Claudin-4 Expression as a Prognostic Biomarker in Colorectal Adenocarcinoma: Correlation with Lymphovascular Invasion, Lymph Node Metastasis, and Pathological Stage
DOI:
https://doi.org/10.48048/tis.2026.11956Keywords:
Colorectal adenocarcinoma, Claudin-4, Lymphovascular invasion, Lymph node metastasis, Prognostic biomarker, Pathological stage, Colorectal adenocarcinoma, Claudin-4, Lymphovascular invasion, Lymph node metastasis, Prognostic biomarkerAbstract
Colorectal cancer (CRC) remains a leading cause of cancer mortality worldwide, with increasing incidence in Asia, including Indonesia. Claudin-4, a tight junction protein, plays a paradoxical role in epithelial barrier function and tumor progression. This study aimed to investigate the relationship between Claudin-4 expression and major prognostic parameters in colorectal adenocarcinoma. A total of 104 formalin-fixed paraffin-embedded tissue blocks of colorectal adenocarcinoma were analyzed immunohistochemically. Claudin-4 expression was categorized as strong (79.8%) or weak (20.2%) based on the Total Immunostaining Score (TIS). Statistical analysis revealed no significant association between Claudin-4 expression and age, sex, tumor location, or size. However, Claudin-4 expression was significantly negatively correlated with lymphovascular invasion (p = 0.020; OR = 0.314, 95% CI 0.114 - 0.861), lymph node metastasis (p = 0.011; OR = 0.283, 95% CI 0.103 - 0.778), and pathological stage (p = 0.028). No significant correlation was observed with distant metastasis. These findings suggest that Claudin-4 may serve as a prognostic biomarker reflecting tumor invasiveness, supporting its potential role in guiding risk stratification in CRC patients.
HIGHLIGHTS
- Most colorectal adenocarcinoma cases (79.8%) showed strong Claudin-4 expression by immunohistochemistry.
- Low Claudin-4 expression was significantly linked to lymphovascular invasion and lymph node metastasis.
- Strong Claudin-4 expression was more common in early pathological stages, while advanced stages showed reduced expression.
- This study provides the first evidence from Indonesia on the prognostic role of Claudin-4 in colorectal adenocarcinoma.
- Findings support Claudin-4 as a promising biomarker to improve risk stratification in colorectal cancer patients.
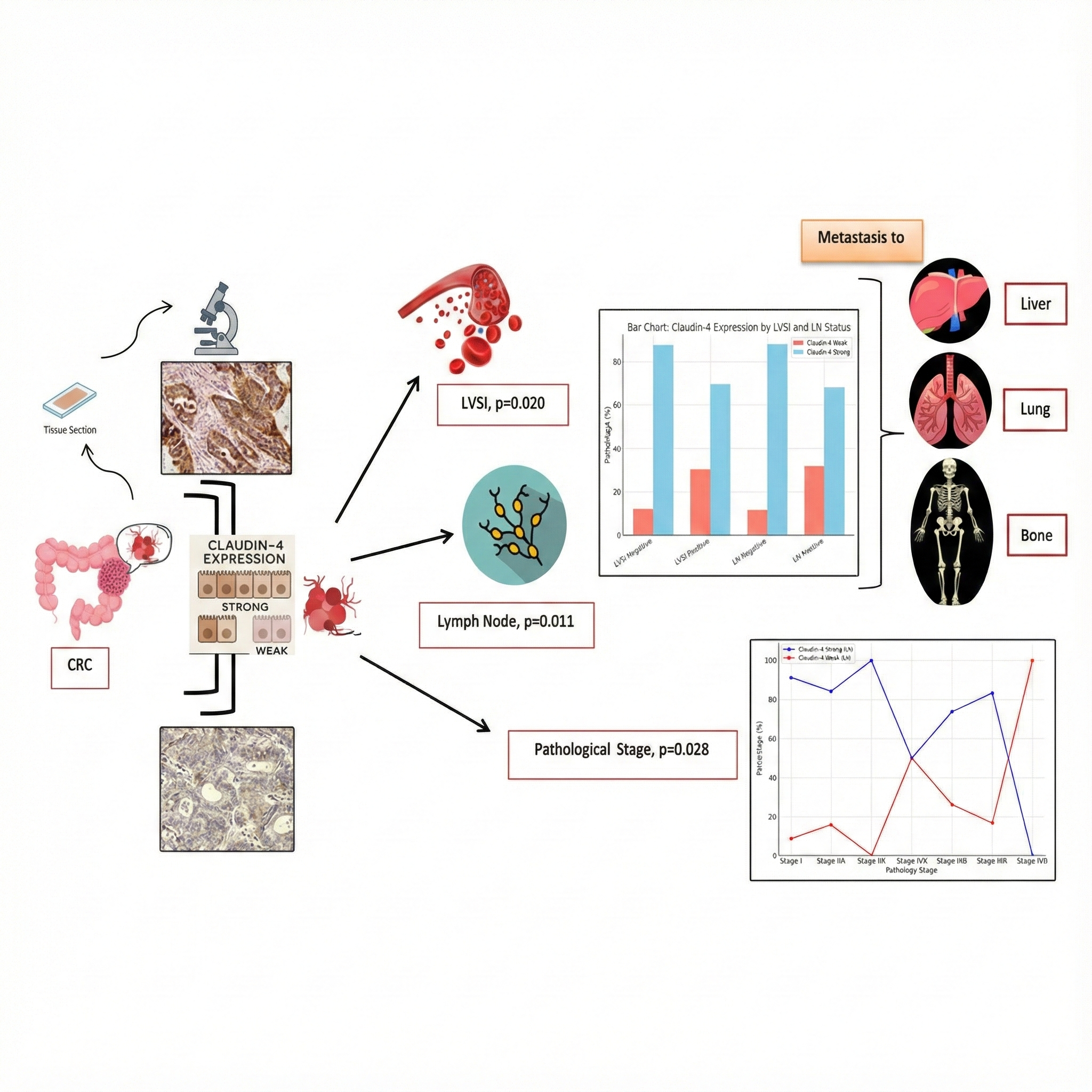
GRAPHICAL ABSTRACT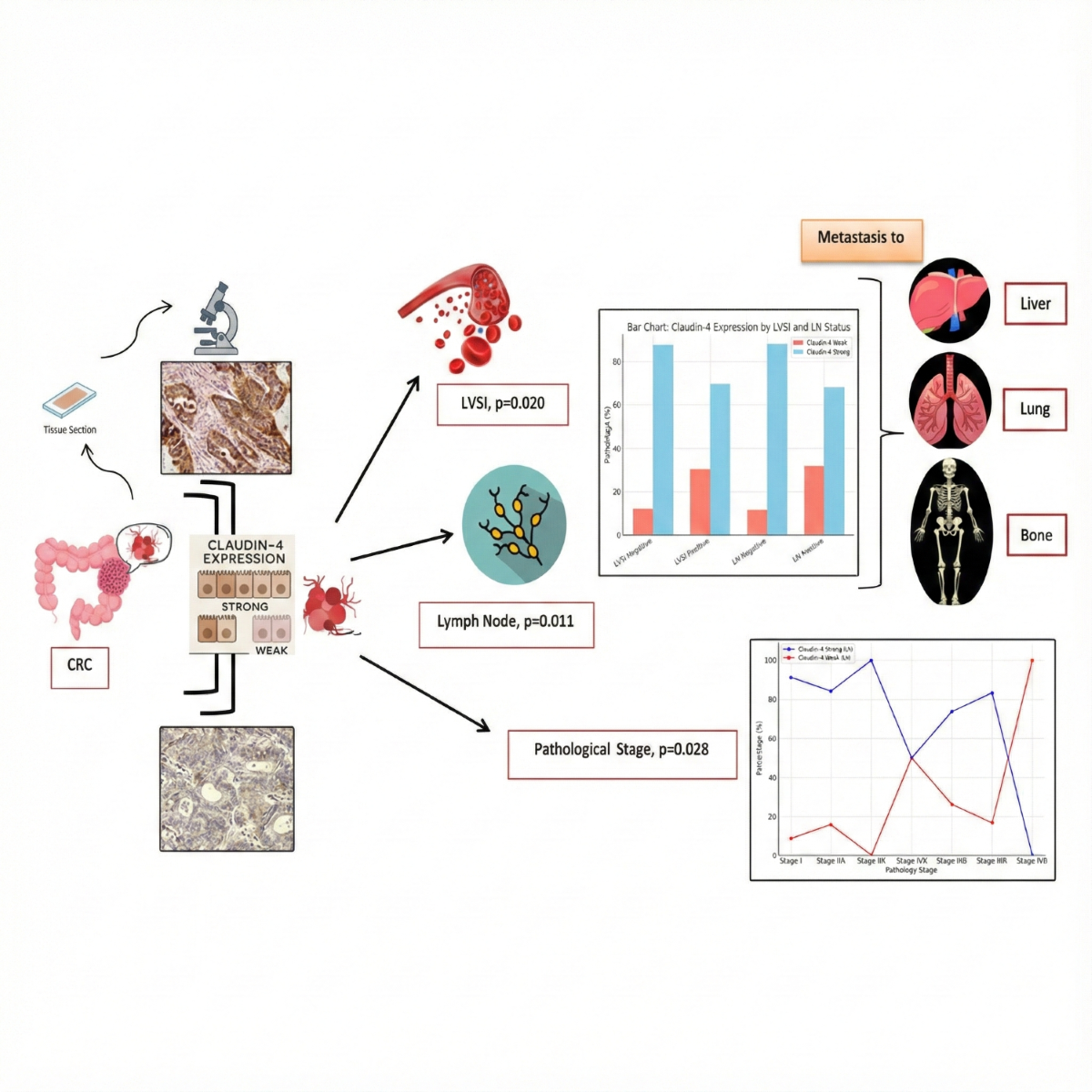
Downloads
References
F Bray, M Laversanne, H Sung, J Ferlay, RL Siegel, I Soerjomataram and A Jemal. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: A Cancer Journal for Clinicians 2024; 74(3), 229-263.
RL Siegel, KD Miller, AG Sauer, SA Fedewa, LF Butterly, JC Anderson, A Cercek, RA Smith and A Jemal. Colorectal cancer statistics, 2020. CA: A Cancer Journal for Clinicians 2020; 70(3), 145-164.
P Tantimetta, T Rattanaarchanai, A Aroonkesorn, W Chanket, P Runsaeng, S Roytrakul, P Hutamekalin and S Obchoei. Recombinant bacteriocin rhamnosin suppresses malignant phenotypes of colorectal cancer cells. Trends in Sciences 2025; 22(8), 10057.
AE Noffsinger. Fenoglio-Preiser’s gastrointestinal pathology. Lippincott Williams & Wilkins, New York, 2017.
UA Miskad, MM Henry, CI Pardamean, A Budiarto, A Irwan, JW Baurley, I Yusuf and B Pardamean. Colorectal cancer in south sulawesi: A case-control study for nongenetic risk factors. Oncology Reviews 2025; 19, 1589655.
X Wang, Y Cao, M Ding, J Liu, X Zuo, H Li and R Fan. Oncological and prognostic impact of lymphovascular invasion in colorectal cancer patients. International Journal of Medical Sciences 2021; 18(7), 1721.
AM Rianti, MH Cangara, A Yamin, H Dahlan, MR Ilyasa and UA Miskad. FGFR2 as a prognostic and predictive marker in colorectal adenocarcinoma based on tils grade. The Indonesian Biomedical Journal 2025; 17(2), 188-196.
R Fujiwara-Tani, S Mori, R Ogata, R Sasaki, A Ikemoto, S Kishi, M Kondoh and H Kuniyasu. Claudin-4: A new molecular target for epithelial cancer therapy. International Journal of Molecular Sciences 2023; 24(6), 5494.
N Roehlen, AA Roca Suarez, H El Saghire, A Saviano, C Schuster, J Lupberger and TF Baumert. Tight junction proteins and the biology of hepatobiliary disease. International Journal of Molecular Sciences 2020; 21(3), 825.
CD Hough, CA Sherman-Baust, ES Pizer, FJ Montz, DD Im, NB Rosenshein, KR Cho, GJ Riggins and PJ Morin. Large-scale serial analysis of gene expression reveals genes differentially expressed in ovarian cancer. Cancer Research 2000; 60(2), 6281-6287.
C Hana, NN Thaw Dar, M Galo Venegas and M Vulfovich. Claudins in cancer: A current and future therapeutic target. International Journal of Molecular Sciences 2024; 25(9), 4634.
J Li. Context-dependent roles of claudins in tumorigenesis. Frontiers in Oncology 2021; 11, 67681.
OP Popova, AV Kuznetsova, SY Bogomazova and AA Ivanov. Claudins as biomarkers of differential diagnosis and prognosis of tumors. Journal of Cancer Research and Clinical Oncology 2021; 147(10), 2803-2817.
H Sung, J Ferlay, RL Siegel, M Laversanne, I Soerjomataram, A Jemal and F Bray. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: A Cancer Journal for Clinicians 2021; 71(3), 209-249.
T Sawicki, M Ruszkowska, A Danielewicz, E Niedźwiedzka, T Arłukowicz and KE Przybyłowicz. A review of colorectal cancer in terms of epidemiology, risk factors, development, symptoms and diagnosis. Cancers 2021; 13(9), 2025.
M Ahmed. Colon cancer: A clinician’s perspective in 2019. Gastroenterology Research 2020; 13(1), 1.
M Abancens, V Bustos, H Harvey, J McBryan and BJ Harvey. Sexual dimorphism in colon cancer. Frontiers in Oncology 2020; 10, 607909.
O Majek, A Gondos, L Jansen, K Emrich, B Holleczek, A Katalinic, A Nennecke, A Eberle and H Brenner. Sex differences in colorectal cancer survival: Population-based analysis of 164,996 colorectal cancer patients in Germany. PLoS One 2013; 8(7), e68077.
F Caiazza, EJ Ryan, G Doherty, DC Winter and K Sheahan. Estrogen receptors and their implications in colorectal carcinogenesis. Frontiers in Oncology 2015; 5, 19.
P Rawla, T Sunkara and A Barsouk. Epidemiology of colorectal cancer: Incidence, mortality, survival, and risk factors. Gastroenterology Review/Przegląd Gastroenterologiczny 2019; 14(2), 89-103.
I Theodora, IK Sudiana, VS Budipramana, F Erwin, S Dewi and BD Novita. Tumor differentiation is correlated with Estrogen Receptor Beta (ERβ) expression but not with Interleukin-6 (IL-6) expression in colorectal carcinoma. The Indonesian Biomedical Journal 2024; 16(5), 481-486.
J Ueda, S Semba, H Chiba, N Sawada, Y Seo, M Kasuga and H Yokozaki. Heterogeneous expression of claudin-4 in human colorectal cancer: Decreased claudin-4 expression at the invasive front correlates cancer invasion and metastasis. Pathobiology 2007; 74(1), 32-41.
H Ueno, H Mochizuki, Y Hashiguchi, H Shimazaki, S Aida, K Hase, S Matsukuma, T Kanai, H Kurihara, K Ozawa, K Yoshimura and S Bekku. Risk factors for an adverse outcome in early invasive colorectal carcinoma. Gastroenterology 2004; 127(2), 385-394.
Y Wang, X Zhong, X He, Z Hu, H Huang, J Chen, K Chen, S Zhao, P Wei and D Li. Liver metastasis from colorectal cancer: Pathogenetic development, immune landscape of the tumour microenvironment and therapeutic approaches. Journal of Experimental & Clinical Cancer Research 2023; 42(1), 177.
J Martin, A Petrillo, EC Smyth, N Shaida, S Khwaja, HK Cheow, A Duckworth, P Heister, R Praseedom, A Jah, A Balakrishnan, S Harper, S Liau, V Kosmoliaptsis and E Huguet. Colorectal liver metastases: Current management and future perspectives. World Journal of Clinical Oncology 2020; 11(10), 761-808.
M Riihimäki, A Hemminki, J Sundquist and K Hemminki. Patterns of metastasis in colon and rectal cancer. Scientific Reports 2016; 6, 29765.
R Fujiwara-Tani, T Sasaki, YI Luo, K Goto, I Kawahara, Y Nishiguchi, S Kishi, S Mori, H Ohmori, M Kondoh and H Kuniyasu. Anti-claudin-4 extracellular domain antibody enhances the antitumoral effects of chemotherapeutic and antibody drugs in colorectal cancer. Oncotarget 2018; 9(100), 37367.
D Süren, M Yıldırım, V Kaya, AS Alikanoğlu, N Bülbüller, M Yıldız and C Sezer. Loss of tight junction proteins (Claudin 1, 4, and 7) correlates with aggressive behavior in colorectal carcinoma. Medical Science Monitor: International Medical Journal of Experimental and Clinical Research 2014; 20, 1255.
D Kyuno, A Takasawa, S Kikuchi, I Takemasa, M Osanai and T Kojima. Role of tight junctions in the epithelial-to-mesenchymal transition of cancer cells. Biochimica et Biophysica Acta (BBA)-Biomembranes 2021; 1863(3), 183503.
S Ersoz, S Mungan, U Cobanoglu, H Turgutalp and Y Ozoran. Prognostic importance of Claudin-1 and Claudin-4 expression in colon carcinomas. Pathology - Research and Practice 2011; 207(5), 285-289.
KE Cox, S Liu, RM Hoffman, SK Batra, P Dhawan and M Bouvet. The expression of the claudin family of proteins in colorectal cancer. Biomolecules 2024; 207(5), 285-289.
Y Tokuhara, T Morinishi, T Matsunaga, H Ohsaki, Y Kushida, R Haba and E Hirakawa. Claudin-1, but not claudin-4, exhibits differential expression patterns between well- to moderately-differentiated and poorly-differentiated gastric adenocarcinoma. Oncology Letters 2015; 10(1), 93-98.
DW Wang, WH Zhang, G Danil, K Yang and JK Hu. The role and mechanism of claudins in cancer. Frontiers in Oncology 2022; 12, 1051497.
B Baran, NM Ozupek, NY Tetik, E Acar, O Bekcioglu and Y Baskin. Difference between left-sided and right-sided colorectal cancer: A focused review of literature. Gastroenterology Research 2018; 11(4), 264.
G Menon, A Recio-Boiles, S Lotfollahzadeh and B Cagir. Colon cancer. StatPearls Publishing, Florida, United States, 2023.
J Yang, P Antin, G Berx, C Blanpain, T Brabletz, M Bronner, K Campbell, A Cano, J Casanova, G Christofori, S Dedhar, R Derynck, HL Ford, J Fuxe, AG de Herreros, GJ Goodall, AK Hadjantonakis, RYJ Huang and C Kalcheim. Guidelines and definitions for research on epithelial - mesenchymal transition. Nature Reviews Molecular Cell Biology 2020; 21(6), 341-352.
W Li, SQ Zong, Q Shi, HJ Li, J Xu and F Hou. Hypoxia-induced vasculogenic mimicry formation in human colorectal cancer cells: Involvement of HIF-1a, Claudin-4, and E-cadherin and Vimentin. Scientific Reports 2016; 6(1), 37534.
NА Nefedova, ОА Kharlova and PG Malkov. Еxpression of claudin-1, 3, and 4 in colorectal cancer and polyps. Arkhiv Patologii 2016; 78(3), 11-19.
L Wang, SY Li, P An and HY Cai. Expression and clinical significance of Claudin-1 and Claudin-4 in colorectal cancer tissues. Zhonghua wei Chang wai ke za zhi= Chinese Journal of Gastrointestinal Surgery 2012; 15(10), 1073-1076.
S Fatimah, AS Rahaju and A Rahniayu. Role of claudin-4 and matrix metalloproteinase-2 in tumor invasion of colorectal adenocarcinoma. Research Journal of Pharmacy and Technology 2021; 14(9), 4795-4800.
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






