Comparative Effectiveness of Single, Dual, and Multi-Antibiotic Therapies in Managing Carbapenem-Resistant Enterobacterales: A Systematic Review and Meta-Analysis on Survival Rates
DOI:
https://doi.org/10.48048/tis.2025.9681Keywords:
Antibiotic, Combination therapy, Enterobacteriaceae, Monotherapy, Survival, Antibiotic, Combination therapy, Enterobacterales, Monotherapy, Survival rateAbstract
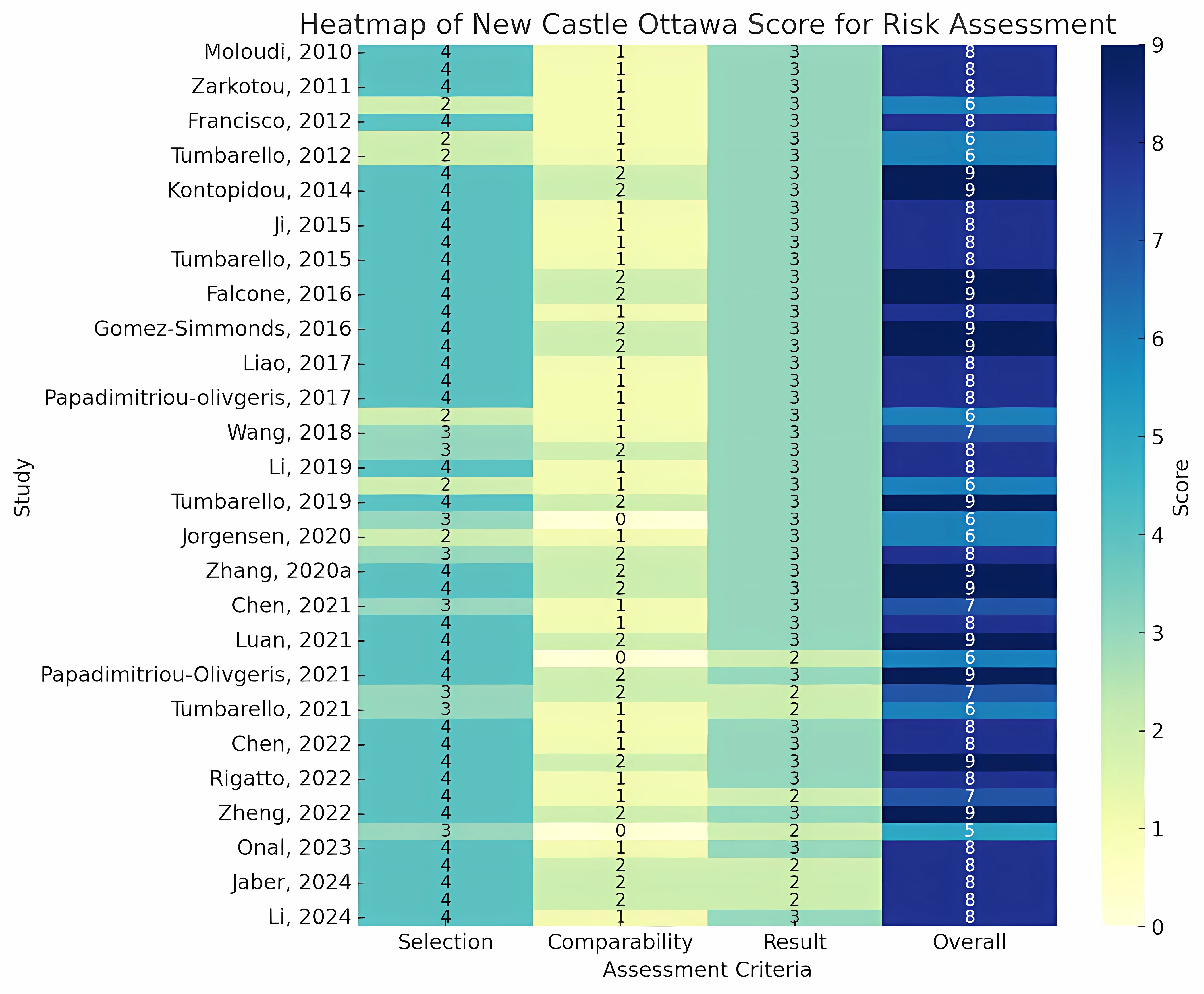
Carbapenem-resistant Enterobacterales (CRE) represent a major global health issue, linked to elevated rates of morbidity and mortality stemming from restricted treatment alternatives. The Gram-negative bacteria, such as Klebsiella pneumoniae and Escherichia coli, are significant contributors to severe infections, including bacteremia, pneumonia, and urinary tract infections. Mechanisms of resistance such as the production of carbapenemases, the action of efflux pumps, and mutations in porins diminish the effectiveness of carbapenems, which are frequently the antibiotics of last resort. In light of this escalating concern, the absence of a universally recognized global guideline for the management of CRE results in diverse treatment strategies. This systematic review and meta-analysis aimed to evaluate the effectiveness of monotherapy, dual therapy, and multi-antibiotic regimens in the treatment of CRE infections. In accordance with established guidelines, data from 5 major databases were analyzed, and the quality of the studies was evaluated using the Newcastle-Ottawa Scale. The findings indicated that combination therapy led to a notable enhancement in survival rates when contrasted with monotherapy (OR = 0.69, 95 % CI 0.62 - 0.78, p < 0.00001). In contrast, no significant difference was found between dual therapy and multi-antibiotic regimens (OR = 1.17, 95 % CI 0.95 - 1.46, p = 0.15). The combination therapy exhibited synergistic effects, improving bacterial eradication while reducing the emergence of resistance. Dual therapy demonstrated superior outcomes when contrasted with multi-antibiotic regimens, presenting lower toxicity risks and enhanced patient adherence. Nonetheless, the absence of stratification considering resistance mechanisms, infection severity, and patient characteristics highlights the necessity for tailored treatment strategies. In conclusion, this study emphasizes the critical necessity for internationally standardized protocols for CRE management to guarantee uniform and effective treatment. Future investigations should concentrate on resistance profiling, assessing the safety and cost-effectiveness of dual and multi-antibiotic regimens, and customizing therapies to individual patient factors to enhance outcomes.
HIGHLIGHTS
- This article presents a systematic review and meta-analysis on the effectiveness of antibiotic strategies in managing carbapenem-resistant Enterobacterales (CRE) infections.
- Combination antibiotic therapy significantly improves patient survival rates compared to monotherapy in CRE infections.
- No statistically significant difference in survival was observed between dual-antibiotic and multi-antibiotic regimens, though dual therapy demonstrated clinical advantages.
- This review suggests that Dual therapy offers reduced toxicity risk and improved patient adherence, making it a safer and more feasible option than multiple-antibiotic regimens.
- The study emphasizes the need for globally standardized CRE treatment protocols and future research that incorporates resistance profiles and patient-specific factors.
GRAPHICAL ABSTRACT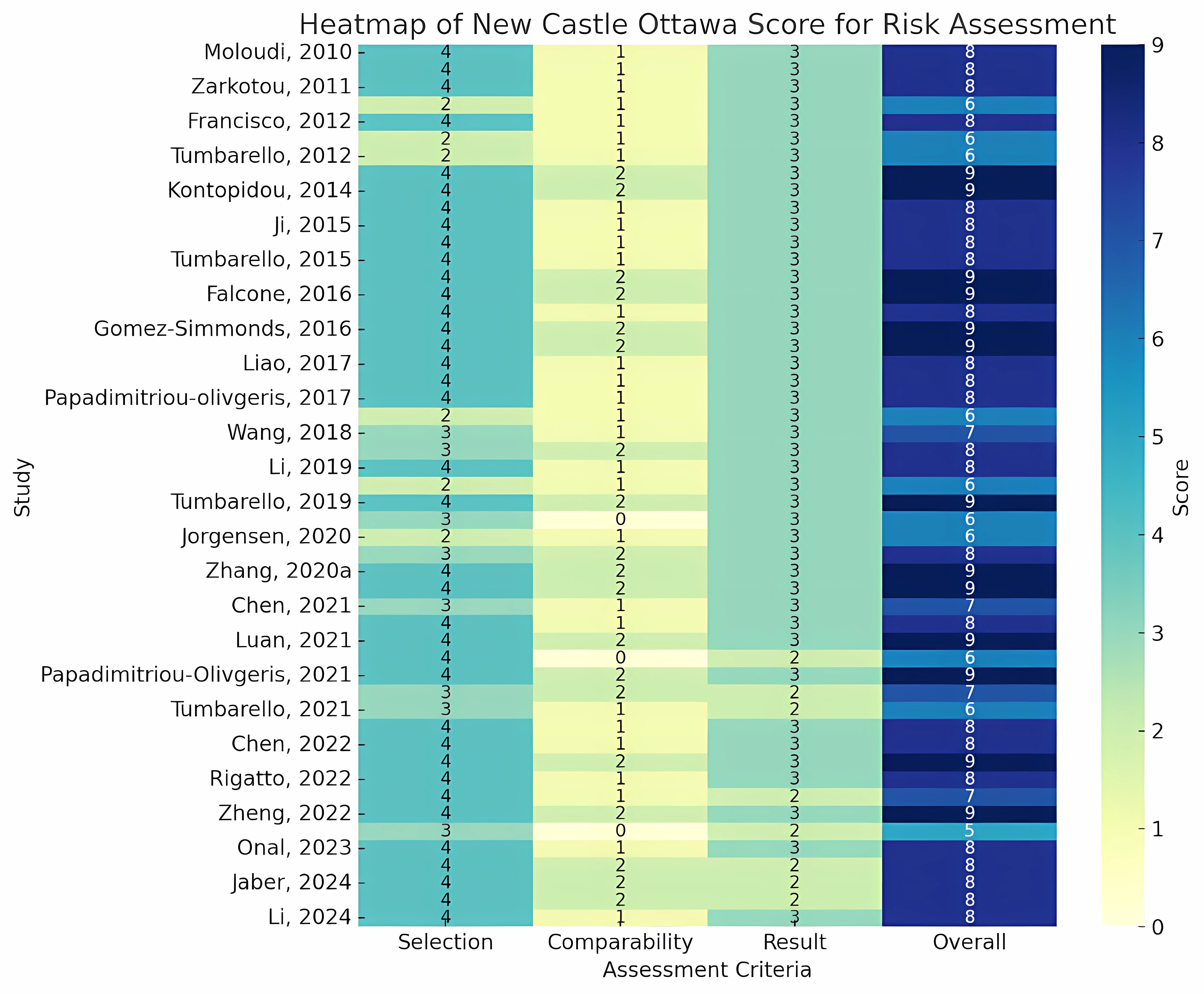
Downloads
References
Y Xu, Y Liu, Y Liu, J Pei, S Yao and C Cheng. Bacteriophage therapy against Enterobacteri-aceae. Virologica Sinica 2015; 30(1), 11-18.
LK Logan and RA Weinstein. The epidemiolo-gy of Carbapenem-resistant Enterobacteri-aceae: The impact and evolution of a global menace. The Journal of Infectious Diseases 2017; 215(S1), S28-S36.
M Shi. Overview of Carbapenem-resistant En-terobacteriaceae. Biomedical Journal of Sci-entific & Technical Research 2021; 39(2), 31248-31251.
B Tuhamize and J Bazira. Carbapenem-resistant Enterobacteriaceae in the livestock, humans and environmental samples around the globe: A systematic review and meta-analysis. Scientific Reports 2024; 14(1), 16333.
MM Mustafai, M Hafeez, S Munawar, S Basha, AA Rabaan, MA Halwani, A Alawfi, A Alshengeti, MA Najim, S Alwarthan, MK Al-Fonaisan, SA Almuthree, M Garout and N Ah-med. Prevalence of Carbapenemase and ex-tended-spectrum β-lactamase producing En-terobacteriaceae: A cross-sectional study. An-tibiotics 2023; 12(1), 1-14.
N Djadjiti, OE Kelechi, OF Nwagbara and S Dane. Prevalence of Enterobacteriaceae among children aged 5-15 from some selected hospitals in Abuja, Nigeria. Journal of Re-search in Medical and Dental Science 2020; 8(2), 33-38.
M Tilahun, Y Kassa, A Gedefie and M Ashagi-re. Emerging carbapenem-resistant Enterobac-teriaceae infection, its epidemiology and nov-el treatment options: A review. Infection and Drug Resistance 2021; 14, 4363-4374.
CC Sheu, YT Chang, SY Lin, YH Chen and PR Hsueh. Infections caused by Carbapenem-resistant Enterobacteriaceae: An update on therapeutic options. Frontiers in Microbiology 2019; 10, 80.
A Martin, K Fahrbach, Q Zhao and T Lodise. Association between carbapenem resistance and mortality among adult, hospitalized pa-tients with serious infections due to Entero-bacteriaceae: Results of a systematic literature review and meta-analysis. Open Forum Infec-tious Diseases 2018; 5(7), ofy150.
R Zhou, X Fang, J Zhang, X Zheng, S Shangguan, S Chen, Y Shen, Z Liu, J Li, R Zhang, J Shen, TR Walsh and Y Wang. Impact of carbapenem resistance on mortality in pa-tients infected with Enterobacteriaceae: A systematic review and meta-analysis. BMJ Open 2021; 11(12), 1-12.
AT Aslan and M Akova. Extended spectrum β-lactamase producing Enterobacteriaceae: Car-bapenem sparing options. Expert Review of An-ti-infective Therapy 2019; 17(12), 969-981.
J Harting. Carbapenem-resistant Enterobacte-riaceae infections: A review of epidemiology and treatment options. The University of Lou-isville Journal of Respiratory Infections 2019; 3(1), 4.
U Amaldi and S Braccini. Present and future of hadrontherapy. AIP Conference Proceedings 2006; 827, 248-261.
EM Trecarichi and M Tumbarello. Therapeutic options for carbapenem-resistant Enterobacte-riaceae infections. Virulence 2017; 8(4), 470-484.
PI Rafailidis and ME Falagas. Options for treat-ing carbapenem-resistant Enterobacteriaceae. Current Opinion in Infectious Diseases 2014; 27(6), 479-483.
E Mouloudi, E Protonotariou, A Zagorianou, E Iosifidis, A Karapanagiotou and T Giasnetsova. Bloodstream infections caused by metallo- β -lactamase/Klebsiella pneumoniae Car-bapenemase - producing K. pneumoniae among intensive care unit patients in Greece: risk fac-tors for infection and impact of type of re-sistance on outcomes. Infection Control & Hospital Epidemiology 2010; 31(12), 1250-1506.
O Zarkotou, S Pournaras, P Tselioti, V Dra-goumanos, V Pitiriga, K Ranellou, A Prekates, K Themeli-Digalaki and A Tsakris. Predictors of mortality in patients with bloodstream in-fections caused by KPC-producing Klebsiella pneumoniae and impact of appropriate antimi-crobial treatment. Clinical Microbiology and Infection 2011; 17(12), 1798-803.
C Navarro‐San Francisco, M Mora‐Rillo, MP Romero‐Gómez, F Moreno‐Ramos, A Rico-Nieto, G Ruiz-Carrascoso, R Gómez-Gil, JR Arribas-López, J Mingorance and JR Paño-Pardo. Bacteraemia due to OXA-48-Carbapenemase-producing Enterobacteri-aceae: A major clinical challenge. Clinical Mi-crobiology and Infection 2013; 19(2), E72-E79.
M Tumbarello, P Viale, C Viscoli, EM Trecar-ichi, F Tumietto, A Marchese, T Spanu, S Am-bretti, F Ginocchio, F Cristini, AR Losito, S Tedeschi, R Cauda and M Bassetti. Predictors of mortality in bloodstream infections caused by Klebsiella pneumoniae Carbapenemase-producing K. pneumoniae: Importance of com-bination therapy. Clinical Infectious Diseases 2012; 55(7), 943-950.
F Kontopidou, H Giamarellou, P Katerelos, A Maragos, I Kioumis, E Trikka-Graphakos, C Valakis and HC Maltezou. Infections caused by carbapenem-resistant Klebsiella pneumoni-ae among patients in intensive care units in Greece: A multi-centre study on clinical out-come and therapeutic options. Clinical Micro-biology and Infection 2014; 20(2), O117-O123.
S Ji, F Lv, X Du, Z Wei, Y Fu, X Mu, Y Jiang and Y Yu. Cefepime combined with amoxicil-lin/clavulanic acid: A new choice for the KPC-producing K. pneumoniae infection. Interna-tional Journal of Infectious Diseases 2015; 38, 108-114.
M Tumbarello, EM Trecarichi, F Giuseppe De Rosa, M Giannella, DR Giacobbe, M Bassetti, AR Losito, M Bartoletti, VD Bono, S Corcione, G Maiuro, S Tedeschi, L Celani, CS Cardellino, T Spanu, A Marchese, S Ambretti, R Cauda, C Viscoli and P Viale. Infections caused by KPC-producing Klebsiella pneumoniae: Differences in therapy and mortality in a multicentre study. Journal of Antimicrobial Chemotherapy 2015; 70(7), 2133-2143.
M Falcone, A Russo, A Iacovelli, G Restuccia, G Ceccarelli, A Giordano, A Farcomeni, A Mo-relli and M Venditti. Predictors of outcome in ICU patients with septic shock caused by Klebsiella pneumoniae carbapenemase-producing K. pneumoniae. Clinical Microbiol-ogy and Infection 2016; 22(5), 444-450.
A Gomez-Simmonds, B Nelson, DP Eiras, A Loo, SG Jenkins, S Whittier, DP Calfee, MJ Satlin, CJ Kubin and EY Furuya. Combination regimens for treatment of carbapenem-resistant Klebsiella pneumoniae bloodstream infections. Antimicrobial Agents and Chemo-therapy 2016; 60(6), 3601-3607.
Y Liao, GH Hu, YF Xu, JP Che, M Luo, HM Zhang, B Peng, XD Yao, JH Zheng and M Liu. Retrospective analysis of fosfomycin combi-national therapy for sepsis caused by car-bapenem-resistant Klebsiella pneumoniae. Ex-perimental and Therapeutic Medicine 2017; 13(3), 1003-1010.
M Papadimitriou-Olivgeris, F Fligou, C Bartzavali, A Zotou, A Spyropoulou and K Koutsileou. Carbapenemase-producing Klebsiella pneumoniae bloodstream infection in critically ill patients: risk factors and pre-dictors of mortality. European Journal of Clin-ical Microbiology & Infectious Diseases 2017; 36(7), 1125-1131.
C Li, Y Li, Z Zhao, Q Liu and B Li. Treatment options and clinical outcomes for carbapenem-resistant Enterobacteriaceae bloodstream in-fection in a Chinese university hospital. Jour-nal of Infection and Public Health 2019; 12(1), 26-31.
M Tumbarello, EM Trecarichi, A Corona, FG De Rosa, M Bassetti, C Mussini, F Menichetti, C Viscoli, C Campoli, M Venditti, A De Gaspe-ri, A Mularoni, C Tascini, G Parruti, C Pallotto, S Sica, E Concia, R Cultrera, G De Pascale, …, P Viale. Efficacy of ceftazidime-avibactam salvage therapy in patients with infections caused by Klebsiella pneumoniae Car-bapenemase-producing K. pneumoniae. Clini-cal Infectious Diseases 2019; 68(3), 355-364.
S Zhang, Z Yang, L Sun, Z Wang, L Sun, J Xu, L Zeng and T Sun. Clinical observation and prognostic analysis of patients with Klebsiella pneumoniae bloodstream infection. Frontiers in Cellular and Infection Microbiology 2020; 10, 577244.
IR Chen, PH Huang, PF Wu, FD Wang and YT Lin. Clinical characteristics and outcomes of 56 patients with pneumonia caused by car-bapenem-resistant Klebsiella pneumoniae. Journal of Global Antimicrobial Resistance 2021; 25, 326-330.
YY Luan, YH Chen, X Li, ZP Zhou, JJ Huang, ZJ Yang, JJ Zhang and M Wu. Clinical charac-teristics and risk factors for critically Ill pa-tients with Carbapenem-resistant Klebsiella pneumoniae (CrKP): A cohort study from de-veloping country. Infection and Drug Re-sistance 2021; 14, 5555-5562.
MH Rigatto, F Ramos, A Barros, S Pedroso, I Guasso, L Gonçalves, P Bergo and AP Zavascki. Double-, single- and none-carbapenem-containing regimens for the treatment of carbapenem-resistant Enterobac-terales (CRE) bloodstream infections: A retro-spective cohort. Journal of Antimicrobial Chemotherapy 2022; 77(11), 3118-3125.
G Zheng, J Cai, L Zhang, D Chen, L Wang, Y Qiu, H Deng, H Bai, X Bian and J He. Ceftazidime/avibactam-based versus polymyx-in b-based therapeutic regimens for the treat-ment of Carbapenem-resistant Klebsiella pneumoniae infection in critically Ill patients: A retrospective cohort study. Infectious Dis-eases and Therapy 2022; 11(5), 1917-1934.
U Önal, NÜ Tüzemen, PK Kaya, R İşçimen, NK Girgin, C Özakın, FŞ Kahveci and H Akalın. Evaluation of the combination treatments with intravenous fosfomycin for carbapenem-resistant Klebsiella pneumoniae. Revista da Associação Médica Brasileira 2023; 69(11), 12-17.
AMR Abu Jaber, B Basgut, AA Hawan, AA Al Shehri, SA AlKahtani, NJ Ahmed and A Abdi. The clinical efficacy of adding ceftazidime/avibactam to standard therapy in treating infections caused by Carbapenem-resistant Klebsiella pneumonia with blaOXA-48-like genes. Antibiotics 2024; 13(3), 265.
J Li, W Wu, M Wu, Z Zhou, J Wang, M Qiu, L Xu, J Ren and X Wu. Clinical and molecular characteristics of patients with bloodstream in-fections caused by KPC and NDM co-producing carbapenem-resistant Klebsiella pneumoniae. Infection and Drug Resistance 2024; 17, 1685-1697.
M Nguyen, GA Eschenauer, M Bryan, K O'Neil, EY Furuya, P Della-Latta and CJ Kubin. Carbapenem-resistant Klebsiella pneumoniae bacteremia: Factors correlated with clinical and microbiologic outcomes. Diagnostic Mi-crobiology and Infectious Disease 2010; 67(2), 180-184.
A Capone, M Giannella, D Fortini, A Giordano, M Meledandri, M Ballardini, M Venditti, E Bordi, D Capozzi, MP Balice, A Tarasi, G Pa-risi, A Lappa, A Carattoli and N Petrosillo. High rate of colistin resistance among patients with carbapenem-resistant Klebsiella pneu-moniae infection accounts for an excess of mortality. Clinical Microbiology and Infection 2013; 19(1), E23-E30.
ZA Qureshi, DL Paterson, BA Potoski, MC Ki-layko, G Sandovsky, E Sordillo, B Polsky, JM Adams-Haduch and Y Doi. Treatment outcome of bacteremia due to KPC-producing Klebsiel-la pneumoniae: Superiority of combination an-timicrobial regimens. Antimicrobial Agents and Chemotherapy 2012; 56(4), 2108-2113.
GL Daikos, S Tsaousi, LS Tzouvelekis, I Any-fantis, M Psichogiou, A Argyropoulou, I Stefa-nou, V Sypsa, V Miriagou, M Nepka, S Georgi-adou, A Markogiannakis, D Goukos and A Skoutelis. Carbapenemase-producing Klebsiel-la pneumoniae bloodstream infections: Lower-ing mortality by antibiotic combination schemes and the role of carbapenems. Antimi-crobial Agents and Chemotherapy 2014; 58(4), 2322-2328.
M Gonzalez-Padilla, J Torre-Cisneros, F Rive-ra-Espinar, A Pontes-Moreno, L López-Cerero, A Pascual, C Natera, M Rodríguez, I Salcedo, F Rodríguez-López, A Rivero and J Rodríguez-Baño. Gentamicin therapy for sepsis due to carbapenem-resistant and colistin-resistant Klebsiella pneumoniae. Journal of Antimicro-bial Chemotherapy 2015; 70(3), 905-913.
MS De Oliveira, DB De Assis, MP Freire, GVB do Prado, AS Machado, E Abdala, LC Pierrotti, C Mangini, L Campos, HHC Filho and AS Lev-in. Treatment of KPC-producing Enterobacte-riaceae: Suboptimal efficacy of polymyxins. Clinical Microbiology and Infection 2015; 21(2), 179.e1-179.e7.
A Díaz, DC Ortiz, M Trujillo, C Garcés, F Jaimes and AV Restrepo. Clinical characteris-tics of carbapenem-resistant Klebsiella pneu-moniae infections in ill and colonized children in Colombia. The Pediatric Infectious Disease Journal 2016; 35(3), 237-241.
A Ghafur, V Devarajan, T Raja, J Easow, MA Raja, S Sreenivas, B Ramakrishnan, SG Raman, D Devaprasad, B Venkatachalam and R Nim-magadda. Monotherapy versus combination therapy against carbapenem-resistant Gram-negative bacteria: A retrospective observa-tional study. Indian Journal of Cancer 2016; 53(4), 592-594.
B Gutiérrez-Gutiérrez, E Salamanca, M de Cueto, PR Hsueh, P Viale, JR Paño-Pardo, M Venditti, M Tumbarello, G Daikos, R Cantón, Y Doi, FF Tuon, I Karaiskos, E Pérez-Nadales, MJ Schwaber, ÖK Azap, M Souli, E Roilides, S Pournaras, …, J Rodríguez-Baño. Effect of ap-propriate combination therapy on mortality of patients with bloodstream infections due to carbapenemase-producing Enterobacteriaceae (INCREMENT): A retrospective cohort study. The Lancet Infectious Diseases 2017; 17(7), 726-734.
I Machuca, B Gutiérrez-Gutiérrez, I Gracia-Ahufinger, FR Espinar, Á Cano, J Guzmán-Puche, E Pérez-Nadales, C Natera, M Rodríguez, R León, JJ Castón, F Rodríguez-López, J Rodríguez-Baño and J Torre-Cisneros. Mortality associated with bacteremia due to colistin-resistant Klebsiella pneumoniae with high-level meropenem resistance: im-portance of combination therapy without col-istin and carbapenems. Antimicrobial Agents and Chemotherapy 2017; 61(8), e00406-17.
A Sousa, MT Pérez-Rodríguez, A Soto, L Rodríguez, A Pérez-Landeiro, L Martínez-Lamas, A Nodar and M Crespo. Effectiveness of ceftazidime/avibactam as salvage therapy for treatment of infections due to OXA-48 car-bapenemase-producing Enterobacteriaceae. Journal of Antimicrobial Chemotherapy 2018; 73(11), 3170-3175.
X Wang, Q Wang, B Cao, S Sun, Y Zhang, B Gu, B Li, K Liao, F Zhao, L Jin, C Jin, C Yang, F Pei, Z Zhang and H Wang. Retrospective ob-servational study from a Chinese network of the impact of combination therapy versus monotherapy on. Antimicrobial Agents and Chemotherapy 2018; 63(1), e01511-e01518.
L Brescini, G Morroni, C Valeriani, S Castellet-ti, M Mingoia, S Simoni, A Masucci, R Montal-ti, M Vivarelli, A Giacometti and F Barchiesi. Clinical and epidemiological characteristics of KPC-producing Klebsiella pneumoniae from bloodstream infections in a tertiary referral center in Italy. BMC Infectious Diseases 2019; 19(1), 1-9.
U Önal, OR Sipahi, H Pullukçu, T Yamazhan, B Arda, S Ulusoy, Ş Aydemir and MI Taşbakan. Retrospective evaluation of the patients with urinary tract infections due to carbapenemase producing Enterobacteriaceae. Journal of Chemotherapy 2019; 32(1), 15-20.
A Gorgulho, AM Grilo, M de Figueiredo and J Selada. Carbapenemase- producing enterobac-teriaceae in a portuguese hospital - a 5-year retrospective study. Germs 2020; 10(2), 95-103.
SCJ Jorgensen, TD Trinh, EJ Zasowski, AM Lagnf, S Bhatia, SM Melvin, SP Simon, JR Rosenberg, ME Steed, SJ Estrada, T Morrisette, SL Davis and MJ Rybak. Evaluation of the IN-CREMENT-CPE, Pitt bacteremia and qPitt scores in patients with carbapenem-resistant Enterobacteriaceae infections treated with ceftazidime - avibactam. Infectious Diseases and Therapy 2020; 9(2), 291-304.
NY Lee, CS Tsai, LS Syue, PL Chen, CW Li, MC Li and WC Ko. Treatment outcome of bac-teremia due to non-carbapenemase producing carbapenem-resistant Klebsiella pneumoniae bacteremia: Role of carbapenem combination therapy. Clinical Therapeutics 2020; 42(3), e33-e44.
G Zhang, M Zhang, F Sun, J Zhou, Y Wang, D Zhu, Z Chen, Q Chen, Q Chang, H Liu, W Chai and H Pan. Epidemiology, mortality and risk factors for patients with K. pneumoniae blood-stream infections: Clinical impact of car-bapenem resistance in a tertiary university teaching hospital of Beijing. Journal of Infec-tion and Public Health 2020; 13(11), 1710-1714.
E Eren, A Ulu-Kılıç, Z Türe, F Cevahir, H Kılıç and E Alp-Meşe. Risk factors of mortality in patients with bloodstream infections due to carbapenem resistant Klebsiella pneumonia. Klimik Dergisi 2021; 34(1), 56-60.
V Nagvekar, A Shah, VP Unadkat, A Chavan, R Kohli, S Hodgar, A Ashpalia, N Patil and R Kamble. Clinical outcome of patients on ceftazidime-avibactam and combination thera-py in carbapenem-resistant Enterobacteri-aceae. Indian Journal of Critical Care Medi-cine 2021; 25(7), 780-784.
M Papadimitriou-Olivgeris, C Bartzavali, A Georgakopoulou, F Kolonitsiou, C Pa-pamichail, I Spiliopoulou, M Christofidou, F Fligou and M Marangos. Mortality of pandrug-resistant Klebsiella pneumoniae bloodstream infections in critically ill patients: A retrospec-tive cohort of 115 episodes. Antibiotics 2021; 10(1), 76.
WC Tsai, LS Syue, WC Ko, CL Lo and NY Lee. Antimicrobial treatment of monomicrobial phenotypic carbapenem-resistant Klebsiella pneumoniae bacteremia: Two are better than one. Journal of Microbiology, Immunology and Infection 2021; 55(6), 1219-1228.
M Tumbarello, F Raffaelli, M Giannella, E Mantengoli, A Mularoni, M Venditti, FG De Rosa, L Sarmati, M Bassetti, G Brindicci, M Rossi, R Luzzati, PA Grossi, A Corona, A Ca-pone, M Falcone, C Mussini, EM Trecarichi, A Cascio, …, P Viale. Ceftazidime-avibactam use for Klebsiella pneumoniae carbapenemase-producing K. pneumoniae infections: A retro-spective observational multicenter study. Clin-ical Infectious Diseases 2021; 73(9), 1664-1676.
AT Aslan, E Kırbaş, B Sancak, ES Tanrıverdi, B Otlu, NC Gürsoy, YA Yılmaz, A Tozluyurt, Ü Liste, A Bıçakcıgil, G Hazırolan, O Dağ, GS Güven and M Akova. A retrospective observa-tional cohort study of the clinical epidemiolo-gy of bloodstream infections due to car-bapenem-resistant Klebsiella pneumoniae in an OXA-48 endemic setting. International Journal of Antimicrobial Agents 2022; 59(4), 106554.
J Chen, H Ma, X Huang, Y Cui, W Peng, F Zhu, S Ma, M Rao, P Zhang, H Yang, L Su, R Niu and P Pan. Risk factors and mortality of car-bapenem-resistant Klebsiella pneumoniae bloodstream infection in a tertiary-care hospi-tal in China: An 8-year retrospective study. Antimicrobial Resistance & Infection Control 2022; 11(1), 161.
CL Luterbach, H Qiu, PO Hanafin, R Sharma, J Piscitelli, FC Lin, J Ilomaki, E Cober, RA Sala-ta, RC Kalayjian, RR Watkins, Y Doi, CB Landersdorfer, D van Duin and GG Rao. A sys-tems-based analysis of mono- and combination therapy for carbapenem-resistant Klebsiella pneumoniae bloodstream infections. Antimi-crobial Resistance & Infection Control 2022; 66(10), e00591-22.
M Tumbarello, F Raffaelli, A Cascio, M Fal-cone, L Signorini, C Mussini, FG De Rosa, AR Losito, G De Pascale, R Pascale, DR Giacobbe, A Oliva, A Farese, P Morelli, G Tiseo, M Mes-chiari, PD Giacomo, F Montagnani and M Fab-biani. Compassionate use of mero-penem/vaborbactam for infections caused by KPC-producing Klebsiella pneumoniae: A multicentre study. JAC-Antimicrobial Re-sistance 2022; 4(1), dlac022.
J Cheng, D Zhao, X Ma and J Li. Molecular epidemiology, risk factors, and outcomes of carbapenem-resistant Klebsiella pneumoniae infection in a tertiary hospital in eastern Chi-na: For a retrospective study conducted over 4 years. Frontiers in Microbiology 2023; 14, 1223138.
L Zhang, S Zhen, Y Shen, T Zhang, J Wang, J Li, Q Lin, Z Xiao, Y Zheng, E Jiang, M Han and S Feng. Bloodstream infections due to car-bapenem-resistant Enterobacteriaceae in he-matological patients: Assessment of risk fac-tors for mortality and treatment options. An-nals of Clinical Microbiology and Antimicro-bials 2023; 22(1), 41.
Katip, A Rayanakorn, P Oberdorfer, P Ta-ruangsri, T Nampuan and S Okonogi. Compara-tive effectiveness and mortality of colistin monotherapy versus colistin-fosfomycin com-bination therapy for the treatment of car-bapenem-resistant Enterobacteriaceae (CRE) infections: A propensity score analysis. Jour-nal of Infection and Public Health 2024; 17(5), 727-734.
Y Leibovici-Weissman, N Tau and D Yahav. Bloodstream infections in the elderly: What is the real goal? Aging Clinical and Experimental Research 2021; 33(4), 1101-1112.
YC Chen, IT Tsai, CH Lai, KH Lin and YC Hsu. Risk factors and outcomes of community-acquired carbapenem-resistant Klebsiella pneumoniae infection in elderly patients. Anti-biotics 2024; 13(3), 282.
WG Melsen, MCJ Bootsma, MM Rovers and MJM Bonten. The effects of clinical and statis-tical heterogeneity on the predictive values of results from meta-analyses. Clinical Microbi-ology and Infection 2014; 20(2), 123-129.
N Petrosillo, E Ioannidou and ME Falagas. Col-istin monotherapy vs. combination therapy: Evidence from microbiological, animal and clinical studies. Clinical Microbiology and In-fection 2008; 14(9), 816-827.
A Schmid, A Wolfensberger, J Nemeth, PW Schreiber, H Sax and SP Kuster. Monotherapy versus combination therapy for multidrug-resistant Gram-negative infections: Systematic review and meta-analysis. Scientific Reports 2019; 9(1), 15290.
P Poulikakos, GS Tansarli and ME Falagas. Combination antibiotic treatment versus monotherapy for multidrug-resistant, exten-sively drug-resistant, and pandrug-resistant Acinetobacter infections: A systematic review. European Journal of Clinical Microbiology and Infectious Diseases 2014; 33, 1675-1685.
GJ Sullivan, NN Delgado, R Maharjan and AK Cain. How antibiotics work together: Molecu-lar mechanisms behind combination therapy. Current Opinion in Microbiology 2020; 57, 31-40.
Z Gounani, MA Asadollahi, JN Pedersen, J Lyngsø, JS Pedersen, A Arpanaei and RL Mey-er. Mesoporous silica nanoparticles carrying multiple antibiotics provide enhanced syner-gistic effect and improved biocompatibility. Colloids Surfaces B Biointerfaces 2019; 175, 498-508.
I Baltas, T Stockdale, M Tausan, A Kashif, J Anwar, J Anvar, E Koutoumanou, D Sidebot-tom, V Garcia-Arias, M Wright and J Democra-tis. Impact of antibiotic timing on mortality from Gram-negative bacteraemia in an English district general hospital: The importance of getting it right every time. Journal of Antimi-crobial Chemotherapy 2021; 76(3), 813-819.
YF Zhou, P Liu, CJ Zhang, XP Liao, J Sun and YH Liu. Colistin combined with tigecycline: A promising alternative strategy to combat Esch-erichia coli harboring blaNDM-5 and mcr-1. Frontiers in Microbiology 2020; 10, 2957.
X Cai, Z Yang, J Dai, K Chen, L Zhang, W Ni, C Wei and J Cui. Pharmacodynamics of tigecy-cline alone and in combination with colistin against clinical isolates of multidrug-resistant Acinetobacter baumannii in an in vitro phar-macodynamic model. International Journal of Antimicrobial Agents 2017; 49(5), 609-616.
S Fergadaki, G Renieris, N Machairas, L Sabra-cos, DI Droggiti, E Misiakos and EJ Giama-rellos-Bourboulis. Efficacy of tigecycline alone or in combination for experimental in-fections by KPC carbapenemase-producing Klebsiella pneumoniae. International Journal of Antimicrobial Agents 2021; 58(3), 106384.
AA Agyeman, PJ Bergen, GG Rao, RL Nation and CB Landersdorfer. A systematic review and meta-analysis of treatment outcomes fol-lowing antibiotic therapy among patients with carbapenem-resistant Klebsiella pneumoniae infections. International Journal of Antimi-crobial Agents 2020; 55(1), 105833.
J Wang, Y Pan, J Shen and Y Xu. The efficacy and safety of tigecycline for the treatment of bloodstream infections: A systematic review and meta-analysis. Annals of Clinical Microbi-ology and Antimicrobials 2017; 16, 1-10.
IL Cheng, YH Chen, CC Lai and HJ Tang. In-travenous colistin monotherapy versus combi-nation therapy against carbapenem-resistant gram-negative bacteria infections: Meta-analysis of randomized controlled trials. Jour-nal of Clinical Medicine 2018; 7(8), 208.
Y Luan, K Chen, J Zhao and L Cheng. Compar-ative study on synergistic toxicity of enroflox-acin combined with three antibiotics on prolif-eration of THLE-2 cell. Antibiotics 2022; 11(3), 394.
F Shahbazi, L Shojaei, F Farvadi and S Kadi-varian. Antimicrobial safety considerations in critically ill patients: Part II: Focused on anti-microbial toxicities. Expert Review of Clinical Pharmacology 2022; 15(5), 563-573.
Y Wang, C Gao, Z Qu and M Li. The combined toxicity of binary mixtures of antibiotics against the cyanobacterium Microcystis is dose-dependent: Insight from a theoretical nonlinear combined toxicity assessment meth-od. Environmental Science and Pollution Re-search 2022; 29(8), 1-13.
S Bangalore, G Kamalakkannan, S Parkar and FH Messerli. Fixed-dose combinations im-prove medication compliance: A meta-analysis. American Journal of Medicine 2007; 120(8), 713-719.
B Tepekule, H Uecker, I Derungs, A Frenoy and S Bonhoeffer. Modeling antibiotic treat-ment in hospitals: A systematic approach shows benefits of combination therapy over cycling, mixing, and mono-drug therapies. PLoS Computational Biology 2017; 13(9), e1005745.
C Nyhoegen, S Bonhoeffer and H Uecker. The many dimensions of combination therapy: How to combine antibiotics to limit resistance evolution. Evolutionary Applications 2024; 17(8), 1-25.
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






