procedure in periodontal intrabony defects. Journal of Periodontology 2020; 91(4), 462-472.
WJ Park, SH Han, NJ Kim and JB Park. 2024, the efficacy of utilizing platelet-rich fibrin for managing periodontal intrabony defects in conjunction with graft material: A systematic review and meta-analysis. Applied Sciences 2024; 14(8), 3371.
OA Al-Aroomi, Y Ou, KA Sakran, H Chen, Y Lin, Y Gao, Q Cai and J Chen. Effectiveness of concentrated growth factors with or without grafting materials in maxillary sinus augmentation: A systematic review. BMC Oral Health 2024; 24(1), 1275.
D Du and Y Liang. A meta-analysis and systematic review of the clinical efficacy and safety of platelet-rich plasma combined with hyaluronic acid (PRP + HA) versus PRP monotherapy for knee osteoarthritis (KOA). Journal of Orthopaedic Surgery and Research. 2025; 20(1), 57.
Y Xu, T Li, L Wang, L Yao, J Li and X Tang. Platelet-rich plasma has better results for long-term functional improvement and pain relief for lateral epicondylitis: A systematic review and meta-analysis of randomized controlled trials. The American Journal of Sports Medicine 2024; 52(10), 2646-2656.
Y Li, H You, C Ou, H Zhu, B Cheng and J Tian. The evolution of 3 generations of platelet concentrates products: A leap from classical formulations to the era of extracellular vesicles. Frontiers in Bioengineering and Biotechnology 2025; 13, 1628565.
R Lopes-Silva, M Santos, ML Sequeira, A Silva, T Antunes, P Valejo-Coelho and M Neiva-Sousa. Platelet-rich plasma effectiveness in treating androgenetic alopecia: A comprehensive evaluation. Cureus 2025; 17(1), e77371.
N Farshidfar, MA Amiri, NE Estrin, P Ahmad, A Sculean and Y Zhang. Platelet-rich plasma (PRP) versus injectable platelet-rich fibrin (i-PRF): A systematic review across all fields of medicine. Periodontology 2000; 2025, 1-31.
J Zhang, W Xu, Y Xiao, D Su, Y He, H Yang, Y Xie, X Wang, RH Xu, S Lei and D Wu. Accurate delivery of mesenchymal stem cell spheroids with platelet-rich fibrin shield: Enhancing survival and repair functions of Sp-MSCs in diabetic wound healing. Advanced Science 2025; 12(25), e2413430.
H Zhou, Q Huang, Y Chen, J Wang and H Jiang. Biological mechanisms and clinical challenges of platelet-rich plasma in chronic musculoskeletal pain: From standardized preparation to multi-omics-guided precision therapy. Journal of Pain Research 2025; 18, 5931-5939.
RV Tey and P Haldankar. Variability in platelet-rich plasma preparations used in regenerative medicine: A comparative analysis. 2022; 2022(1), 3852898.
M Kavitha, S Shakthipriya, D Arunaraj, R Hemamalini, S Velayudham and B Bakthavatchalam. Comparative evaluation of platelet-rich fibrin and concentrated growth factor as scaffolds in regenerative endodontic procedure: A randomized controlled clinical trial. The Journal of Contemporary Dental Practice 2022; 23(12), 1211-1217.
AT Ulusoy, I Turedi, M Cimen and ZC Cehreli. Evaluation of blood clot, platelet‐rich plasma, platelet‐rich fibrin, and platelet pellet as scaffolds in regenerative endodontic treatment: A prospective randomized trial. Journal of Endodontics 2019; 45, 560-566.
L Rossi, M Ranalletta, I Pasqualini, JP Zicaro, MC Paz, P Camino and NS Piuzzi. Substantial variability in platelet-rich plasma composition is based on patient age and baseline platelet count. Arthroscopy, Sports Medicine, and Rehabilitation 2023; 5(3), e853-e858.
J Wu, Y Piao and Q Liu. Platelet-rich plasma-derived extracellular vesicles: A superior alternative in regenerative medicine? Cell Proliferation 2021; 54(12), e13123.
M Mozzati, G Gallesio, M Tumedei and M Del Fabbro. Concentrated growth factors vs. leukocyte-and-platelet-rich fibrin for enhancing postextraction socket healing. A longitudinal comparative study. Applied Sciences 2020; 10(22), 8256.
HC Park, SG Kim, JS Oh, JS You, JS Kim, SC Lim, MA Jeong, JS Kim, C Jung, YS Kwon and H Ji. Early bone formation at a femur defect using CGF and PRF grafts in adult dogs: A comparative study. Implant Dentistry 2016; 25, 387-393.
TH Kim, SH Kim, GK Sándor and YD Kim. Comparison of platelet-rich plasma (PRP), platelet-rich fibrin (PRF), and concentrated growth factor (CGF) in rabbit-skull defect healing. Archives of Oral Biology 2014; 59(5), 550-558.
A Azadi, P Eftekhari-Moghadam, F Atarbashi-Moghadam, P Hazrati, AA Baghban and R Amid. Adjunctive therapy for root coverage with concentrated growth factor versus platelet-rich fibrin membranes: A systematic review and bayesian network meta-analysis. Clinical Oral Investigations 2024; 28(12), 654.
CC Zumarán, MV Parra, SA Olate, EG Fernández, FT Muñoz and ZS Haidar. The 3 R's for platelet-rich fibrin: A "super" tri-dimensional biomaterial for contemporary naturally-guided oro-maxillo-facial soft and hard tissue repair, reconstruction and regeneration. Materials 2018; 11(8), 1293.
A Al-Badran, S Bierbaum and C Wolf-Brandstetter. Does the choice of preparation protocol for platelet-rich fibrin have consequences for healing and alveolar ridge preservation after tooth extraction? A meta-analysis. Journal of Oral and Maxillofacial Surgery : Official Journal of the American Association of Oral and Maxillofacial Surgeons 2023; 11(8), 1293.
K Monisha. Role of bone grafts and Prf/Cgf in different specialities of dentistry - a systematic review. International Journal of Scientific Development and Research 2021; 6(4), 603-607.
ME Kramer and TC Keaney. Systematic review of platelet‐rich plasma (PRP) preparation and composition for the treatment of androgenetic alopecia. Journal of Cosmetic Dermatology 2018; 17, 666 - 671.
P Sebbagh, A Cannone, G Gremion, V Gremeaux and W Raffoul. Current status of PRP manufacturing requirements & european regulatory frameworks: Practical tools for the appropriate implementation of PRP therapies in musculoskeletal regenerative medicine. Bioengineering 2023; 10(3), 292.
M Rath, J Spinnen, LD Kuhrt, E Priglinger, P Seika, D Runge, S Schubring, D Laue, M Wickert, M Erdem, W Ertel and LK Shopperly. Platelet-rich plasma - a comprehensive review of isolation, activation, and application. Acta Biomaterialia 2025; 204, 52-75.
SJ Awan, N Idrees, T Asif, T Munawar, M Munawar and N Naeem. Platelet-rich plasma-derived exosomes as novel frontier in regenerative medicine. Current Cancer Therapy Reviews 2025. https://doi.org/10.2174/0115733947399426250911115018
Y Hou, X Wen, L Zhou, and X Fang. The value of platelet-rich plasma-derived extracellular vesicles in modern medicine. Annals of Medicine 2023; 55(2), 2287705.
N Faramarzi, IK Yazdi, M Nabavinia, A Gemma, A Fanelli, A Caizzone, LM Ptaszek, I Sinha, A Khademhosseini, JN Ruskin and A Tamayol. Patient-specific bioinks for 3D bioprinting of tissue engineering scaffolds. Advanced Healthcare Materials 2018; 7(11), e1701347.
K Yi, Q Li, X Lian, Y Wang and Z Tang. Utilizing 3D bioprinted platelet-rich fibrin-based materials to promote the regeneration of oral soft tissue. Regenerative Biomaterials 2022; 9, rbac021.
Z Li, X Zhang, T Yuan, Y Zhang, C Luo, J Zhang, Y Liu and W Fan. Addition of platelet-rich plasma to silk fibroin hydrogel bioprinting for cartilage regeneration. Tissue Engineering Part A 2020; 26, 886-895.
JM DeLong, RP Russell and AD Mazzocca. Platelet-rich plasma: The PAW classification system. Arthroscopy : The Journal of Arthroscopic & Related Surgery: Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association 2012; 28(7), 998-1009.
T Buchheit, CL Hunt, JS Eldrige, Y Eshraghi and D Souza. Product characteristics should be reported in all biological therapy publications. Regional Anesthesia & Pain Medicine 2022; 47, 449.
S Ren, H Wang, S Ma, J Zhou, J Zhai, Y Zhu, S Chen, S Chen, K Jia, W Xu and Y Zhou. New strategy of personalized tissue regeneration: When autologous platelet concentrates encounter biomaterials. Frontiers in Bioengineering and Biotechnology 2023; 11, 1297357.
A Grzelak, A Hnydka and J Higuchi. Recent achievements in the development of biomaterials improved with platelet concentrates for soft and hard tissue engineering applications. International Journal of Molecular Sciences 2024; 25(3), 1525.
M Niemann, M Ort, L Lauterbach, M Streitz, A Wilhelm, G Grütz, FN Fleckenstein, F Graef, A Blankenstein, S Reinke, U Stöckle, C Perka, GN Duda, S Geißler, T Winkler and T Maleitzke. Individual immune cell and cytokine profiles determine platelet-rich plasma composition. Arthritis Research & Therapy 2023; 25(1), 6.
F Islam, SB Javdan, MR Lewis, JD Craig, H Wu and TL Deans. Programming megakaryocytes to produce engineered platelets for delivering non-native proteins. Communications Biology 2025; 8(1), 638.
T Burnouf, P Strengers and MP Busch. Beyond transfusion: Platelet-derived therapeutic products as a new frontier for blood establishments and transfusion medicine. Vox Sanguinis 2026; 121(2), 114-123.
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






