An Overview of the Biomaterials Used in Hydrogel Fabrication for Chronic Wound Healing Applications
DOI:
https://doi.org/10.48048/tis.2025.9392Keywords:
Chronic wound, Hydrogel, Biomaterials, Wound dressing, BiocompatibilityAbstract
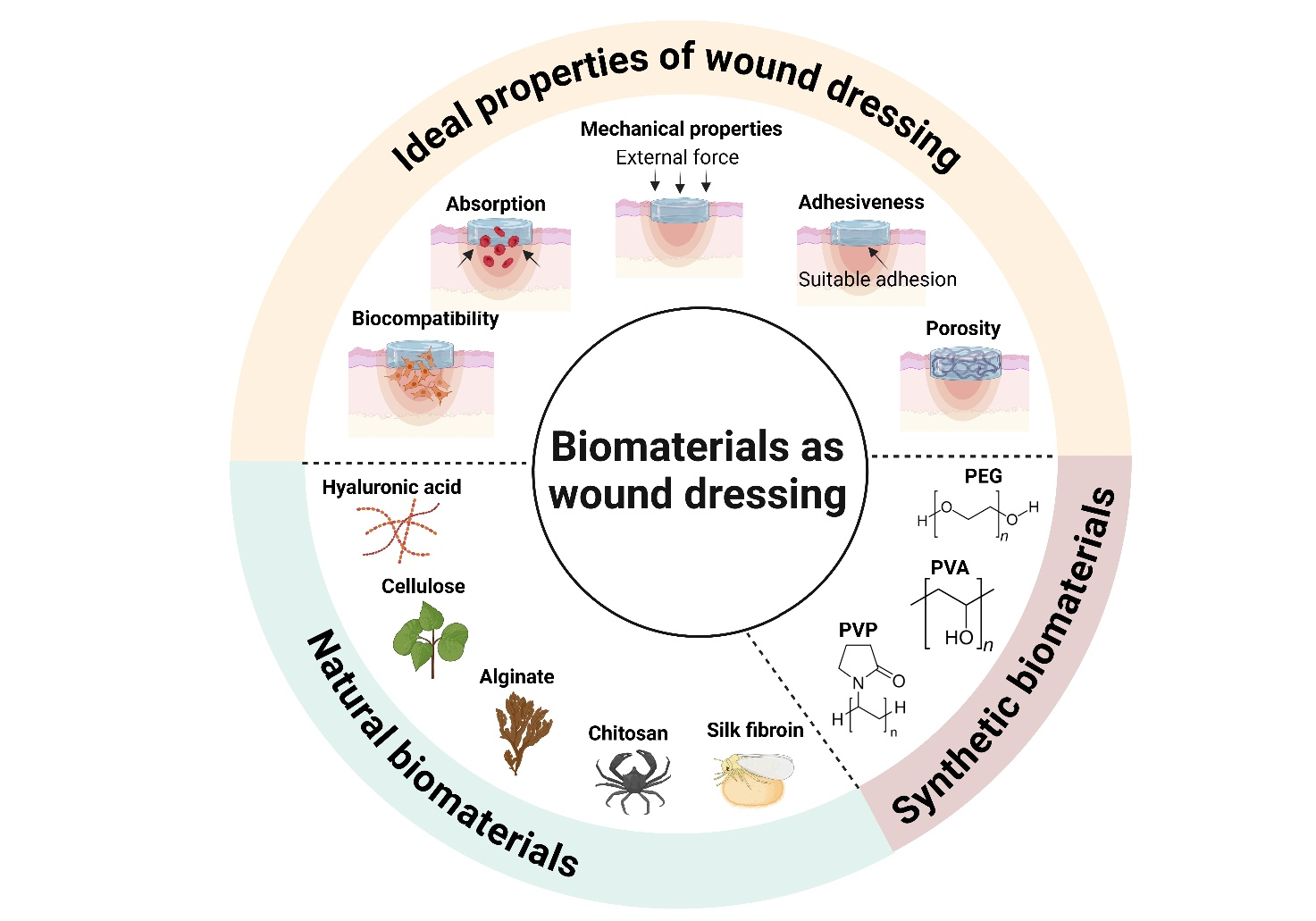
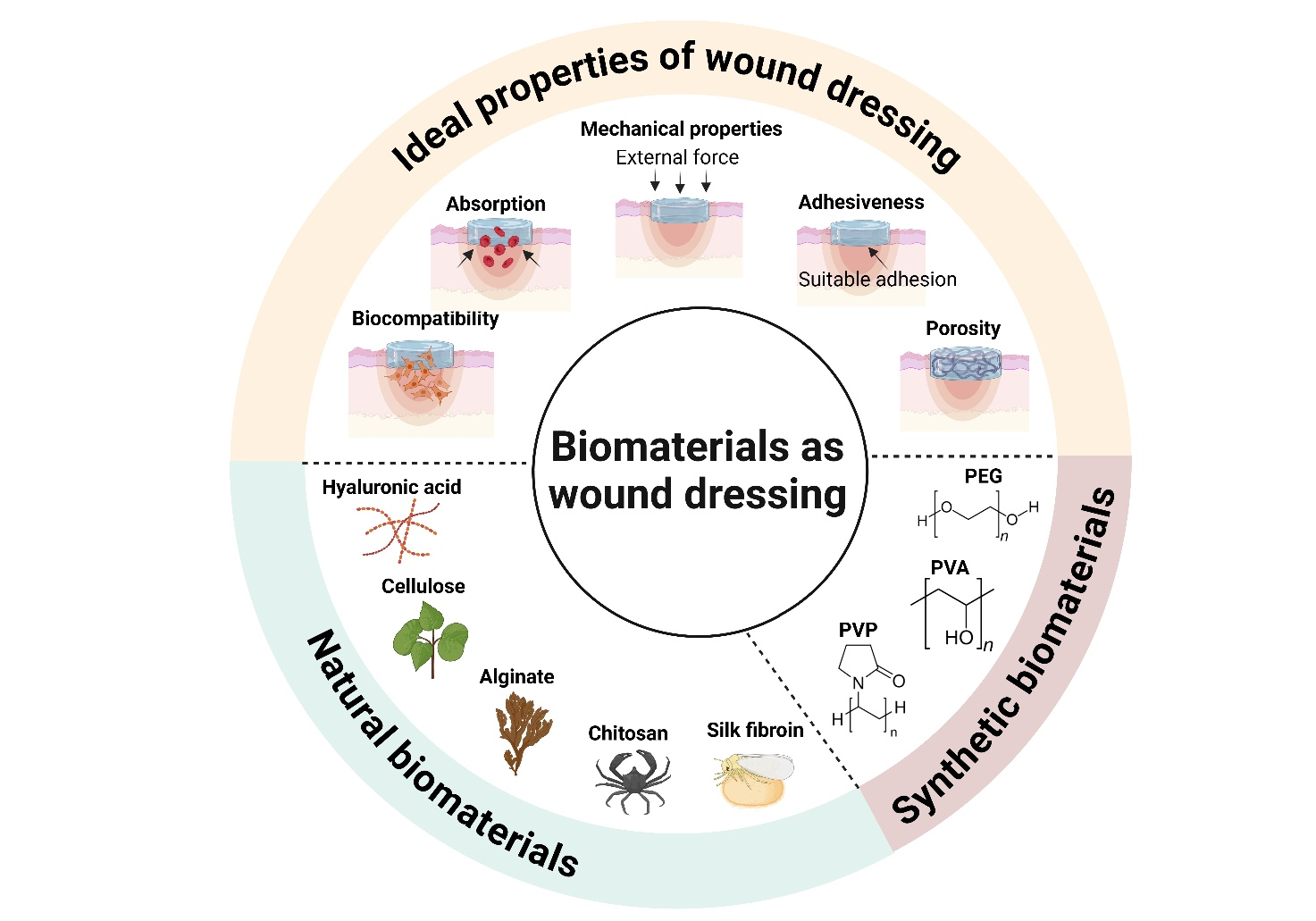
Wound healing is a delicate, complex and challenging medical process. Hydrogel is a material that possesses properties aligned with the ideal characteristics required for wound dressings. Its mechanical properties, derived from the interconnection of fibers, closely resemble those of soft tissues regarding moisture retention, secretion absorption, and oxygen permeability. Additionally, hydrogels can be tailored to perform various functions, such as crosslinking with other materials and loading drugs, bioactive compounds and growth factors. This review focuses on the fabrication of multifunctional hydrogel wound dressings using both natural and synthetic biological materials, including silk fibroin, chitosan, alginate, cellulose, hyaluronic acid, polyvinyl alcohol, polyethylene glycol and polyvinyl pyrrolidone, each exhibiting distinct properties that enhance their efficacy as wound dressings. Consequently, this review highlights significant advancements in developing more effective hydrogel wound dressings.
HIGHLIGHTS
- Chronic wounds have a significant impact on patient well-being; thus, the use of hydrogel-based wound dressings can significantly influence the rate and quality of the wound healing process.
- The design of hydrogel should also reduce inflammation, eliminate infection, promote healing process, and exploit mechanical qualities to absorb exudates.
- By incorporating bioactive molecules such as growth factors and antibacterial agents into hydrogel scaffolds, wound healing process can be enhanced.
- Before clinical trials, novel hydrogels require biocompatibility, mechanical, moisture retention, and animal model studies to ensure efficacy and safety.
- By addressing the research gap and proposing the direction of future wound dressing development, it would improve the patient outcomes for chronic wound treatment.
GRAPHICAL ABSTRACT
Downloads
References
A Sharma, R Shankar, AK Yadav, A Pratap, MA Ansari and V Srivastava. Burden of chronic nonhealing wounds: An overview of the worldwide humanistic and economic burden to the healthcare system. The International Journal of Lower Extremity Wounds 2024. https://doi.org/10.1177/153473462412463
RG Frykberg and J Banks. Challenges in the treatment of chronic wounds. Advances in Wound Care 2015; 4(9), 560-582.
MA Fonder, GS Lazarus, DA Cowan, B Aronson-Cook, AR Kohli and AJ Mamelak. Treating the chronic wound: A practical approach to the care of nonhealing wounds and wound care dressings. Journal of the American Academy of Dermatology 2008; 58(2), 185-206.
K Flynn, NN Mahmoud, S Sharifi, LJ Gould and M Mahmoudi. Chronic wound healing models. ACS Pharmacology & Translational Science 2023; 6(5), 783-801.
A Medina, PG Scott, A Ghahary and EE Tredget. Pathophysiology of chronic nonhealing wounds. Journal of Burn Care & Rehabilitation 2005; 26(4), 306-319.
PG Bowler. Wound pathophysiology, infection and therapeutic options. Annals of Medicine 2002; 34(6), 419-427.
G Han and R Ceilley. Chronic wound healing: A review of current management and treatments. Advances in Therapy 2017; 34, 599-610.
CK Sen. Human wound and its burden: Updated 2020 compendium of estimates. Advances in Wound Care 2021; 10(5), 281-292.
X Zhang, W Shu, Q Yu, W Qu, Y Wang and R Li. Functional biomaterials for treatment of chronic wound. Frontiers in Bioengineering and Biotechnology 2020; 8, 516.
J Ho, C Walsh, D Yue, A Dardik and U Cheema. Current advancements and strategies in tissue engineering for wound healing: A comprehensive review. Advances in Wound Care 2017; 6(6), 191-209.
GC Gurtner, S Werner, Y Barrandon and MT Longaker. Wound repair and regeneration. Nature 2008; 453(7193), 314-321.
V Gounden and M Singh. Hydrogels and wound healing: Current and future prospects. Gels 2024; 10(1), 43.
W Zhang, L Liu, H Cheng, J Zhu, X Li, S Ye and X Li. Hydrogel-based dressings designed to facilitate wound healing. Materials Advances 2024; 5(4), 1364-1394.
I Firlar, M Altunbek, C McCarthy, M Ramalingam and G Camci-Unal. Functional hydrogels for treatment of chronic wounds. Gels 2022; 8(2), 127.
Y Liang, J He and B Guo. Functional hydrogels as wound dressing to enhance wound healing. ACS Nano 2021; 15(8), 12687-12722.
W Wang, S Ummartyotin and R Narain. Advances and challenges on hydrogels for wound dressing. Current Opinion in Biomedical Engineering 2023; 26, 100443.
B Sheokand, M Vats, A Kumar, CM Srivastava, I Bahadur and SR Pathak. Natural polymers used in the dressing materials for wound healing: Past, present and future. Journal of Polymer Science 2023; 61(14), 1389-1414.
Y Zhong, H Xiao, F Seidi and Y Jin. Natural polymer-based antimicrobial hydrogels without synthetic antibiotics as wound dressings. Biomacromolecules 2020; 21(8), 2983-3006.
H Zhang, X Lin, X Cao, Y Wang, J Wang and Y Zhao. Developing natural polymers for skin wound healing. Bioactive Materials 2024; 33, 355-376.
GD Mogoşanu and AM Grumezescu. Natural and synthetic polymers for wounds and burns dressing. International Journal of Pharmaceutics 2014; 463(2), 127-136.
R Xu, Y Fang, Z Zhang, Y Cao, Y Yan, L Gan, J Xu and G Zhou. Recent advances in biodegradable and biocompatible synthetic polymers used in skin wound healing. Materials 2023; 16(15), 5459.
A Sadeghianmaryan, N Ahmadian, S Wheatley, H Alizadeh Sardroud, SAS Nasrollah, E Naseri and A Ahmadi. Advancements in 3D-printable polysaccharides, proteins, and synthetic polymers for wound dressing and skin scaffolding - a review. International Journal of Biological Macromolecules 2024; 266, 131207.
P Bertsch, M Diba, DJ Mooney and SCG Leeuwenburgh. Self-healing injectable hydrogels for tissue regeneration. Chemical Reviews 2023; 123(2), 834-873.
R Zhao, H Liang, E Clarke, C Jackson and M Xue. Inflammation in chronic wounds. International Journal of Molecular Sciences 2016; 17(12), 2085.
Y Zhu, R Hoshi, S Chen, J Yi, C Duan, RD Galiano, HF Zhang and GA Ameer. Sustained release of stromal cell derived factor-1 from an antioxidant thermoresponsive hydrogel enhances dermal wound healing in diabetes. Journal of Controlled Release 2016; 238, 114-122.
M Farahani and A Shafiee. Wound healing: From passive to smart dressings. Advanced Healthcare Materials 2021; 10(16), 2100477.
N Yuan, K Shao, S Huang and C Chen. Chitosan, alginate, hyaluronic acid and other novel multifunctional hydrogel dressings for wound healing: A review. International Journal of Biological Macromolecules 2023; 240, 124321.
RJ Snyder, C Fife and Z Moore. Components and quality measures of DIME (devitalized tissue, infection/inflammation, moisture balance, and edge preparation) in wound care. Advances in Skin & Wound Care 2016; 29(5), 205-215.
GD Winter. Formation of the scab and the rate of epithelization of superficial wounds in the skin of the young domestic pig. Nature 1962; 193(4812), 293-294.
Y Deng, X Yang, X Zhang, H Cao, L Mao, M Yuan and W Liao. Novel fenugreek gum-cellulose composite hydrogel with wound healing synergism: Facile preparation, characterization and wound healing activity evaluation. International Journal of Biological Macromolecules 2020; 160, 1242-1251.
W Zam, R Harfouch, R Ali, Y Atfah and A Mousa. Natural extracts and honey based impregnated gauze wound dressing preparation and in vitro antibacterial efficacy. Research Journal of Pharmacognosy and Phytochemistry 2018; 10(1), 1-7.
Z Li, A Milionis, Y Zheng, M Yee, L Codispoti, F Tan, D Poulikakos and CH Yap. Superhydrophobic hemostatic nanofiber composites for fast clotting and minimal adhesion. Nature Communications 2019; 10(1), 5562.
Z Liang, P Lai, J Zhang, Q Lai and L He. Impact of moist wound dressing on wound healing time: A meta‐analysis. International Wound Journal 2023; 20(10), 4410-4421.
H Cheng, C Li, Y Jiang, B Wang, F Wang, Z Mao, H Xu, L Wang and X Sui. Facile preparation of polysaccharide-based sponges and their potential application in wound dressing. Journal of Materials Chemistry B 2018; 6(4), 634-640.
V Vivcharenko and A Przekora. Modifications of wound dressings with bioactive agents to achieve improved pro-healing properties. Applied Sciences 2021; 11(9), 4114.
P Chaganti, I Gordon, JH Chao and S Zehtabchi. A systematic review of foam dressings for partial thickness burns. The American Journal of Emergency Medicine 2019; 37(6), 1184-1190.
Z Pan, H Ye and D Wu. Recent advances on polymeric hydrogels as wound dressings. APL Bioengineering 2021; 5, 011504.
W Wei, Q Zhang, W Zhou, Z Liu, Y Wang, EV Alakpa, H Ouyang and H Liu. Immunomodulatory application of engineered hydrogels in regenerative medicine. Applied Materials Today 2019; 14, 126-136.
S Tavakoli and AS Klar. Advanced hydrogels as wound dressings. Biomolecules 2020; 10(8), 1169.
E Rezvani Ghomi, S Khalili, S Nouri Khorasani, R Esmaeely Neisiany and S Ramakrishna. Wound dressings: Current advances and future directions. Journal of Applied Polymer Science 2019; 136(27), 47738.
AG Niculescu and AM Grumezescu. An up-to-date review of biomaterials application in wound management. Polymers 2022; 14(3), 421.
RS Duman and B Voleti. Signaling pathways underlying the pathophysiology and treatment of depression: Novel mechanisms for rapid-acting agents. Trends in Neurosciences 2012; 35(1), 47-56.
HU Zaman, JMM Islam, MA Khan and RA Khan. Physico-mechanical properties of wound dressing material and its biomedical application. Journal of the Mechanical Behavior of Biomedical Materials 2011; 4(7), 1369-1375.
HY Tan, N Wang, S Li, M Hong, X Wang and Y Feng. The reactive oxygen species in macrophage polarization: reflecting its dual role in progression and treatment of human diseases. Oxidative Medicine and Cellular Longevity 2016; 2016(1), 2795090.
C Huang, L Dong, B Zhao, Y Lu, S Huang, Z Yuan, G Luo, Y Xu and W Qian. Anti‐inflammatory hydrogel dressings and skin wound healing. Clinical and Translational Medicine 2022; 12(11), e1094.
G Wang, F Yang, W Zhou, N Xiao, M Luo and Z Tang. The initiation of oxidative stress and therapeutic strategies in wound healing. Biomedicine & Pharmacotherapy 2023; 157, 114004.
SA Alsareii, J Ahmad, A Umar, MZ Ahmad and IA Shaikh. Enhanced in vivo wound healing efficacy of a novel piperine-containing bioactive hydrogel in excision wound rat model. Molecules 2023; 28(2), 545.
P Zhou, H Zhou, J Shu, S Fu and Z Yang. Skin wound healing promoted by novel curcumin-loaded micelle hydrogel. Annals of Translational Medicine 2021; 9(14), 1152.
F Yousefian, R Hesari, T Jensen, S Obagi, A Rgeai, G Damiani, CG Bunick and A Grada. Antimicrobial wound dressings: A concise review for clinicians. Antibiotics 2023; 12(9), 1434.
Y Liang, Y Liang, H Zhang and B Guo. Antibacterial biomaterials for skin wound dressing. Asian Journal of Pharmaceutical Sciences 2022; 17(3), 353-384.
S Liu, T Jiang, R Guo, C Li, C Lu, G Yang, J Nie, F Wang, X Yang and Z Chen. Injectable and degradable PEG hydrogel with antibacterial performance for promoting wound healing. ACS Applied Bio Materials 2021; 4(3), 2769-2780.
F Zhang, C Yin, X Qi, C Guo and X Wu. Silk fibroin crosslinked glycyrrhizic acid and silver hydrogels for accelerated bacteria‐infected wound healing. Macromolecular Bioscience 2022; 22(4), 2100407.
A Gefen, P Alves, D Beeckman, B Cullen, JL Lázaro-Martínez, H Lev-Tov, B Najafi, N Santamaria, A Sharpe, T Swanson and K Woo. How should clinical wound care and management translate to effective engineering standard testing requirements from foam dressings? Mapping the existing gaps and needs. Advances in Wound Care 2024; 13(1), 34-52.
BB Mandal and SC Kundu. Cell proliferation and migration in silk fibroin 3D scaffolds. Biomaterials 2009; 30(15), 2956-2965.
N Annabi, JW Nichol, X Zhong, C Ji, S Koshy, A Khademhosseini and F Dehghani. Controlling the porosity and microarchitecture of hydrogels for tissue engineering. Tissue Engineering Part B: Reviews 2010; 16(4), 371-383.
B Ladoux and A Nicolas. Physically based principles of cell adhesion mechanosensitivity in tissues. Reports on Progress in Physics 2012; 75(11), 116601.
LA Barnes, CD Marshall, T Leavitt, MS Hu, AL Moore, JG Gonzalez, MT Longaker and GC Gurtner. Mechanical forces in cutaneous wound healing: Emerging therapies to minimize scar formation. Advances in Wound Care 2018; 7(2), 47-56.
S Prete, M Dattilo, F Patitucci, G Pezzi, OI Parisi and F Puoci. Natural and synthetic polymeric biomaterials for application in wound management. Journal of Functional Biomaterials 2023; 14(9), 455.
WE Hennink and CF Van Nostrum. Novel crosslinking methods to design hydrogels. Advanced Drug Delivery Reviews 2002; 64, 223-236.
W Sun, DA Gregory, MA Tomeh and X Zhao. Silk fibroin as a functional biomaterial for tissue engineering. International Journal of Molecular Sciences 2021; 22(3), 1499.
K Kaewprasit, A Promboon, S Kanokpanont and S Damrongsakkul. Physico‐chemical properties and in vitro response of silk fibroin from various domestic races. Journal of Biomedical Materials Research Part B: Applied Biomaterials 2014; 102(8), 1639-1647.
R Parhi. Cross-linked hydrogel for pharmaceutical applications: A review. Advanced Pharmaceutical Bulletin 2017; 7(4), 515-530.
S Kapoor and SC Kundu. Silk protein-based hydrogels: Promising advanced materials for biomedical applications. Acta Biomaterialia 2016; 31, 17-32.
M Vidya and S Rajagopal. Silk fibroin: A promising tool for wound healing and skin regeneration. International Journal of Polymer Science 2021; 2021(1), 9069924.
BD Lawrence, PM Karpecki, B Levy and DW Infanger. Silk-Derived Protein-4 (SDP-4) versus a novel sodium acetate vehicle in the treatment of patients with moderate to severe dry eye disease: A randomized, dual cohort, controlled trial. Research Square 2023, https://doi.org/10.21203/rs.3.rs-3373971/v1
HW Ju, OJ Lee, JM Lee, BM Moon, HJ Park, YR Park, MC Lee, SH Kim, JR Chao, CS Ki and CH Park. Wound healing effect of electrospun silk fibroin nanomatrix in burn-model. International Journal of Biological Macromolecule 2016; 2021(1), 9069924.
S He, D Shi, Z Han, Z Dong, Y Xie, F Zhang, W Zeng and Q Yi. Heparinized silk fibroin hydrogels loading FGF1 promote the wound healing in rats with full-thickness skin excision. Biomedical Engineering Online 2019; 18, 97.
R Yu, Y Yang, J He, M Li and B Guo. Novel supramolecular self-healing silk fibroin-based hydrogel via host-guest interaction as wound dressing to enhance wound healing. Chemical Engineering Journal 2021; 417, 128278.
B Maity, S Alam, S Samanta, RG Prakash and T Govindaraju. Antioxidant silk fibroin composite hydrogel for rapid healing of diabetic wound. Macromolecular Bioscience 2022; 22(9), 2200097.
I Aranaz, AR Alcántara, MC Civera, C Arias, B Elorza, A Heras Caballero and N Acosta. Chitosan: An overview of its properties and applications. Polymers 2021; 13(19), 3256.
XY Zhu, Y Zhao, HD Zhang, WX Wang, HH Cong and H Yin. Characterization of the specific mode of action of a chitin deacetylase and separation of the partially acetylated chitosan oligosaccharides. Marine Drugs 2019; 17(2), 74.
M Kozma, B Acharya and R Bissessur. Chitin, chitosan, and nanochitin: Extraction, synthesis, and applications. Polymers 2022; 14(19), 3989.
Y Zhao, J Li, F Leng, S Lv, W Huang, W Sun and X Jiang. Degradable porous carboxymethyl chitin hemostatic microspheres. Journal of Biomaterials Science, Polymer Edition 2020; 31(11), 1369-1384.
R Teixeira-Santos, M Lima, LC Gomes and FJ Mergulhão. Antimicrobial coatings based on chitosan to prevent implant-associated infections: A systematic review. iScience 2021; 24(12), 103480.
M Ansari, SS Kordestani, S Nazralizadeh and H Eslami. Biodegradable cell-seeded collagen based polymer scaffolds for wound healing and skin reconstruction. Journal of Macromolecular Science, Part B 2018; 57(2), 100-109.
J Lu, X Fan, J Hu, J Li, J Rong, W Wang, Y Chen, W Liu, J Chen and Y Chen. Construction and function of robust and moist bilayer chitosan-based hydrogel wound dressing. Materials & Design 2023; 226, 111604.
J Li, M Qiao, Y Ji, L Lin, X Zhang and RJ Linhardt. Chemical, enzymatic and biological synthesis of hyaluronic acids. International Journal of Biological Macromolecules 2020; 152, 199-206.
RC Gupta, R Lall, A Srivastava and A Sinha. Hyaluronic acid: Molecular mechanisms and therapeutic trajectory. Frontiers in Veterinary Science 2019; 6, 458280.
A Maleki, A Kjøniksen and B Nyström. Effect of pH on the behavior of hyaluronic acid in dilute and semidilute aqueous solutions. Macromolecular Symposia 2008; 274(1), 131-140.
H Weng, W Jia, M Li and Z Chen. New injectable chitosan-hyaluronic acid based hydrogels for hemostasis and wound healing. Carbohydrate Polymers 2022; 294, 119767.
Y Zhao, B Yi, J Hu, D Zhang, G Li, Y Lu and Q Zhou. Double cross‐linked biomimetic hyaluronic acid‐based hydrogels with thermo‐stimulated self‐contraction and tissue adhesiveness for accelerating post‐wound closure and wound healing. Advanced Functional Materials 2023; 33(26), 2300710.
JT McNamara, JLW Morgan and J Zimmer. A molecular description of cellulose biosynthesis. Annual Review of Biochemistry 2015; 84(1), 895-921.
EE Tudoroiu, CE Dinu-Pîrvu, MG Albu Kaya, L Popa, V Anuța, RM Prisada and MV Ghica. An overview of cellulose derivatives-based dressings for wound-healing management. Pharmaceuticals 2021; 14(12), 1215.
F Ahmad, B Mushtaq, FA Butt, MS Zafar, S Ahmad, A Afzal, Y Nawab, A Rasheed and Z Ulker. Synthesis and characterization of nonwoven cotton-reinforced cellulose hydrogel for wound dressings. Polymers 2021; 13(23), 4098.
A Gupta, SM Briffa, S Swingler, H Gibson, V Kannappan, G Adamus, M Kowalczuk, C Martin and I Radecka. Synthesis of silver nanoparticles using curcumin-cyclodextrins loaded into bacterial cellulose-based hydrogels for wound dressing applications. Biomacromolecules 2020; 21(5), 1802-1811.
MUA Khan, GM Stojanović, R Hassan, TJS Anand, M Al-Ejji and A Hasan. Role of graphene oxide in bacterial cellulose-gelatin hydrogels for wound dressing applications. ACS Omega 2023; 8(18), 15909-15919.
R Abka-khajouei, L Tounsi, N Shahabi, AK Patel, S Abdelkafi and P Michaud. Structures, properties and applications of alginates. Marine Drugs 2022; 20(6), 364.
S Zhang, J Dong, R Pan, Z Xu, M Li and R Zang. Structures, properties, and bioengineering applications of alginates and hyaluronic acid. Polymers 2023; 15(9), 2149.
S Nazarnezhada, G Abbaszadeh-Goudarzi, H Samadian, M Khaksari, JM Ghatar, H Khastar, N Rezaei, SR Mousavi, S Shirian and M Salehi. Alginate hydrogel containing hydrogen sulfide as the functional wound dressing material: In vitro and in vivo study. International Journal of Biological Macromolecules 2020; 164, 3323-3331.
M Saberian, E Seyedjafari, SJ Zargar, FS Mahdavi and P Sanaei‐rad. Fabrication and characterization of alginate/chitosan hydrogel combined with honey and aloe vera for wound dressing applications. Journal of Applied Polymer Science 2021; 138(47), 51398.
F Diniz, R Maia, LR De Andrade, L Andrade, M Vinicius Chaud, C Da Silva, C Corrêa, R De Albuquerque Junior, L Pereira Da Costa, S Shin, S Hassan, E Sanchez-Lopez, E Souto and P Severino. Silver nanoparticles-composing alginate/gelatine hydrogel improves wound healing in vivo. Nanomaterials 2020; 10(2), 390.
BD Ulery, LS Nair and CT Laurencin. Biomedical applications of biodegradable polymers. Journal of Polymer Science Part B: Polymer Physics 2011; 49(12), 832-864.
T Gaaz, A Sulong, M Akhtar, A Kadhum, A Mohamad and A Al-Amiery. Properties and applications of polyvinyl alcohol, halloysite nanotubes and their nanocomposites. Molecules 2015; 20(12), 22833-22847.
M Mandru, M Bercea, LM Gradinaru, C Ciobanu, M Drobota, S Vlad and R Albulescu. Polyurethane/poly(vinyl alcohol) hydrogels: Preparation, characterization and drug delivery. European Polymer Journal 2019; 118, 137-145.
H Rajati, H Alvandi, SS Rahmatabadi, L Hosseinzadeh and E Arkan. A nanofiber-hydrogel composite from green synthesized AgNPs embedded to PEBAX/PVA hydrogel and PA/Pistacia atlantica gum nanofiber for wound dressing. International Journal of Biological Macromolecules 2023; 226, 1426-1443.
BM Bakadia, L Lamboni, AA Qaed Ahmed, R Zheng, BO Ode Boni, Z Shi, S Song, T Souho, BM Mukole, F Qi and G Yang. Antibacterial silk sericin/poly (vinyl alcohol) hydrogel with antifungal property for potential infected large burn wound healing: Systemic evaluation. Smart Materials in Medicine 2023; 4, 37-58.
Y Inada, M Furukawa, H Sasaki, Y Kodera, M Hiroto, H Nishimura and A Matsushima. Biomedical and biotechnological applications of PEG- and PM-modified proteins. Trends in Biotechnology 1995; 13(3), 86-91.
J Wang, S Li, Y Han, J Guan, S Chung, C Wang and D Li. Poly(ethylene glycol)-polylactide micelles for cancer therapy. Frontiers in Pharmacology 2018; 9, 202.
T Jiang, S Liu, Z Wu, Q Li, S Ren, J Chen, X Xu, C Wang, C Lu, X Yang and Z Chen. ADSC-exo@MMP-PEG smart hydrogel promotes diabetic wound healing by optimizing cellular functions and relieving oxidative stress. Materials Today Bio 2022; 16, 100365.
C Li, T Jiang, C Zhou, A Jiang, C Lu, G Yang, J Nie, F Wang, X Yang and Z Chen. Injectable self-healing chitosan-based POSS-PEG hybrid hydrogel as wound dressing to promote diabetic wound healing. Carbohydrate Polymers 2023; 299, 120198.
M Nakada, H Ishida and Y Furushima. Structural and dynamical characterisation of intermediate water interacting polyvinyl pyrrolidone. Materialia 2020; 12, 100743.
M Kurakula and GSNK Rao. Pharmaceutical assessment of polyvinylpyrrolidone (PVP): As excipient from conventional to controlled delivery systems with a spotlight on COVID-19 inhibition. Journal of Drug Delivery Science and Technology 2020; 60, 102046.
M Contardi, D Kossyvaki, P Picone, M Summa, X Guo, JA Heredia-Guerrero, D Giacomazza, R Carzino, L Goldoni, G Scoponi, F Rancan, R Bertorelli, M Di Carlo, A Athanassiou and IS Bayer. Electrospun polyvinylpyrrolidone (PVP) hydrogels containing hydroxycinnamic acid derivatives as potential wound dressings. Chemical Engineering Journal 2021; 409, 128144.
T Ito, N Otani, K Fujii, K Mori, M Eriguchi and Y Koyama. Bioadhesive and biodissolvable hydrogels consisting of water‐swellable poly(acrylic acid)/poly(vinylpyrrolidone) complexes. Journal of Biomedical Materials Research Part B: Applied Biomaterials 2020; 108(2), 503-512.
P Lu, D Ruan, M Huang, M Tian, K Zhu, Z Gan and Z Xiao. Harnessing the potential of hydrogels for advanced therapeutic applications: Current achievements and future directions. Signal Transduction and Targeted Therapy 2024; 9(1), 166.
L Qi, C Zhang, B Wang, J Yin and S Yan. Progress in hydrogels for skin wound repair. Macromolecular Bioscience 2022; 22(7), 2100475.
L Lei, Y Bai, X Qin, J Liu, W Huang and Q Lv. Current understanding of hydrogel for drug release and tissue engineering. Gels 2022; 8(5), 301.
S Aher, D Solanki and A Jain. Nanotechnology at work: Hydrogel drug delivery architectures. Journal of Drug Delivery and Therapeutics 2024; 14(3), 179-196.
H Choi, WS Choi and JO Jeong. A review of advanced hydrogel applications for tissue engineering and drug delivery systems as biomaterials. Gels 2024; 10(11), 693.
LM Caballero Aguilar, SM Silva and SE Moulton. Growth factor delivery: Defining the next generation platforms for tissue engineering. Journal of Controlled Release 2019; 306, 40-58.
P Dadhich, P Kumar, A Roy and KN Bitar. Advances in 3D printing technology for tissue engineering. In: N Chakravorty and PC Shukla (Eds.). Regenerative medicine: Emerging techniques to translation approaches. Springer, Singapore, 2023, p. 181-206.
Á Aguilar-de-Leyva, V Linares, M Casas and I Caraballo. 3D printed drug delivery systems based on natural products. Pharmaceutics 2020; 12(7), 620.
B Zheng, Z Qiu, J Xu, X Zeng, K Liu and L Chen. 3D printing-mediated microporous starch hydrogels for wound hemostasis. Journal of Materials Chemistry B 2023; 11(35), 8411-8421.
X Zhou, X Yu, T You, B Zhao, L Dong, C Huang, X Zhou, M Xing, W Qian and G Luo. 3D printing‐based hydrogel dressings for wound healing. Advanced Science 2024; 11(47), 2404580.
A Fawzy and V Fortunata. Hydrogel dressings in wound management: Advances, applications, and future directions. International Journal of Medical Science and Clinical Research Studies 2023; 3(11), 2674-2680.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






