The Microbiota and Microbiome in COVID-19 in Adults and Children and Potential Therapeutic Interventions: A Review
DOI:
https://doi.org/10.48048/tis.2024.8702Keywords:
Microbiota, Gut microbiota, COVID-19, Dysbiosis, Immune systemAbstract
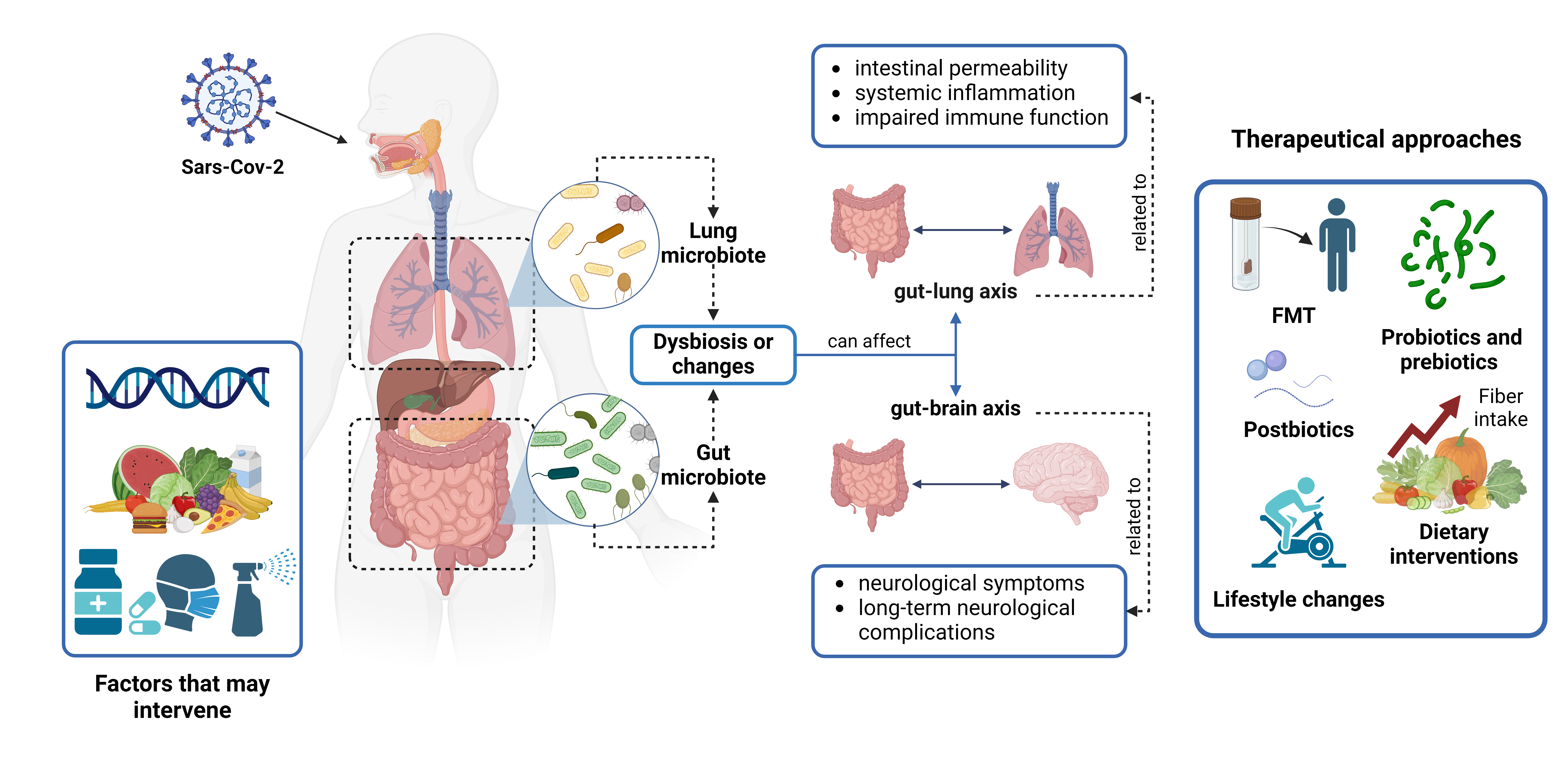
The work presented is a comprehensive review of the role of the human microbiota in the context of the COVID-19 pandemic. A diverse microbial community heavily colonizes the human body called the microbiota, with the gut microbiota being the most diverse. The composition of the microbiota varies in different parts of the body and changes with age, diet, and other environmental factors. Emerging evidence suggests that the gut microbiota plays a critical role in modulating the host immune response and may influence the severity of COVID-19. Patients with COVID-19 have significant alterations in their gut and respiratory microbiota, characterized by a depletion of beneficial commensal bacteria and an enrichment of opportunistic pathogens. These changes in microbiota composition are associated with elevated inflammatory markers, a dysregulated immune response, and more severe disease outcomes. In addition, changes in the gut microbiota can affect lung and brain function, influencing the severity of COVID-19 cases and neurological symptoms, as well as long-term neurological complications associated with the disease. Due to the importance of the microbiota in COVID-19, several therapeutic approaches targeting the microbiota have been proposed to improve outcomes in this disease, including fecal microbiota transplantation, probiotic and prebiotic supplementation, postbiotic or microbiota-derived metabolite supplementation, dietary interventions, and lifestyle strategies. Overall, the review highlights the critical role of the human microbiota in the pathogenesis and progression of COVID-19 and the potential of microbiota-targeted interventions to improve patient outcomes.
HIGHLIGHTS
- COVID-19 causes gut microbiota dysbiosis, associated with elevated inflammatory markers, a dysregulated immune response, and more severe disease outcomes.
- Gut microbiota dysbiosis due to COVID-19 affects lung and brain function, which is associated with the severity of COVID-19 cases.
- Gut microbiota is crucial in COVID-19, so several strategies have been developed to regulate it in COVID-19 cases, such as fecal microbiota transplantation, probiotics, and prebiotics, among others.
GRAPHICAL ABSTRACT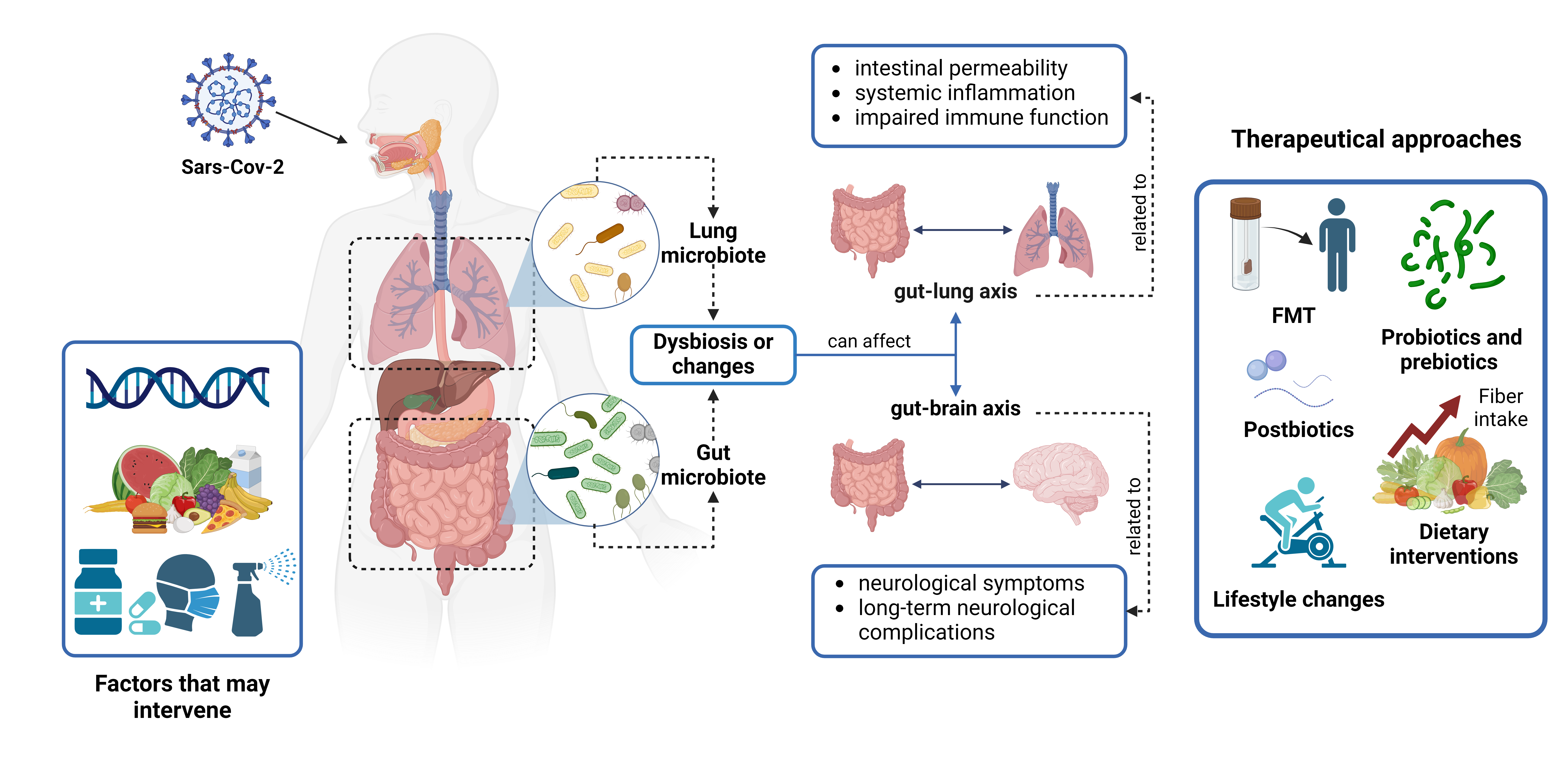
Downloads
References
T Ahrodia, S Das, S Bakshi and B Das. Structure, functions, and diversity of the healthy human microbiome. In: B Das and V Singh (Eds.). Progress in molecular biology and translational science. Academic Press, Cambridge, 2022, p. 53-82.
JL Round and NW Palm. Causal effects of the microbiota on immune-mediated diseases. Sci. Immunol. 2018; 3, eaao1603.
N Li, S Liang, Q Chen, L Zhao, B Li and G Huo. Distinct gut microbiota and metabolite profiles induced by delivery mode in healthy Chinese infants. J. Proteomics 2021; 232, 104071.
A Almeida, AL Mitchell, M Boland, SC Forster, GB Gloor, A Tarkowska, TD Lawley and RD Finn. A new genomic blueprint of the human gut microbiota. Nature 2019; 568, 499-504.
TP Wypych, LC Wickramasinghe and BJ Marsland. The influence of the microbiome on respiratory health. Nat. Immunol. 2019; 20, 1279-90.
C Pattaroni, ML Watzenboeck, S Schneidegger, S Kieser, NC Wong, E Bernasconi, J Pernot, L Mercier, S Knapp, LP Nicod, CP Marsland, M Roth-Kleiner and BJ Marsland. Early-life formation of the microbial and immunological environment of the human airways. Cell Host Microbe 2018; 24, 857-865.e4.
PW O’Toole and IB Jeffery. Microbiome-health interactions in older people. Cell Mol. Life Sci. 2018; 75, 119-28.
K Pienkowska, L Wiehlmann and B Tümmler. Airway microbial metagenomics. Microbes Infect. 2018; 20, 536-42.
E Ansaldo, TK Farley and Y Belkaid. Control of immunity by the microbiota. Annu. Rev. Immunol. 2021; 39, 449-79.
D Zheng, T Liwinski and E Elinav. Interaction between microbiota and immunity in health and disease. Cell Res. 2020; 30, 492-506.
S Cording, J Medvedovic, E Lecuyer, T Aychek and G Eberl. Control of pathogens and microbiota by innate lymphoid cells. Microbes Infect. 2018; 20, 317-22.
H Kayama, R Okumura and K Takeda. Interaction between the microbiota, epithelia, and immune cells in the intestine. Annu. Rev. Immunol. 2020; 38, 23-48.
EM Brown, DJ Kenny and RJ Xavier. Gut microbiota regulation of T cells during inflammation and autoimmunity. Annu. Rev. Immunol. 2019; 37, 599-624.
S Romagnoli, A Peris, ARD Gaudio and P Geppetti. SARS-CoV-2 and COVID-19: From the bench to the bedside. Physiol. Rev. 2020; 100, 1455-66.
WJ Wiersinga, A Rhodes, AC Cheng, SJ Peacock and HC Prescott. Pathophysiology, transmission, diagnosis, and treatment of coronavirus disease 2019 (COVID-19): A review. JAMA 2020; 324, 782-93.
AJ Rodriguez-Morales, JA Cardona-Ospina, E Gutiérrez-Ocampo, R Villamizar-Peña, Y Holguin-Rivera, JP Escalera-Antezana, LE Alvarado-Arnez, DK Bonilla-Aldana, C Franco-Paredes, AF Henao-Martinez, A Paniz-Mondolfi, GJ Lagos-Grisales, E Ramírez-Vallejo, JA Suárez, LI Zambrano, WE Villamil-Gómez, GJ Balbin-Ramon, AA Rabaan, H Harapan, …, R Sah. Clinical, laboratory and imaging features of COVID-19: A systematic review and meta-analysis. Travel Med. Infect. Dis. 2020; 34, 101623.
SA Lauer, KH Grantz, Q Bi, FK Jones, Q Zheng, HR Meredith, AS Azman, NG Reich and J Lessler. The incubation period of coronavirus disease 2019 (COVID-19) from publicly reported confirmed cases: Estimation and application. Ann. Intern. Med. 2020; 172, 577-82.
WJ Guan, ZY Ni, Y Hu, WH Liang, CQ Ou, JX He, L Liu, H Shan, CL Lei, DSC Hui, B Du, LJ Li, G Zeng, KY Yuen, RC Chen, CL Tang, T Wang, PY Chen, J Xiang, …, NS Zhong. Clinical characteristics of coronavirus disease 2019 in China. N. Engl. J. Med. 2020; 382, 1708-20.
UA Angulo-Zamudio, N León-Sicairos, J Medina-Serrano, N DeLira-Bustillos, H Villamil-Ramírez, S Canizales-Quinteros, L Macías-Kauffer, A Campos-Romero, J Alcántar-Fernández and A Canizalez-Roman. Association of FTO, ABCA1, ADRB3, and PPARG variants with obesity, type 2 diabetes, and metabolic syndrome in a Northwest Mexican adult population. J. Diabetes Complications 2021; 35, 108025.
UA Angulo-Zamudio, M Pacheco-Avila, I Medina-Ramirez, J Velazquez-Roman, J Angulo-Rocha, FA Martínez-Villa, H Flores-Villaseñor, JJ Martinez-Garcia, J Sanchez-Cuen, O Garzon-Lopez, M Guel-Gomez, HM Cuen-Diaz, MF Barajas-Olivas, A Campos-Romero, J Alcántar-Fernández, MALR Esparza and A Canizalez-Roman. Epidemiological and clinical characteristics of pregnant women and neonates with COVID-19 in Northwest Mexico. Am. J. Reprod. Immunol. 2022; 88, e13583.
R Mao, Y Qiu, JS He, JY Tan, XH Li, J Liang, J Shen, LR Zhu, Y Chen, M Iacucci, SC Ng, S Ghosh and MH Chen. Manifestations and prognosis of gastrointestinal and liver involvement in patients with COVID-19: A systematic review and meta-analysis. Lancet Gastroenterol. Hepatol. 2020; 5, 667-78.
X Jin, JS Lian, JH Hu, J Gao, L Zheng, YM Zhang, SR Hao, HY Jia, H Cai, XL Zhang, GD Yu, KJ Xu, XY Wang, JQ Gu, SY Zhang, CY Ye, CL Jin, YF Lu, X Yu, …, Y Yang. Epidemiological, clinical and virological characteristics of 74 cases of coronavirus-infected disease 2019 (COVID-19) with gastrointestinal symptoms. Gut 2020; 69, 1002-9.
C Huang, Y Wang, X Li, L Ren, J Zhao, Y Hu, L Zhang, G Fan, J Xu, X Gu, Z Cheng, T Yu, J Xia, Y Wei, W Wu, X Xie, W Yin, H Li, M Liu, Y Xiao, H Gao, L Guo, J Xie, G Wang, R Jiang, Z Gao, Q Jin, J Wang and B Cao. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020; 395, 497-506.
T Zuo, Q Liu, F Zhang, YK Yeoh, Y Wan, H Zhan, GCY Lui, Z Chen, AYL Li, CP Cheung, N Chen, W Lv, RWY Ng, EYK Tso, KSC Fung, V Chan, L Ling, G Joynt, DSC Hui, FKL Chan, PKS Chan and SC Ng. Temporal landscape of human gut RNA and DNA virome in SARS-CoV-2 infection and severity. Microbiome 2021; 9, 91.
R Xu, R Lu, T Zhang, Q Wu, W Cai, X Han, Z Wan, X Jin, Z Zhang and C Zhang. Temporal association between human upper respiratory and gut bacterial microbiomes during the course of COVID-19 in adults. Commun. Biol. 2021; 4, 240.
V Lloréns-Rico, AC Gregory, JV Weyenbergh, S Jansen, TV Buyten, J Qian, M Braz, SM Menezes, PV Mol, L Vanderbeke, C Dooms, J Gunst, G Hermans, P Meersseman, E Wauters, J Neyts, D Lambrechts, J Wauters and J Raes. Clinical practices underlie COVID-19 patient respiratory microbiome composition and its interactions with the host. Nat. Commun. 2021; 12, 6243.
I Sulaiman, M Chung, L Angel, JCJ Tsay, BG Wu, ST Yeung, K Krolikowski, Y Li, R Duerr, R Schluger, SA Thannickal, A Koide, S Rafeq, C Barnett, R Postelnicu, C Wang, S Banakis, L Pérez-Pérez, G Shen, …, E Ghedin. Microbial signatures in the lower airways of mechanically ventilated COVID-19 patients associated with poor clinical outcome. Nat. Microbiol. 2021; 6, 1245-58.
F Zhang, GCY Lui, YK Yeoh, AYL Li, H Zhan, Y Wan, ACK Chung, CP Cheung, N Chen, CKC Lai, Z Chen, EYK Tso, KSC Fung, V Chan, L Ling, G Joynt, DSC Hui, FKL Chan, PKS Chan and SC Ng. Alterations in gut microbiota of patients with COVID-19 during time of hospitalization. Gastroenterology 2020; 159, 944-955.e8.
T Zuo, H Zhan, F Zhang, Q Liu, EYK Tso, GCY Lui, N Chen, A Li, W Lu, FKL Chan, PKS Chan and SC Ng. Alterations in fecal fungal microbiome of patients with COVID-19 during time of hospitalization until discharge. Gastroenterology 2020; 159, 1302-10.
YK Yeoh, T Zuo, GCY Lui, F Zhang, Q Liu, AY Li, AC Chung, CP Cheung, EY Tso, KS Fung, V Chan, L Ling, G Joynt, DSC Hui, KM Chow, SSS Ng, TCM Li, RW Ng, TC Yip, GLH Wong, FK Chan, CK Wong, PK Chan and SC Ng. Gut microbiota composition reflects disease severity and dysfunctional immune responses in patients with COVID-19. Gut 2021; 70, 698-706.
MJ Cox, N Loman, D Bogaert and J O’Grady. Co-infections: Potentially lethal and unexplored in COVID-19. Lancet Microbe 2020; 1, e11.
N Zhu, D Zhang, W Wang, X Li, B Yang, J Song, X Zhao, B Huang, W Shi, R Lu, P Niu, F Zhan, X Ma, D Wang, W Xu, G Wu, GF Gao and W Tan. A novel coronavirus from patients with pneumonia in China, 2019. N. Engl. J. Med. 2020; 382, 727-33.
R Lu, X Zhao, J Li, P Niu, B Yang, H Wu, W Wang, H Song, B Huang, N Zhu, Y Bi, X Ma, F Zhan, L Wang, T Hu, H Zhou, Z Hu, W Zhou, L Zhao, J Chen and W Tan. Genomic characterisation and epidemiology of 2019 novel coronavirus: Implications for virus origins and receptor binding. Lancet 2020; 395, 10224.
A Wu, Y Peng, B Huang, X Ding, X Wang, P Niu, J Meng, Z Zhu, Z Zhang, J Wang, J Sheng, L Quan, Z Xia, W Tan, G Cheng and T Jiang. Genome composition and divergence of the novel coronavirus (2019-nCoV) originating in China. Cell Host Microbe 2020; 27, 325-8.
M Letko, A Marzi and V Munster. Functional assessment of cell entry and receptor usage for SARS-CoV-2 and other lineage B betacoronaviruses. Nat. Microbiol. 2020; 5, 562-9.
D Wrapp, N Wang, KS Corbett, JA Goldsmith, CL Hsieh, O Abiona, BS Graham and JS McLellan. Cryo-EM structure of the 2019-nCoV spike in the prefusion conformation. Science 2020; 367, 1260-3.
J Shang, G Ye, K Shi, Y Wan, C Luo, H Aihara, Q Geng, A Auerbach and F Li. Structural basis of receptor recognition by SARS-CoV-2. Nature 2020; 581, 221-4.
J Lan, J Ge, J Yu, S Shan, H Zhou, S Fan, Q Zhang, X Shi, Q Wang, L Zhang and X Wang. Structure of the SARS-CoV-2 spike receptor-binding domain bound to the ACE2 receptor. Nature 2020; 581, 215-20.
T Ou, H Mou, L Zhang, A Ojha, H Choe and M Farzan. Hydroxychloroquine-mediated inhibition of SARS-CoV-2 entry is attenuated by TMPRSS2. PLoS Pathog. 2021; 17, e1009212.
Q Wang, Y Zhang, L Wu, S Niu, C Song, Z Zhang, G Lu, C Qiao, Y Hu, KY Yuen, Q Wang, H Zhou, J Yan and J Qi. Structural and functional basis of SARS-CoV-2 entry by using human ACE2. Cell 2020; 181, 894-904.
M Hoffmann, H Kleine-Weber, S Schroeder, N Krüger, T Herrler, S Erichsen, TS Schiergens, G Herrler, NH Wu, A Nitsche, MA Müller, C Drosten and S Pöhlmann. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell 2020; 181, 271-80.
J Lv, Z Wang, Y Qu, H Zhu, Q Zhu, W Tong, L Bao, Q Lv, J Cong, D Li, W Deng, P Yu, J Song, WM Tong, J Liu, Y Liu, C Qin and B Huang. Distinct uptake, amplification, and release of SARS-CoV-2 by M1 and M2 alveolar macrophages. Cell Discov. 2021; 7, 24.
B Wang, L Zhang, Y Wang, T Dai, Z Qin, F Zhou and L Zhang. Alterations in microbiota of patients with COVID-19: Potential mechanisms and therapeutic interventions. Signal Transduction Target Ther. 2022; 7, 143.
M Suárez-Fariñas, M Tokuyama, G Wei, R Huang, A Livanos, D Jha, A Levescot, H Irizar, R Kosoy, S Cording, W Wang, B Losic, RC Ungaro, A Di’Narzo, G Martinez-Delgado, M Suprun, MJ Corley, A Stojmirovic, SM Houten, …, S Mehandru. Intestinal inflammation modulates the expression of ACE2 and TMPRSS2 and potentially overlaps with the pathogenesis of SARS-CoV-2-related disease. Gastroenterology 2021; 160, 287-301.
X Zou, K Chen, J Zou, P Han, J Hao and Z Han. Single-cell RNA-seq data analysis on the receptor ACE2 expression reveals the potential risk of different human organs vulnerable to 2019-nCoV infection. Front. Med. 2020; 14, 185-92.
Y Zhao, Z Zhao, Y Wang, Y Zhou, Y Ma and W Zuo. Single-cell RNA expression profiling of ACE2, the receptor of SARS-CoV-2. Am. J. Respir. Crit. Care Med. 2020; 202, 756-9.
MFG Castro, BT McCune, Q Zeng, PW Rothlauf, NM Sonnek, Z Liu, KF Brulois, X Wang, HB Greenberg, MS Diamond, MA Ciorba, SPJ Whelan and S Ding. TMPRSS2 and TMPRSS4 promote SARS-CoV-2 infection of human small intestinal enterocytes. Sci. Immunol. 2020; 5, eabc3582.
W Sungnak, N Huang, C Bécavin, M Berg, R Queen, M Litvinukova, C Talavera-López, H Maatz, D Reichart, F Sampaziotis, KB Worlock, M Yoshida and JL Barnes. SARS-CoV-2 entry factors are highly expressed in nasal epithelial cells together with innate immune genes. Nat. Med. 2020; 26, 681-7.
S Lukassen, RL Chua, T Trefzer, NC Kahn, MA Schneider, T Mule, H Winter, M Meister, C Veith, AW Boots, BP Hennig, M Kreuter, C Conrad and R Eils. SARS-CoV-2 receptor ACE2 and TMPRSS2 are primarily expressed in bronchial transient secretory cells. EMBO J. 2020; 39, e105114.
CJ Burrell, CR Howard and FA Murphy. Fenner and white’s medical virology. Academic Press, Cambridge, 2017, p. 437-46.
D Wu, T Wu, Q Liu and Z Yang. The SARS-CoV-2 outbreak: What we know. Int. J. Infect. Dis. 2020; 94, 44-8.
Centers for Disease Control and Prevention. SARS-CoV-2 variant classifications and definitions. 2022, Available at: https://www.cdc.gov/coronavirus/2019-ncov/variants/variant-classifications. html, accessed January 2024.
A Rambaut, EC Holmes, Á O’Toole, V Hill, JT McCrone, C Ruis, LD Plessis and OG Pybus. A dynamic nomenclature proposal for SARS-CoV-2 lineages to assist genomic epidemiology. Nat. Microbiol. 2020; 5, 1403-7.
S Rajput, D Paliwal, M Naithani, A Kothari, K Meena and S Rana. COVID-19 and gut microbiota: A potential connection. Indian J. Clin. Biochem. 2021; 36, 266-77.
M Jabczyk, J Nowak, B Hudzi and B Zubelewicz-Szkodzińska. Diet, probiotics and their impact on the gut microbiota during the COVID-19 pandemic. Nutrients 2021; 13, 3172.
S Tarashi, MS Zamani, MD Omrani, A Fateh, A Moshiri, A Saedisomeolia, SD Siadat and S Kubow. Commensal and pathogenic bacterial-derived extracellular vesicles in host-bacterial and interbacterial dialogues: Two sides of the same coin. J. Immunol. Res. 2022; 2022, 8092170.
J Xu, B Lawley, G Wong, A Otal, L Chen, TJ Ying, X Lin, WW Pang, F Yap, YS Chong, PD Gluckman, YS Lee, MF Chong, GW Tannock and N Karnani. Ethnic diversity in infant gut microbiota is apparent before the introduction of complementary diets. Gut Microbes 2020; 11, 1362-73.
S Wandro, S Osborne, C Enriquez, C Bixby, A Arrieta and K Whiteson. The microbiome and metabolome of preterm infant stool are personalized and not driven by health outcomes, including necrotizing enterocolitis and late-onset sepsis. mSphere 2018; 3, e00104-18.
S Yamamoto, M Saito, A Tamura, D Prawisuda, T Mizutani and H Yotsuyanagi. The human microbiome and COVID-19: A systematic review. PLoS One 2021; 16, e0253293.
G Ianiro, BH Mullish, CR Kelly, H Sokol, Z Kassam, SC Ng, M Fischer, JR Allegretti, L Masucci, F Zhang, J Keller, M Sanguinetti, SP Costello, H Tilg and A Gasbarrini. Screening of faecal microbiota transplant donors during the COVID-19 outbreak: Suggestions for urgent updates from an international expert panel. Lancet Gastroenterol. Hepatol. 2020; 5, 430-2.
HJ Lee and M Kim. Skin barrier function and the microbiome. Int. J. Mol. Sci. 2022; 23, 13071.
M Relvas, A Regueira-Iglesias, C Balsa-Castro, F Salazar, JJ Pacheco, C Cabral, C Henriques and I Tomás. Relationship between dental and periodontal health status and the salivary microbiome: Bacterial diversity, co-occurrence networks and predictive models. Sci. Rep. 2021; 11, 929.
WADS Piters, EA Sanders and D Bogaert. The role of the local microbial ecosystem in respiratory health and disease. Philos. Trans. R. Soc. London B Biol. Sci. 2015; 370, 20140294.
BA Tortelli, WG Lewis, JE Allsworth, N Member-Meneh, LR Foster, HE Reno, JF Peipert, JC Fay and AL Lewis. Associations between the vaginal microbiome and Candida colonization in women of reproductive age. Am. J. Obstet. Gynecol. 2020; 222, 471.e1-471.e9.
MM Lamers, J Beumer, JVD Vaart, K Knoops, J Puschhof, TI Breugem, RBG Ravelli, JPV Schayck, AZ Mykytyn, HQ Duimel, EV Donselaar, S Riesebosch, HJH Kuijpers, D Schipper, WJVD Wetering, MD Graaf, M Koopmans, E Cuppen, PJ Peters, …, H Clevers. SARS-CoV-2 productively infects human gut enterocytes. Science 2020; 369, 50-4.
S Khanmohammadi and N Rezaei. Role of Toll-like receptors in the pathogenesis of COVID-19. J. Med. Virol. 2021; 93, 2735-9.
C Donovan, G Liu, S Shen, JE Marshall, RY Kim, CA Alemao, KF Budden, JP Choi, M Kohonen-Corish, EM El-Omar, IA Yang and PM Hansbro. The role of the microbiome and the NLRP3 inflammasome in the gut and lung. J. Leukocyte Biol. 2020; 108, 925-35.
L Yang, C Liu, W Zhao, C He, J Ding, R Dai, K Xu, L Xiao, L Luo, S Liu, W Li and H Meng. Impaired autophagy in intestinal epithelial cells alters gut microbiota and host immune responses. Appl. Environ. Microbiol. 2018; 84, e00880-18.
L Aldars-García, AC Marin, M Chaparro and JP Gisbert. The interplay between immune system and microbiota in inflammatory bowel disease: A narrative review. Int. J. Mol. Sci. 2021; 22, 3076.
YP Hung, CC Lee, JC Lee, PJ Tsai and WC Ko. Gut dysbiosis during COVID-19 and potential effect of probiotics. Microorganisms 2021; 9, 1605.
M Gong, G Wang, K Dua, J Xu, X Xu and G Liu. COVID-19 and gut injury. Nutrients 2022; 14, 4409.
SA Badi, S Khatami and SD Siadat. Tripartite communication in COVID-19 infection: SARS-CoV-2 pathogenesis, gut microbiota and ACE2. Future Virol. 2022; 17, 773-6.
Y Fan and O Pedersen. Gut microbiota in human metabolic health and disease. Nat. Rev. Microbiol. 2021; 19, 55-71.
V Marrella, F Nicchiotti and B Cassani. Microbiota and immunity during respiratory infections: Lung and gut affair. Int. J. Mol. Sci. 2024; 25, 4051.
L Zheng, C Liu, H Wang, J Zhang, L Mao, X Dong, S Hu, N Li, D Pi, J Qiu, F Xu, C Chen and Z Zou. Intact lung tissue and bronchoalveolar lavage fluid are both suitable for the evaluation of murine lung microbiome in acute lung injury. Microbiome 2024; 12, 56.
JM Cavaillon, BG Chousterman and T Skirecki. Compartmentalization of the inflammatory response during bacterial sepsis and severe COVID-19. J. Intensive Med. 2024; 4, 326-40.
SJ Piersma. Tissue-specific features of innate lymphoid cells in antiviral defense. Cell. Mol. Immunol. 2024. https://doi.org/10.1038/s41423-024-01161-x
D Dhar and A Mohanty. Gut microbiota and Covid-19- possible link and implications. Virus Res. 2020; 285, 198018.
SH Wong, RN Lui and JJ Sung. Covid-19 and the digestive system. J. Gastroenterol. Hepatol. 2020; 35, 744-8.
C Wang, Q Li and J Ren. Microbiota-immune interaction in the pathogenesis of gut-derived infection. Front. Immunol. 2019; 10, 1873.
S Ostadmohammadi, SA Nojoumi, A Fateh, SD Siadat and F Sotoodehnejadnematalahi. Interaction between Clostridium species and microbiota to progress immune regulation. Acta Microbiologica Immunologica Hungarica 2022; 69, 89-103.
SF Oh, T Praveena, H Song, JS Yoo, DJ Jung, D Erturk-Hasdemir, YS Hwang, CWC Lee, JL Nours, H Kim, J Lee, RS Blumberg, J Rossjohn, SB Park and DL Kasper. Host immunomodulatory lipids created by symbionts from dietary amino acids. Nature 2021; 600, 302-7.
Y Shen, F Yu, D Zhang, Q Zou, M Xie, X Chen, L Yuan, B Lou, G Xie, R Wang, X Yang, W Chen, Q Wang, B Feng, Y Teng, Y Dong, L Huang, J Bao, D Han, C Liu, W Wu, X Liu, L Fan, MP Timko, S Zheng and Y Chen. Dynamic alterations in the respiratory tract microbiota of patients with COVID-19 and its association with microbiota in the gut. Adv. Sci. 2022; 9, e2200956.
S Lamichhane, P Sen, AM Dickens, M Orešič and HC Bertram. Gut metabolome meets microbiome: A methodological perspective to understand the relationship between host and microbe. Methods 2018; 149, 3-12.
RG Nichols, JM Peters and AD Patterson. Interplay between the host, the human microbiome, and drug metabolism. Hum. Genomics 2019; 13, 27.
D Ellinghaus, F Degenhardt, L Bujanda, M Buti, A Albillos, P Invernizzi, J Fernández, D Prati, G Baselli, R Asselta, MM Grimsrud, C Milani, F Aziz, J Kässens, S May, M Wendorff, L Wienbrandt, F Uellendahl-Werth, T Zheng, …, TH Karlsen. Genomewide association study of severe Covid-19 with respiratory failure. N. Engl. J. Med. 2020; 383, 1522-34.
T Zuo, Q Liu, F Zhang, GCY Lui, EY Tso, YK Yeoh, Z Chen, SS Boon, FK Chan, PK Chan and SC Ng. Gut 2021; 70, 276-84.
H Tangestani, HK Boroujeni, K Djafarian, H Emamat and S Shab-Bidar. Vitamin D and the gut microbiota: A narrative literature review. Clin. Nutr. Res. 2021; 10, 181-91.
G Merra, A Capacci, G Cenname, E Esposito, M Dri, LD Renzo and M Marchetti. The “microbiome”: A protagonist in COVID-19 era. Microorganisms 2022; 10, 296.
F Li, H Lu, X Li, X Wang, Q Zhang and L Mi. The impact of COVID-19 on intestinal flora: A protocol for systematic review and meta analysis. Medicine 2020; 99, e22273.
J Chen and L Vitetta. The role of the gut-lung axis in COVID-19 infections and its modulation to improve clinical outcomes. Front. Biosci. 2022; 14, 23.
SM Yousof, I Tanvir, E Kolieb and R Atta. Work stress, dysbiosis, and immune dysregulation: The interconnected triad in COVID-19 infection in the medical team staff - A mini-review. J. Microsc. Ultrastruct. 2022; 10, 147-53.
R Jitvaropas, O Mayuramart, V Sawaswong, P Kaewsapsak and S Payungporn. Classification of salivary bacteriome in asymptomatic COVID-19 cases based on long-read nanopore sequencing. Exp. Biol. Med. 2022; 247, 1937-46.
N Katz-Agranov and G Zandman-Goddard. Autoimmunity and COVID-19 - The microbiotal connection. Autoimmun. Rev. 2021; 20, 102865.
JW Blackett, Y Sun, L Purpura, KG Margolis, MSV Elkind, S O’Byrne, M Wainberg, JA Abrams, HH Wang, L Changa and DE Freedberg. Decreased gut microbiome tryptophan metabolism and serotonergic signaling in patients with persistent mental health and gastrointestinal symptoms after COVID-19. Clin. Transl. Gastroenterol. 2022; 13, e00524.
Q Liu, JWY Mak, Q Su, YK Yeoh, GCY Lu, SSS Ng, F Zhang, AYL Li, W Lu, DSC Hui, PK Chan, FKL Chan and SC Ng. Gut microbiota dynamics in a prospective cohort of patients with post-acute COVID-19 syndrome. Gut 2022; 71, 544-52.
R Enaud, R Prevel, E Ciarlo, F Beaufils, G Wieërs, B Guery and L Delhaes. The gut-lung axis in health and respiratory diseases: A place for inter-organ and inter-kingdom crosstalks. Front. Cell. Infect. Microbiol. 2020. https://doi.org/10.3389/fcimb.2020.00009
AT Dang and BJ Marsland. Microbes, metabolites, and the gut-lung axis. Mucosal Immunol. 2019; 12, 843-50.
Y Tian, KY Sun, TQ Meng, Z Ye, SM Guo, ZM Li, CL Xiong, Y Yin, HG L and LQ Zhou. Gut microbiota may not be fully restored in recovered COVID-19 patients after 3-month recovery. Front. Nutr. 2021; 8, 638825.
L Tang, S Gu, Y Gong, B Li, H Lu, Q Li, R Zhang, X Gao, Z Wu, J Zhang, Y Zhang and L Li. Clinical significance of the correlation between changes in the major intestinal bacteria species and COVID-19 severity. Engineering 2020; 6, 1178-84.
J Cao, C Wang, Y Zhang, G Lei, K Xu, N Zhao, J Lu, F Meng, L Yu, J Yan, C Bai, S Zhang, N Zhang, Y Gong, Y Bi, Y Shi, Z Chen, L Dai, J Wang and P Yang. Integrated gut virome and bacteriome dynamics in COVID-19 patients. Gut Microbes 2021; 13, 1887722.
Y Han, Z Jia, J Shi, W Wang and K He. The active lung microbiota landscape of COVID-19 patients through the metatranscriptome data analysis. Bioimpacts 2022; 12, 139-46.
N Nagata, T Takeuchi, H Masuoka, R Aoki, M Ishikane, N Iwamoto, M Sugiyama, W Suda, Y Nakanishi, J Terada-Hirashima, M Kimura, T Nishijima, H Inooka, T Miyoshi-Akiyama, Y Kojima, C Shimokawa, H Hisaeda, F Zhang, YK Yeoh, …, H Ohno. Human gut microbiota and its metabolites impact immune responses in COVID-19 and its complications. Gastroenterology 2023; 164, 272-88.
S Stricker, T Hain, CM Chao and S Rudloff. Respiratory and intestinal microbiota in pediatric lung diseases-current evidence of the gut-lung axis. Int. J. Mol. Sci. 2022; 23, 6791.
B Aktas and B Aslim. Gut-lung axis and dysbiosis in COVID-19. Turk. J. Biol. 2020; 44, 265-72.
A Hernández-Terán, AE Vega-Sánchez, F Mejía-Nepomuceno, R Serna-Muñoz, S Rodríguez-Llamazares, I Salido-Guadarrama, JA Romero-Espinoza, C Guadarrama-Pérez, JL Sandoval-Gutierrez, F Campos, EN Mondragón-Rivero, A Ramírez-Venegas, M Castillejos-López, NA Téllez-Navarrete, R Pérez-Padilla and JA Vázquez-Pérez. Microbiota composition in the lower respiratory tract is associated with severity in patients with acute respiratory distress by influenza. Virol. J. 2023; 20, 19.
E Dima, A Kyriakoudi, M Kaponi, I Vasileiadis, P Stamou, A Koutsoukou, NG Koulouris and N Rovina. The lung microbiome dynamics between stability and exacerbation in chronic obstructive pulmonary disease (COPD): Current perspectives. Respir. Med. 2019; 157, 1-6.
A Kuwahara, K Matsuda, Y Kuwahara, S Asano, T Inui and Y Marunaka. Microbiota-gut-brain axis: enteroendocrine cells and the enteric nervous system form an interface between the microbiota and the central nervous system. Biomed. Res. 2020; 41, 199-216.
N Kim, M Yun, YJ Oh and HJ Choi. Mind-altering with the gut: Modulation of the gut-brain axis with probiotics. J. Microbiol. 2018; 56, 172-82.
CR Martin, V Osadchiy, A Kalani and EA Mayer. The brain-gut-microbiome axis. Cell. Mol. Gastroenterol. Hepatol. 2018; 6, 133-48.
H Forssberg. Microbiome programming of brain development: Implications for neurodevelopmental disorders. Dev. Med. Child Neurol. 2019; 61, 744-9.
L Sempach, JPK Doll, V Limbach, F Marzetta, AC Schaub, E Schneider, C Kettelhack, L Mählmann, N Schweinfurth-Keck, M Ibberson, UE Lang and A Schmidt. Examining immune-inflammatory mechanisms of probiotic supplementation in depression: Secondary findings from a randomized clinical trial. Transl. Psychiatry 2024; 14, 305.
JB Zawilska and K Kuczyńska. Psychiatric and neurological complications of long COVID. J. Psychiat. Res. 2022; 156, 349-60.
S Lopez-Leon, T Wegman-Ostrosky, C Perelman, R Sepulveda, PA Rebolledo, A Cuapio and S Villapol. More than 50 long-term effects of COVID-19: A systematic review and meta-analysis. Sci. Rep. 2021; 11, 16144.
COVID-19 Mental Disorders Collaborators. Global prevalence and burden of depressive and anxiety disorders in 204 countries and territories in 2020 due to the COVID-19 pandemic. Lancet 2021; 398, 1700-12.
OL Aiyegbusi, SE Hughes, G Turner, SC Rivera, C McMullan, JS Chandan, S Haroon, G Price, EH Davies, K Nirantharakumar, E Sapey and MJ Calvert. Symptoms, complications and management of long COVID: A review. J. R. Soc. Med. 2021; 114, 428-42.
JR Lechien, CM Chiesa-Estomba, DRD Siati, M Horoi, SDL Bon, A Rodriguez, D Dequanter, S Blecic, FE Afia, L Distinguin, Y Chekkoury-Idrissi, S Hans, IL Delgado, C Calvo-Henriquez, P Lavigne, C Falanga, MR Barillari, G Cammaroto, M Khalife, …, S Saussez. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): A multicenter European study. Eur. Arch. Otorhinolaryngol. 2020; 277, 2251-61.
E Xu, Y Xie and Z Al-Aly. Long-term neurologic outcomes of COVID-19. Nat. Med. 2022; 28, 2406-15.
M Taquet, JR Geddes, M Husain, S Luciano and PJ Harrison. 6-month neurological and psychiatric outcomes in 236 379 survivors of COVID-19: A retrospective cohort study using electronic health records. Lancet Psychiatry 2021; 8, 416-27.
K Socała, U Doboszewska, A Szopa, A Serefko, M Włodarczyk, A Zielińska, E Poleszak, J Fichna and P Wlaź. The role of microbiota-gut-brain axis in neuropsychiatric and neurological disorders. Pharmacol. Res. 2021; 172, 105840.
B Golofast and K Vales. The connection between microbiome and schizophrenia. Neurosci. Biobehav. Rev. 2020; 108, 712-31.
JH Kim, Y Lee, YS Kwon and JH Sohn. Clinical implications of the association between respiratory and gastrointestinal disorders in migraine and non-migraine headache patients. J. Clin. Med. 2023; 12, 3434.
G Kokic, HS Hillen, D Tegunov, C Dienemann, F Seitz, J Schmitzova, L Farnung, A Siewert, C Höbartner and P Cramer. Mechanism of SARS-CoV-2 polymerase stalling by remdesivir. Nat. Commun. 2021; 12, 279.
F Kabinger, C Stiller, J Schmitzová, C Dienemann, G Kokic, HS Hillen, C Höbartner and P Cramer. Mechanism of molnupiravir-induced SARS-CoV-2 mutagenesis. Nat. Struct. Mol. Biol. 2021; 28, 740-6.
W Fischer, JJ Eron, W Holman, MS Cohen, L Fang, LJ Szewczyk, TP Sheahan, R Baric, KR Mollan, CR Wolfe, ER Duke, MM Azizad, K Borroto-Esoda, DA Wohl, AJ Loftis, P Alabanza, F Lipansky and WP Painter. Molnupiravir, an oral antiviral treatment for COVID-19. medRxiv 2021; 14, eabl7430.
DR Owen, CMN Allerton, AS Anderson, L Aschenbrenner, M Avery, S Berritt, B Boras, RD Cardin, A Carlo, KJ Coffman, A Dantonio, L Di, H Eng, RA Ferre, KS Gajiwala, SA Gibson, SE Greasley, BL Hurst, EP Kadar, …, Y Zhu. An oral SARS-CoV-2 M(pro) inhibitor clinical candidate for the treatment of COVID-19. Science 2021; 374, 1586-93.
J Stebbing, V Krishnan, SD Bono, S Ottaviani, G Casalini, PJ Richardson, V Monteil, VM Lauschke, A Mirazimi, S Youhanna, YJ Tan, F Baldanti, A Sarasini, JAR Terres, BJ Nickoloff, RE Higgs, G Rocha, NL Byers, DE Schlichting, …, M Corbellino. Mechanism of baricitinib supports artificial intelligence-predicted testing in COVID-19 patients. EMBO Mol. Med. 2020; 12, e12697.
AC Kalil, TF Patterson, AK Mehta, KM Tomashek, CR Wolfe, V Ghazaryan, VC Marconi, GM Ruiz-Palacios, L Hsieh, S Kline, V Tapson, NM Iovine, MK Jain, DA Sweeney, HME Sahly, AR Branche, JR Pineda, DC Lye, U Sandkovsky, …, JH Beigel. Baricitinib plus remdesivir for hospitalized adults with Covid-19. N. Engl. J. Med. 2021; 384, 795-807.
P Zimmermann, KP Perrett, N Ritz, KL Flanagan, R Robins-Browne, FRMVD Klis and N Curtis. Biological sex influences antibody responses to routine vaccinations in the first year of life. Acta Paediatrica 2020; 109, 147-57.
T Hagan, T Hagan, M Cortese, N Rouphael, C Boudreau, C Linde, MS Maddur, J Das, H Wang, J Guthmiller, NY Zheng, M Huang, AA Uphadhyay, L Gardinassi, C Petitdemange, MP McCullough, SJ Johnson, K Gill, B Cervasi and J Zo. Antibiotics-driven gut microbiome perturbation alters immunity to vaccines in humans. Cell 2019; 178, 1313-28.
VC Harris, BW Haak, SA Handley, B Jiang, DE Velasquez, BLJ Hykes, L Droit, GAM Berbers, EM Kemper, EMMV Leeuwen, MBV Hensbroek and WJ Wiersinga. Effect of antibiotic-mediated microbiome modulation on rotavirus vaccine immunogenicity: A human, randomized-control proof-of-concept trial. Cell Host Microbe 2018; 24, 197-207.
PV Damme, ID Coster, AS Bandyopadhyay, H Revets, K Withanage, PD Smedt, L Suykens, MS Oberste, WC Weldon, SA Costa-Clemens, R Clemens, J Modlin, AJ Weiner, AJ Macadam, R Andino, OM Kew, JL Konopka-Anstadt, CC Burns, J Konz, …, C Gast. The safety and immunogenicity of two novel live attenuated monovalent (serotype 2) oral poliovirus vaccines in healthy adults: A double-blind, single-centre phase 1 study. Lancet 2019; 394, 148-58.
DV Patangia, CA Ryan, E Dempsey, RP Ross and C Stanton. Impact of antibiotics on the human microbiome and consequences for host health. Microbiologyopen 2022; 11, e1260.
Y Lu, X Yuan, M Wang, Z He, H Li, J Wang and Q Li. Gut microbiota influence immunotherapy responses: Mechanisms and therapeutic strategies. J. Hematol. Oncol. 2022; 15, 47.
S Feng, C Zhang, S Chen, R He, G Chao and S Zhang. TLR5 signaling in the regulation of intestinal mucosal immunity. J. Inflammation Res. 2023; 16, 2491-501.
MT Sorbara and EG Pamer. Microbiome-based therapeutics. Nat. Rev. Microbiol. 2022; 16, 2491-501.
JWY Mak, FKL Chan and SC Ng. Probiotics and COVID-19: One size does not fit all. Lancet Gastroenterol. Hepatol. 2020; 5, 644-5.
T Shinde, PM Hansbro, SS Sohal, P Dingle, R Eri and R Stanley. Microbiota modulating nutritional approaches to countering the effects of viral respiratory infections including SARS-CoV-2 through promoting metabolic and immune fitness with probiotics and plant bioactives. Microorganisms 2020; 8, 921.
F Anwar, HN Altayb, FA Al-Abbasi, AL Al-Malki, MA Kamal and V Kumar. Antiviral effects of probiotic metabolites on COVID-19. J. Biomol. Struct. Dyn. 2021; 39, 4175-84.
SK Tiwari, LMT Dicks, IV Popov, A Karaseva, AM Ermakov, A Suvorov, JR Tagg, R Weeks and ML Chikindas. Probiotics at war against viruses: What is missing from the picture? Front. Microbiol. 2020; 11, 1877.
F Infusino, F Infusino, M Marazzato, M Mancone, F Fedele, CM Mastroianni, P Severino, G Ceccarelli, L Santinelli, E Cavarretta, AGM Marullo, F Miraldi, R Carnevale, C Nocella, G Biondi-Zoccai, C Pagnini, S Schiavon, F Pugliese, G Frati and G D’Ettorre. Diet supplementation, probiotics, and nutraceuticals in SARS-CoV-2 infection: A scoping review. Nutrients 2020; 12, 17186.
L Conte and DM Toraldo. Targeting the gut-lung microbiota axis by means of a high-fibre diet and probiotics may have anti-inflammatory effects in COVID-19 infection. Ther. Adv. Respir. Dis. 2020; 14, 1753466620937170.
D Baud, VD Agri, GR Gibson, G Reid and E Giannoni. Using probiotics to flatten the curve of coronavirus disease COVID-2019 pandemic. Front. Public Health 2020; 8, 186.
PD Groot, T Nikolic, S Pellegrini, V Sordi, S Imangaliyev, E Rampanelli, N Hanssen, I Attaye, G Bakker, G Duinkerken, A Joosten, A Prodan, E Levin, H Levels, BPV Loon, AV Bon, C Brouwer, SV Dam, S Simsek, …, M Nieuwdorp. Faecal microbiota transplantation halts progression of human new-onset type 1 diabetes in a randomised controlled trial. Gut 2021; 70, 92-105.
S Paramsothy, S Nielsen, MA Kamm, NP Deshpande, JJ Faith, JC Clemente, R Paramsothy, AJ Walsh, JVD Bogaerde, D Samuel, RWL Leong, S Connor, W Ng, E Lin, TJ Borody, MR Wilkins, JF Colombel, HM Mitchell and NO Kaakoush. Specific bacteria and metabolites associated with response to fecal microbiota transplantation in patients with ulcerative colitis. Gastroenterology 2019; 156, 1440-1454.e2.
SP Costello, PA Hughes, O Waters, RV Bryant, AD Vincent, P Blatchford, R Katsikeros, J Makanyanga, MA Campaniello, C Mavrangelos, CP Rosewarne, C Bickley, C Peters, MN Schoeman, MA Conlon, IC Roberts-Thomson and JM Andrews. Effect of fecal microbiota transplantation on 8-week remission in patients with ulcerative colitis: A randomized clinical trial. JAMA 2019; 321, 156-64.
OV Goloshchapov, AB Chukhlovin, DS Bug, DE Polev, OV Kosarev, RV Klementeva, EA Izmailova, IV Kazantsev, MS Khalipskaia, MO Goloshchapova, OS Yudintseva, IM Barkhatov, NV Petukhova, LS Zubarovskaya, AD Kulagin and IS Moiseev. Safety, feasibility, and advantages of oral microbiota transplantation: The first clinical case. J. Pediatr. Hematol. Oncol. 2024; 46, 287-96.
E Giannoni, D Baud, VD Agri, GR Gibson and G Reidd. Probiotics and COVID-19. Lancet Gastroenterol. Hepatol. 2020; 5, 720-1.
YP Silva, A Bernardi and RL Frozza. The role of short-chain fatty acids from gut microbiota in gut-brain communication. Front. Endocrinol. 2020; 11, 25.
CE Santo, C Caseiro, MJ Martins, R Monteiro and I Brandão. Gut microbiota, in the halfway between nutrition and lung function. Nutrients 2021; 13, 1716.
M Teymoori-Rad, F Shokri, V Salimi and SM Marashi. The interplay between vitamin D and viral infections. Rev. Med. Virol. 2019; 29, e2032.
M Teymoori-Rad and SM Marashi. Vitamin D and Covid-19: From potential therapeutic effects to unanswered questions. Rev. Med. Virol. 2021; 31, e2159.
M Jabczyk, J Nowak, B Hudzik and B Zubelewicz-Szkodzińska. Microbiota and its impact on the immune system in COVID-19 - A narrative review. J. Clin. Med. 2021; 10, 4537.
K Berding, K Vlckova, W Marx, H Schellekens, C Stanton, G Clarke, F Jacka, TG Dinan and JF Cryan. Diet and the microbiota-gut-brain axis: Sowing the seeds of good mental health. Adv. Nutr. 2021; 12, 1239-85.
J Hu, L Zhang, W Lin, W Tang, FKL Chan and SC Ng. Review article: Probiotics, prebiotics and dietary approaches during COVID-19 pandemic. Trends Food Sci. Tech. 2021; 108, 187-96.
A Bertuccioli, GB Zonzini, M Cazzaniga, M Cardinali, FD Pierro, A Gregoretti, N Zerbinati, L Guasti, MR Matera, I Cavecchia and CM Palazzi. Sports-Related Gastrointestinal Disorders: From the microbiota to the possible role of nutraceuticals, a narrative analysis. Microorganisms 2024; 12, 804.
LR Dowling, MR Strazzari, S Keely and GE Kaiko. Enteric nervous system and intestinal epithelial regulation of the gut-brain axis. J. Allergy Clin. Immunol. 2022; 150, 513-22.
K Sanada, S Nakajima, S Kurokawa, A Barceló-Soler, D Ikuse, A Hirata, A Yoshizawa, Y Tomizawa, M Salas-Valero, Y Noda, M Mimura, A Iwanami and T Kishimoto. Gut microbiota and major depressive disorder: A systematic review and meta-analysis. J. Affect. Disord. 2020; 266, 1-13.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2024 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






