Sex-Based Differences in Gingival Inflammatory Responses to Porphyromonas gingivalis in Male and Female Rats
DOI:
https://doi.org/10.48048/tis.2025.9479Keywords:
Female rats, Lymphocytes, Macrophage, Male rats, Neutrophils, Porphyromonas gingivalis, Sex, Tumor necrosis factor-alphaAbstract
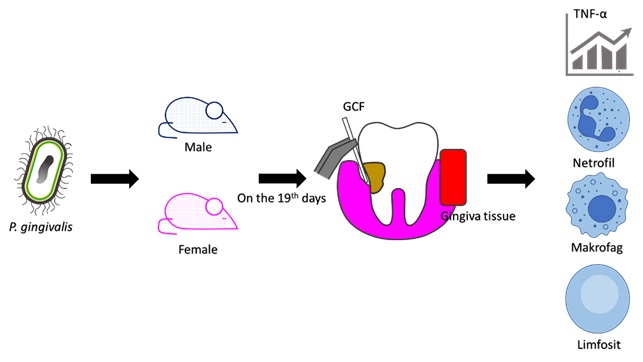
Periodontitis is defined as the inflammation of periodontal tissue. It is primarily caused by plaque bacteria, with Porphyromonas gingivalis being one of the most predominant bacteria. The inflammatory response to P. gingivalis varies by sex, as evidenced by higher serum titers in females than in males. This study aimed to compare the inflammatory responses in the gingiva of female and male rats following injection with P. gingivalis. The study was experimental laboratory using post-test control group design. Both male and female rats received injections of 2.109 cells/mL of P. gingivalis every 3 days over 19 days. The injections were into the distobuccal and distolingual gingival sulcus of the mandibular first molar. On the 19 days, tumor necrosis factor-alpha (TNF-α) levels of gingival fluid were measured using ELISA methods. Then, the rats were euthanized and removed the mandible. The number of leukocytes in the mandibular gingival tissue was assessed histologically using hematoxylin eosin staining. All of data were analyzed by Independent T-Test (p < 0.0 %). The findings revealed that the TNF-α levels in the gingival crevicular fluid of female rats (161.14 ng/mL) were significantly 1.5 times higher than male rats (109.57 ng/mL) after P. gingivalis injection (p < 0.05). The numbers of neutrophils and macrophages in female rats (neutrophils = 35.57 cells and macrophages = 13.71 cells) were significantly higher than those in male rats (neutrophils = 30.14 cells and macrophages = 8.43) (p < 0.05). However, the lymphocyte count was insignificantly comparable between sexes following injection (females = 22.24 cells and males = 22 cells) (p > 0.05). Sex differences might influence the immune response to P. gingivalis infection, with females exhibiting a stronger response characterized by increased leukocyte infiltration and TNF-α level than males. After injections of P. gingivalis, the inflammatory response observed in female rats was notably greater than that in male rats.
HIGHLIGHTS
- Periodontitis is a chronic inflammatory disease that affects periodontal tissues, and Porphyromonas gingivalis is the main pathogen involved with this condition.
- The inflammatory response to gingivalis differs according to sex, regardless of smoking habit or existing systemic diseases.
- Female rats demonstrated a more intense inflammatory response than male rats following gingivalis infection.
- This study emphasizes the importance of recognizing sex differences in the biological mechanisms underlying the development of periodontal diseases.
- Women need to prioritize maintaining oral health, as they appear to be more susceptible than men to infections caused by periodontal pathogens.
GRAPHICAL ABSTRACT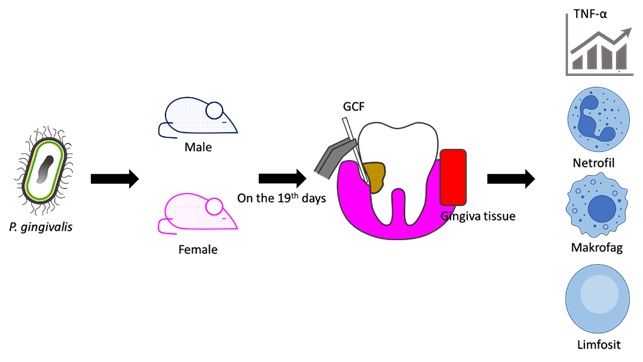
Downloads
References
GG Nascimento, S Alves-Costa and M Romandini. Burden of severe periodontitis and edentulism in 2021, with projections up to 2050: The global burden of disease 2021 study. Journal of Periodontal Research 2024; 59(5), 823-867.
MX Chen, YJ Zhong, QQ Dong, HM Wong and YF Wen. Global, regional, and national burden of severe periodontitis, 1990 - 2019: An analysis of the global burden of disease study 2019. Journal of Clinical Periodontology 2021; 48(9), 1165-1188.
Kementerian Kesehatan Republik Indonesia. Laporan Nasional: RISKESDAS 2018. Badan Penelitian dan Pengembangan Kesehatan, Jakarta, Indonesia, 2019, p. 202-204.
A Susanto, D Carolina, A Amaliya, IS Pribadi and A Miranda. Periodontal health status and treatment needs of the community in Indonesia: A cross sectional study. Journal of International Oral Health 2020; 12(2), 114-119.
R Sawitri, SLC Masulili and R Lessang. Analysis of periodontal disease by age, gender, and smoking. Journal of International Dental and Medical Research 2018; 11(3), 1040-1044.
P Wulandari, D Widkaja, AH Nasution, A Syahputra and G Gabrina. Association between age, gender and education level with the severity of periodontitis in pre-elderly and elderly patients. Dental Journal 2022; 55(1), 16-20.
YN Alawaji, A Alshammari, N Mostafa, RM Carvalho and J Aleksejuniene. Periodontal disease prevalence, extent, and risk associations in untreated individuals. Clinical and Experimental Dental Research 2022; 8(1), 380-394.
NI Ummah, P Soesilawati, SJMR Syahnia, NL Arini and AS Oki. The Role of porphyromonas gingivalis in oral biofilm: Pathophysiology in chronic periodontitis. Research Journal of Pharmacy and Technology 2023; 16(4), 1754-1760.
Y Zhao, Y Zhou, J Zhao, Y Feng, ZR Gao, Q Ye, Q Liu, Y Chen, S Zhang, L Tan, MA Dusenge, J Hu, Y Feng 1, F Yan and Y Guo. Sex variations in the oral microbiomes of youths with severe periodontitis. Journal of Immunology Research 2021; 2021(1), 8124593.
A Chopra, SG Bhat and K Sivaraman. Porphyromonas gingivalis adopts intricate and unique molecular mechanisms to survive and persist within the host: A critical update. Journal of Oral Microbiology 2020; 12(1), 1801090.
A Chopra, Y Shiheido-Watanabe and J Eberhard. Editorial: Porphyromonas gingivalis: molecular mechanisms of invasion, immune evasion, and dysbiosis. Frontiers in Cellular and Infection Microbiology 2023; 13, 1289103.
PG Kulkarni, S Gosavi, PB Haricharan, S Malgikar, DP Mudrakola, N Turagam, and KK Ealla. Molecular detection of porphyromonas gingivalis in chronic periodontitis patients. The Journal of Contemporary Dental Practice 2018; 19(8), 992-996.
GD Tribble, JE Kerr and B Wang. Genetic diversity in the oral pathogen porphyromonas gingivalis: Molecular mechanisms and biological consequences. Futur Microbiology 2013; 8(5), 607-620.
RI Roestamadji, U Tedjosasongko, N Indrastie, I Diyatri, MDC Surboyo, SM Sudarmo, B Santoso and N Takahashi. Quantification of porphyromonas gingivalis bacteria in final trimester of pregnant women according to their oral health status. European Journal of General Dentistry 2022; 11(3), 201-207.
C Champagne, N Yoshinari, JA Oetjen, EL Riche, JD Beck and S Offenbacher. Gender differences in systemic inflammation and atheroma formation following porphyromonas gingivalis infection in heterozygous apolipoprotein E-deficient mice. Journal of Periodontal Research 2009; 44(5), 569-577.
LM Tebloeva, ZE Revazova, KG Fabrikant, LA Dmitrieva and KG Gurevich. Differences in immune response to Porphyromonas gingivalis. The Journal of Contemporary Dental Practice 2015; 15(5), 573-575.
KJ Demirel, AN Guimaraes and I Demirel. Effects of estradiol on the virulence traits of porphyromonas gingivalis. Scientific Reports 2022; 12(1), 13881.
X Duan, RC Gleason, F Li, KB Hosur, X Duan, D Huang, H Wang, G Hajishenagllis and S Liang. Sex dimorphism in periodontitis in animal models. Journal of Periodontal Research 2016. 2016; 51(2), 196-202.
M Furuta, Y Shimazaki, S Tanaka, K Takeuchi, Y Shibata, T Takeshita, F Nishimura and Y yamashita. Gender-specific associations of serum antibody to Porphyromonas gingivalis and inflammatory markers. BioMed Research International 2015; 2015(1), 897971.
RB Johnson and JC Wikle. Sex differences in inflammatory and apoptotic signaling molecules in normal and diseased human gingiva. Journal of Periodontology 2014; 85(11), 1612-1619.
P Sengupta. The laboratory rat : Relating its age with human’s. International Journal of Preventive Medicine 2013; 4(6), 624-30.
AW Suci-Dharmayanti, AN Anjani, ATW Handayani, Z Hamzah, Z Meilawaty, M Novita, M Syafriaddi and ADP Shita. Superoxide dismutase expression in the ovaries of periodontitis animal models induced by porphyromonas gingivalis and treated with cassava leaves extract. Annals of Dentistry University of Malaya 2021; 28, 40-46.
AWS Dharmayanti, Z Meilawaty, T Ermawati, AM Putradjaka and Z Hamzah. Effect of ovarian dysfunction induced ovariectomy and Porphyromonas gingivalis induction to risk of metabolic syndrome: In vivo study. Brazilian Dental Science 2024; 27(1), e3880.
A Wulan, S Dharmayanti and B Kusumawardani. Deoxypyridinoline and mineral levels in gingival crevicular fluid as disorder indicators of menopausal women with periodontal disease. Dental Journal: Majalah Kedokteran Gigi 2017; 50(32), 131-137.
AW Suci-Dharmayanti, R Budirahardjo and B Febrianto. The Effect of porphyromonas gingivalis infection on menopause to the mechanical strength of the mandible and femur. Odonto : Dental Journal 2022; 9(1), 119-129.
DL Yuliana, YP Dachlan and H Arwati. Effect of Tumor Necrosis Factor Alpha (Tnf-A) And Interleukin-10 (II-10) Levels of Aggressive Periodontitis In Rats (Rattus Norvegicus) Induced by Agrregitibacter Actinomycetemcomitans. In: Proceedings of the 2nd International Conference Postgraduate School, Sarabaya, Indonesia, 2018.
H Taguchi, Y Aono, T Kawato, M Asano, N Shimizu and T Saigusa. Intragingival injection of Porphyromonas gingivalis-derived lipopoly saccharide induces a transient increase in gingival tumour necrosis factor-α, but not interleukin-6, in anaesthetised rats. International Journal of Oral Science 2015; 7(3), 155-160.
NS Romero-Castro, M Vazquez-Villamar, JF Munoz-Valle, S Reyes-Fernandez, VO Serna-Radilla, S Garcia-Arellano and N Castro-Alarcon. Relationship between TNF-α, MMP-8, and MMP-9 levels in gingival crevicular fluid and the subgingival microbiota in periodontal disease. Odontology 2020; 108(1), 25-33.
YC Rahayu, EM Setiawatie, RP Rahayu, NN Sakinah, B Kusumawardani, A Gunadi and BH Ryandhana. Effects of cocoa pod husk extract (theobroma cacao L.) on alveolar bone in experimental periodontitis rats. Trends in Sciences 2023; 20(6), 6535.
M Plasay and L Muslimin. Melittin, a potential natural toxin with anticancer properties: Regulating IL-1β, COX-2 and TNF-α in human colorectal cancer cells WiDr. Trends in Sciences 2024; 21(4), 7424.
JL Bain, SR Lester, WD Henry, CM Bishop, AA Turnage, JP Naftel, and RB Johnson. Comparative gender differences in local and systemic concentrations of pro-inflammatory cytokines in rats with experimental periodontitis. Journal of Periodontal Research 2009; 44(1), 133-140.
JJ Yu, MJ Ruddy, HR Conti, K Boonanantanasarn and SL Gaffen. The interleukin-17 receptor plays a gender-dependent role in host protection against porphyromonas gingivalis -induced periodontal bone loss. Infection and Immunity 2008; 76(9), 4206-4213.
V Grover, A Jain, A Kapoor, R Malhotra and GS Chahal. The gender bender effect in periodontal immune response. Endocrine, Metabolic & Immune Disorders - Drug Targets 2016; 16(1), 12-20.
R Teimouri, S Amini and M Guagliano. Analytical modeling of ultrasonic surface burnishing process: Evaluation of residual stress field distribution and strip deflection. Materials Science and Engineering: A 2019; 747, 208-224.
SN Ulfita, AWS Dharmayanti and B Yuwono. Effect of porphyromonas gingivalis infection on leukocyte count in rat model of diabetes mellitus. Majalah Kedokteran Gigi Indonesia 2018; 4(1), 27-35.
AW Suci-Dharmayanti, T Ermawati and B Febrianto. Ovarian failure affected leukocytes profile in peripheral blood and gingival fluid ( In vivo study ). In: Proceedings of the 2nd International Conference in Health Sciences, Central Java, Indonesia. 2017.
I Olsen and G Hajishengallis. Major neutrophil functions subverted by Porphyromonas gingivalis. Journal of Oral Microbiology 2016; 8(1), 30936.
PL Yun, AA Decarlo and N Hunter. Gingipains of porphyromonas gingivalis modulate leukocyte adhesion molecule expression induced in human endothelial cells by ligation of CD99. Infection and Immunity 2006; 74(3), 1661-1672.
M Sochalska and J Potempa. Manipulation of neutrophils by porphyromonas gingivalis in the development of periodontitis. Frontiers in Cellular and Infection Microbiology 2017; 7, 197.
A Cekici, A Kantarci, H Hasturk and TEV Dyk. Inflammatory and immune pathways in the pathogenesis of periodontal disease. Periodontology 2000 2014; 64(1), 57-80.
YC Rahayu, AWS Dharmayanti, YE Putri and A Irmawati. The analysis of proanthocyanidins cacao peel extract (Theobroma cacao L.) potential on the expression of TNF-α and COX-2 on periodontitis rat. International Journal of Pharmaceutical Research 2020; 12(4), 4337-4343.
E Ioannidou. The sex and gender intersection in chronic periodontitis. Frontiers in Public Health 2017; 5, 189.
HJ Shiau, ME Aichelmann-Reidy and MA Reynolds. Influence of sex steroids on inflammation and bone metabolism. Periodontology 2000 2014; 64(1), 81-94.
PC Ulloa, BP Krom and MHVD Veen. Sex Steroid hormones as a balancing factor in oral host microbiome interactions. Frontiers in Cellular and Infection Microbiology 2021; 11, 714229.
TT Tavakoli, F Gholami, H Huang, PF Gonçalves, A Villasante-Tezanos, I Aukhil, RCGD Oliveira, N Hovencamp, S Wallet, E Ioannidou and LM Shaddox. Gender differences in immunological response of African-American juveniles with Grade C molar incisor pattern periodontitis. Journal of Periodontology 2022; 93(3), 392-402.
MS Valerio and KL Kirkwood. Sexual dimorphism in immunity to oral bacterial diseases: Intersection of neutrophil and osteoclast pathobiology. Journal of Dental Research 2018; 97(13), 1416-1423.
J Vag, TL Nagy and B Mikecs. Sex-related differences in endothelium-dependent vasodilation of human gingiva. BMC Oral Health 2022; 22(1), 177.
JP Steffens, BS Herrera, LS Coimbra, DN Stephens, CR Jr, LC Spolidorio, A Kantarci and TEV Dyke. Testosterone regulates bone response to inflammation. Hormone and Metabolic Research 2014; 46(3), 193-200.
CC Villar, MC Sloniak, JBD Assis, RC Porto and GA Romito. Unveiling sex-disparities and the impact of gender-affirming hormone therapy on periodontal health. Frontiers in Dental Medicine 2024; 5, 1430193.
S Kovats. Estrogen receptors regulate innate immune cells and signaling pathways. Cell Immunology 2015; 294(2), 63-69.
P Jitprasertwong, N Charadram, S Kumphune, S Pongcharoen and S Sirisinha. Female sex hormones modulate Porphyromonas gingivalis lipopolysaccharide-induced Toll-like receptor signaling in primary human monocytes. Journal of Periodontal Research 2016; 51(3), 395-406.
J Yan, JM Green, R Hull, JD O’Sullivan, RD Henderson, SJ Read and RA McCombe. The effect of ageing on human lymphocyte subsets: Comparison of males and females. Immunity & Ageing 2010; 7, 4.
R Pellegrino, R Paganelli, AD Iorio, S Bandinelli, A Moretti, G Iolascon, E Sparvieri, D Tarantino and L Ferrucci . Temporal trends, sex differences, and age-related disease influence in neutrophil, lymphocyte count and neutrophil to lymphocyte-ratio: Results from InCHIANTI follow-up study. Immunity & Ageing 2023; 20(1), 46.
HJ Shiau and MA Reynolds. Sex differences in destructive periodontal disease: Exploring the biologic basis. Journal of Periodontology 2010; 81(11), 1505-1517.
H Zhang, JL Bain, CP Caskey, LC Sandifer and RB Johnson. Effects of gender on serum biomarkers of systemic inflammation coincident to experimentally-induced periapical lesions. Archives of Oral Biology 2011; 56(2), 168-176.
Z Jafri, A Bhardwaj, M Sawai and N Sultan. Influence of female sex hormones on periodontium: A case series. Journal of Natural Science, Biology and Medicine 2015; 6, S146-S149.
G Monasterio, F Castillo, J Astorga, A Hoare, C Terraza-Aguirre, EA Cafferata, EJ Villablanca and R Vernal. O-polysaccharide plays a major role on the virulence and immunostimulatory potential of aggregatibacter actinomycetemcomitans during periodontal infection. Frontiers in Immunology 2020; 11, 591240.
F Magata, M Horiuchi, R Echizenya, R Miura, S Chiba, M Matsui, A Miyamoto, Y Kobayashi and T Shimizu. Lipopolysaccharide in ovarian follicular fluid influences the steroid production in large follicles of dairy cows. Animal Reproduction Science 2014; 144(1-2), 6-13.
F Magata, M Horiiuchi, A Miyamoto and T Shimizu. Lipopolysaccharide (LPS) inhibits steroid production in theca cells of bovine follicles In Vitro: Distinct effect of LPS on theca cell function in pre- and post-selection follicles. The Journal of Reproduction and Development 2014; 60(4), 280-287.
KL Bidne, MJ Dickson, JW Ross, LH Baumgard and AF Keating. Disruption of female reproductive function by endotoxins. Reproduction 2020; 155(4), R169-R181.
A Nirola, P Batra and J Kaur. Ascendancy of sex hormones on periodontium during reproductive life cycle of women. Journal of the International Clinical Dental Research Organization 2018; 10(1), 3-11.
J Aisemberg, CA Vercelli, MV Bariani, SC Billi, ML Wolfson and AM Franchi. Progesterone is essential for protecting against LPS-Induced pregnancy loss. LIF as a potential mediator of the anti-inflammatory effect of progesterone. PLoS One. 2013; 8(2), e56161.
AK Sathish, J Varghese and AJ Fernandes. The impact of sex hormones on the periodontium during a woman’s lifetime: A concise-review update. Current Oral Health Reports 2022; 9(4), 146-156.
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






