Potential of Probiotics as Adjuvant Therapy to Reduce Depressive Disorder Based on Dose and Duration: A Meta-Analysis
DOI:
https://doi.org/10.48048/tis.2025.10622Keywords:
Probiotics, Depression, Depressive Disorder, Gut-Brain Axis, Randomized Controlled Trials, Meta-Analysis, Depression, Depressive disorder, Gut-brain axis, Meta-analysis, Probiotics, Randomized controlled trialsAbstract
Depression is a common and severe mood disorder affecting millions globally. Recent research suggests that probiotics may play a role in reducing symptoms of depression. Integrating probiotics into clinical practice can enhance patient outcomes, improve quality of life, and advance the overall care of individuals with depressive disorders. This meta-analysis aims to evaluate the effectiveness of probiotics as an adjunctive therapy for disorders. It focuses on determining the impact of probiotic dosage, duration, and specific strains on reducing depressive symptoms by modulating gut microbiota, which is implicated in the gut-brain axis and mental health. A systematic search on randomized controlled trials (RCTs) was conducted in PubMed, Scopus, and the Cochrane Library from 2019 to 2024, PRISMA guidelines for examining probiotics on depression. The selected studies met predefined inclusion criteria, including validated depression assessment scales. Data extraction involved a standardized form, and a meta-analysis was conducted using Rev 5.4 with a random-effects model to account for variations across studies. Our study showed that probiotics significantly reduce symptoms in patients with major depressive disorder (SMD = −0.37, 95% CI −0.64 to −0.10, p = 0.007) and in cases of mild to moderate depressive disorders (SMD = −0.75, 95% CI −0.17 to −0.33, p = 0.0004). A daily probiotic dose of 3×10⁹ CFU administered over 8-weeks was associated with a reduction in depressive symptoms, regardless of the initial severity of the condition. In individuals diagnosed with major depressive disorder (MDD), a higher dosage of 8×10⁹ CFU over the same duration yielded more pronounced therapeutic effects. These results contribute to the evidence supporting the role of the gut-brain axis in the pathophysiology of depression. They also highlight the potential of probiotics as adjunctive agents in depression management, thereby informing the development of evidence-based clinical guidelines for integrative treatment strategies.
HIGHLIGHTS
This study highlights that specific probiotics, dosages, and durations may reduce depressive symptoms. Clinicians should consider discussing probiotic options with patients and collaborating with other health workers to integrate this approach into comprehensive treatment plans.
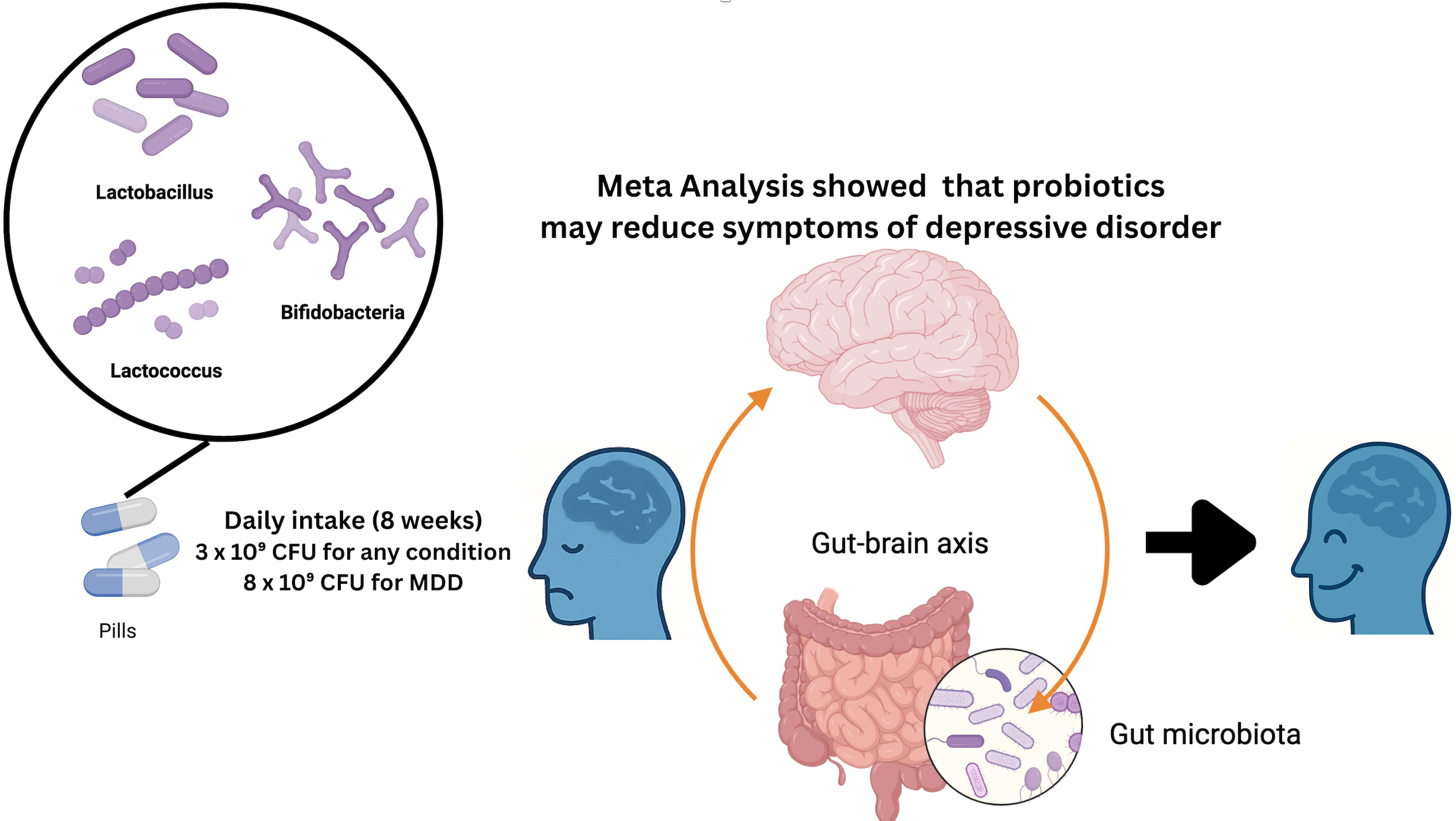
GRAPHICAL ABSTRACT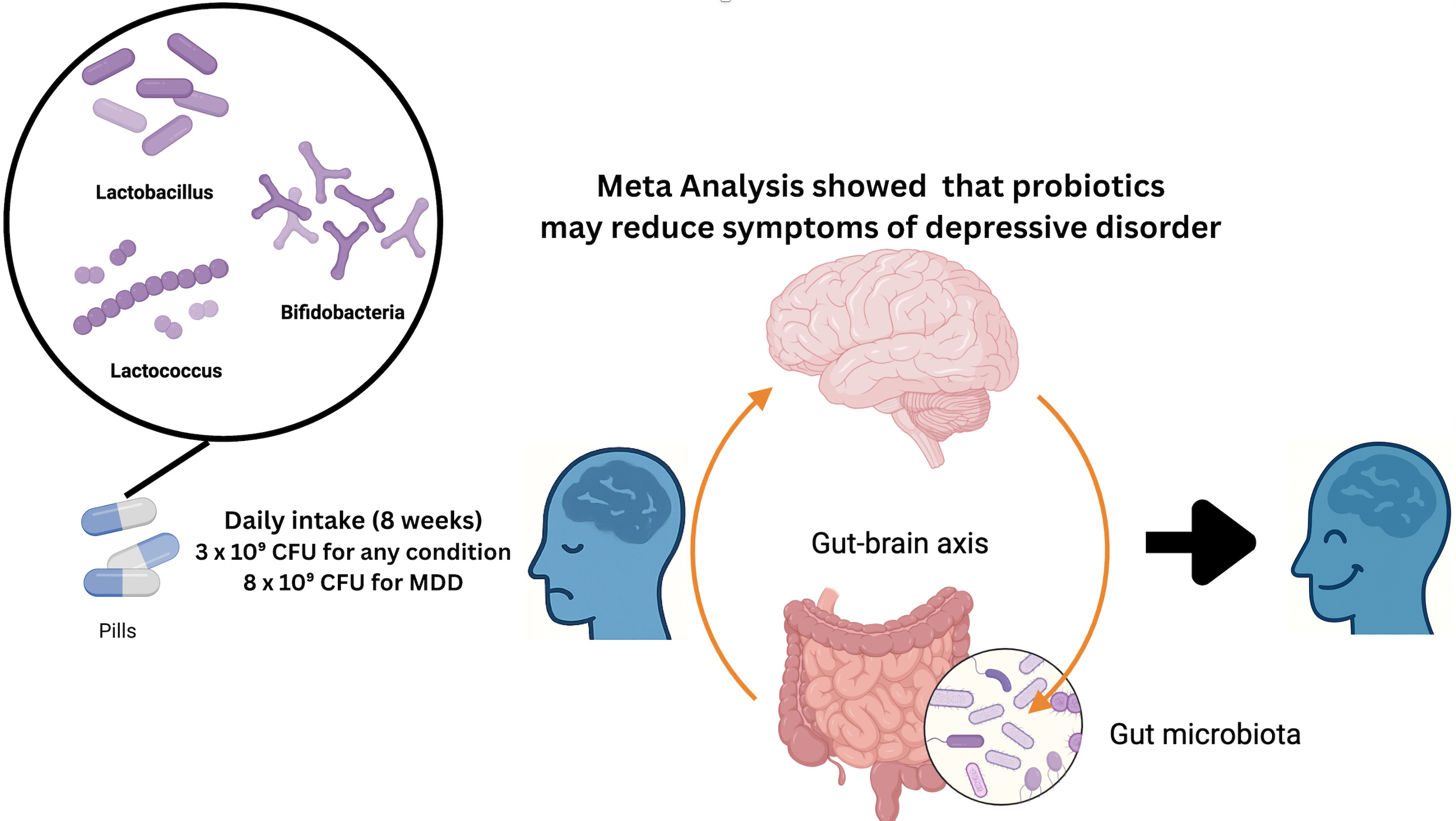
Downloads
References
World Health Organization, Available at: https://www.who.int, accessed June 2024.
CJK Wallace and RV Milev. The Efficacy, Safety, and Tolerability of probiotics on depression: Clinical results from an open-label pilot study. Frontiers in Psychiatry 2021; 12, 612879.
VL Nikolova, AJ Cleare, AH Young and JM Stone. Acceptability, Tolerability and Estimates of putative treatment effects of probiotics as adjunctive treatment in patients with depression: A randomized clinical trial. JAMA Psychiatry 2023; 80(8), 842-847.
AC Schaub, E Schneider, JF Vazquez-Castellanos, N Schweinfurth, C Kettelhack, JPK Doll, G Yamanbaeva, L Mahlmann, S Brand, C Beglinger, S Borgwardt, J Raes, A Schmidt and UE Lang. Clinical, gut microbial and neural effects of a probiotic add-on therapy in depressed patients: A randomized controlled trial. Translational Psychiatry 2022; 12(1), 277.
SJ Yong, T Tong, J Chew and WL Lim. Antidepressive mechanisms of probiotics and their therapeutic potential. Frontiers in Neuroscience 2020; 14, 1361.
O Gawlik-Kotelnicka, A Margulska, K Pleska, A Skowronska and D Strzelecki. Metabolic status influences probiotic efficacy for depression-pro-demet randomized clinical trial results. Nutrients 2024; 16(9), 1389.
MJ Page, JE McKenzie, PM Bossuyt, I Boutron, TC Hoffmann, CD Mulrow, L Shamseer, JM Tetzlaff, EA Akl, SE Brennan, R Chou, J Glanville, JM Grimshaw, A Hrobjartsson, MM Lalu, T Li, EW Loder, E Mayo-Wilson, S McDonald, LA McGuinness, ..., D Moher. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021; 372, 71.
AT Beck, RA Steer and MG Carbin. Psychometric properties of the beck depression inventory: Twenty-five years of evaluation. Clinical Psychology Review 1988; 8(1), 77-100.
RA Steer, AT Beck, JH Riskind and G Brown. Relationships between the beck depression inventory and the hamilton psychiatric rating scale for depression in depressed outpatients. Journal of Psychopathology and Behavioral Assessment 1987; 9(3), 327-339.
R DerSimonian and N Laird. Meta-analysis in clinical trials revisited. Contemporary Clinical Trials 2015; 45, 139-145.
P Higgins, DG Altman, PC Gøtzsche, P Jüni, D Moher, AD Oxman, J Savovic, KF Schulz, L Weeks, JA Sterne. The Cochrane Collaboration's tool for assessing risk of bias in randomised trials. BMJ. 2011; 343, d5928.
JAC Sterne, J Savović, MJ Page, RG Elbers, NS Blencowe, I Boutron, CJ Cates, H-Y Cheng, MS Corbett, SM Eldridge, MA Hernán, S Hopewell, A Hróbjartsson, DR Junqueira, P Jüni, JJ Kirkham, T Lasserson, T Li, A McAleenan, BC Reeves,..., JPT Higgins. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 2019; 366, l4898.
HJ Lee, JK Hong, JK Kim, DH Kim, SW Jang, SW Han, and IY Yoon. Effects of probiotic nvp-1704 on mental health and sleep in healthy adults: An 8-week randomized, double-blind, placebo-controlled trial. Nutrients 2021; 13(8), 2660.
K Kreuzer, A Reiter, AM Birkl-Toglhofer, N Dalkner, S Morkl, M Mairinger, E Fleischmann, F Fellendorf, M Platzer, M Lenger, T Farber, M Seidl, A Birner, R Queissner, LMS Mendel, A Maget, A Kohlhammer-Dohr, A Haussl, J Wagner-Skacel, H Schoggl,... , S Bengesser. The PROVIT study-effects of multispecies probiotic add-on treatment on metabolomics in major depressive disorder-a randomized, placebo-controlled trial. Metabolites 2022; 12(8), 770.
EZ Reininghaus, M Platzer, A Kohlhammer-Dohr, C Hamm, S Morkl, SA Bengesser, FT Fellendorf, T Lahousen-Luxenberger, B Leitner-Afschar, H Schoggl, D Amberger-Otti, W Wurm, R Queissner, A Birner, VS Falzberger, A Painold, W Fitz, J Wagner-Skacel, M Brunnmayr, A Rieger,... , N Dalkner. Provit: Supplementary probiotic treatment and vitamin b7 in depression-a randomized controlled trial. Nutrients 2020; 12(11), 3422.
J Moludi, M Alizadeh, MHS Mohammadzad and M Davari. The effect of probiotic supplementation on depressive symptoms and quality of life in patients after myocardial infarction: Results of a preliminary double-blind clinical trial. Psychosomatic medicine 2019; 81(9), 770-777.
B Chahwan, S Kwan, A Isik, S van Hemert, C Burke and L Roberts. Gut feelings: A randomised, triple-blind, placebo-controlled trial of probiotics for depressive symptoms. Journal of Affective Disorders 2019; 253, 317-326.
D Johnson, S Thurairajasingam, V Letchumanan, KG Chan and LH Lee. Exploring the role and potential of probiotics in the field of mental health: Major depressive disorder. Nutrients 2021; 13(5), 1728.
HM Chen, PH Kuo, CY Hsu, YH Chiu, YW Liu, ML Lu and CH Chen. Psychophysiological effects of lactobacillus plantarum ps128 in patients with major depressive disorder: A preliminary 8-Week open trial. Nutrients 2021; 13(11), 3731.
SJ Yong, T Tong, J Chew and WL Lim. Antidepressive mechanisms of probiotics and their therapeutic potential. Frontiers in Neuroscience 2020; 13, 1361.
Q Zhang, B Chen, J Zhang, J Dong, J Ma, Y Zhang, K Jin and J Lu. Effect of Prebiotics, Probiotics, Synbiotics on Depression: Results from a meta-analysis. BMC Psychiatry 2023; 23(1), 477.
AC Schaub, E Schneider, JF Vazquez-Castellanos, N Schweinfurth, C Kettelhack, JPK Doll, G Yamanbaeva, L Mahlmann, S Brand, C Beglinger, S Borgwardt, J Raes, A Schmidt and UE Lang. Clinical, gut microbial and neural effects of a probiotic add-on therapy in depressed patients: A randomized controlled trial. Translational Psychiatry 2022; 12(1), 227.
M Egger, GD Smith, M Schneider and C Minder. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997; 315(7109), 629-634.
JAC Sterne, AJ Sutton, JPA Ioannidis, N Terrin, DR Jones, J Lau, J Carpenter, G Rucker, RM Harbord, CH Schmid, J Tetzlaff, JJ Deeks, J Peters, P Macaskill, G Schwarzer, S Duval, DG Altman, D Moher and JPT Higgins. Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ 2011; 343, 4002.
K Kreuzer, AM Birkl-Toeglhofer, J Haybaeck, A Reiter, N Dalkner, FT Fellendorf, A Maget, M Platzer, M Seidl, LM Mendel, M Lenger, A Birner, R Queissner, M Mairinger, A Obermayer, A Kohlhammer-Dohr, TM Stross, A Haussl, C Hamm, H Schoggl,... , SA Bengesser. PROVIT-CLOCK: A potential influence of probiotics and vitamin b7 add-on treatment and metabolites on clock gene expression in major depression. Neuropsychobiology 2024; 83(3-4), 135-151.
J Companys, L Pla-Paga, L Calderon-Perez, E Llaurado, R Sola, A Pedret and RM Valls. Fermented dairy products, probiotic supplementation, and cardiometabolic diseases: A systematic review and meta-analysis. Advances in Nutrition 2020; 11(4), 843-863.
N Hamjane, MB Mechita, NG Nourouti and A Barakat. Gut microbiota dysbiosis -associated obesity and its involvement in cardiovascular diseases and type 2 diabetes. A systematic review. Microvascular Research 2024; 151, 104601.
M Jiang, L Kang, YL Wang, B Zhou, HY Li, Q Yan and ZG Liu. Mechanisms of microbiota-gut-brain axis communication in anxiety disorders. Frontiers in Neuroscience 2024; 18, 1501134.
X Chang, Y Zhang, X Chen, S Li, H Mei, H Xiao, X Ma, Z Liu and R Li. Gut microbiome and serum amino acid metabolome alterations in autism spectrum disorder. Scientific Reports 2024; 14(1), 4037.
Q Wang, Q Yang and X Liu. The microbiota-gut-brain axis and neurodevelopmental disorders. Protein Cell 2023; 14(10), 762-775.
J Zhao, J Liu, J Feng, X Liu and Q Hu. The gut microbiota-brain connection: Insights into major depressive disorder and bipolar disorder. Frontiers in Psychiatry 2024; 15, 1421490.
JR Kelly, AP Allen, A Temko, W Hutch, PJ Kennedy, N Farid, E Murphy, G Boylan, J Bienenstock, JF Cryan, G Clarke and TG Dinan. Lost in translation? The potential psychobiotic Lactobacillus rhamnosus (JB-1) fails to modulate stress or cognitive performance in healthy male subjects. Brain, Behavior, and Immunity 2017; 61, 50-59.
H Rong, XH Xie, J Zhao, WT Lai, MB Wang, D Xu, YH Liu, YY Guo, SX Xu, WF Deng, QF Yang, L Xiao, YL Zhang, FS He, S Wang and TB Liu. Similarly in depression, nuances of gut microbiota: Evidences from a shotgun metagenomics sequencing study on major depressive disorder versus bipolar disorder with current major depressive episode patients. Journal of Psychiatric Research 2019; 113, 90-99.
E Aizawa, H Tsuji, T Asahara, T Takahashi, T Teraishi, S Yoshida, M Ota, N Koga, K Hattori and H Kunugi. Possible association of Bifidobacterium and Lactobacillus in the gut microbiota of patients with major depressive disorder. Journal of Affective Disorders 2016; 202, 254-257.
H Luan, X Wang and Z Cai. Mass spectrometry-based metabolomics: Targeting the crosstalk between gut microbiota and brain in neurodegenerative disorders. Mass Spectrometry Reviews 2019; 38(1), 22-33.
M Schirmer, SP Smeekens, H Vlamakis, M Jaeger, M Oosting, EA Franzosa, RT Horst, T Jansen, L Jacobs, MJ Bonder, A Kurilshikov, J Fu, LAB Joosten, A Zhernakova, C Huttenhower, C Wijmenga, MG Netea and RJ Xavier. Linking the Human Gut Microbiome to Inflammatory Cytokine Production Capacity. Cell 2016; 167(4), 1125-1136.
Z Ghorbani, S Nazari, F Etesam, S Nourimajd, M Ahmadpanah and SR Jahromi. The effect of synbiotic as an adjuvant therapy to fluoxetine in moderate depression: A randomized multicenter trial. Archives of Neuroscience 2018; 5(2), 60507.
J Godos, W Currenti, D Angelino, P Mena, S Castellano, F Caraci, F Galvano, DD Rio, R Ferri and G Grosso. Diet and mental health: Review of the recent updates on molecular mechanisms. Antioxidants 2020; 9(4), 346.
SZ Alamdary, B Bakhshi and S Soudi. The anti-apoptotic and anti-inflammatory effect of Lactobacillus acidophilus on Shigella sonnei and vibrio cholerae interaction with intestinal epithelial cells: A comparison between invasive and non-invasive bacteria. PLoS One 2018; 13(6), 0196941.
A Najarian, S Sharif and MW Griffiths. Evaluation of protective effect of Lactobacillus acidophilus La-5 on toxicity and colonization of Clostridium difficile in human epithelial cells in vitro. Anaerobe 2019; 55, 142-151.
LC Lew, YY Hor, NAA Yusoff, SB Choi, MSB Yusoff, NS Roslan, A Ahmad, JAM Mohammad, MFIL Abdullah, N Zakaria, N Wahid, Z Sun, LY Kwok, H Zhang and MT Liong. Probiotic Lactobacillus plantarum P8 alleviated stress and anxiety while enhancing memory and cognition in stressed adults: A randomised, double-blind, placebo-controlled study. Clinical Nutrition 2019; 38(5), 2053-2064.
A Kazemi, AA Noorbala, K Azam and K Djafarian. Effect of prebiotic and probiotic supplementation on circulating pro-inflammatory cytokines and urinary cortisol levels in patients with major depressive disorder: A double-blind, placebo-controlled randomized clinical trial. Journal of Functional Foods 2019; 52, 596-602.
L Huang, Z Ma, X Ze, X Zhao, M Zhang, X Lv, Y Zheng and H Liu. Gut microbiota decreased inflammation induced by chronic unpredictable mild stress through affecting NLRP3 inflammasome. Frontiers in Cellular and Infection Microbiology 2023; 13, 1189008.
N Li, Q Wang, Y Wang, A Sun, Y Lin, Y Jin and X Li. Oral probiotics ameliorate the behavioral deficits induced by chronic mild stress in mice via the gut microbiota-inflammation axis. Frontiers in Behavioral Neuroscience 2018; 12, 266.
VL Nikolova, AJ Cleare, AH Young and J Stone. Updated review and meta-analysis of probiotics for the treatment of clinical depression: Adjunctive vs. stand-alone treatment. Journal of Clinical Medicine 2021; 10(4), 647.
N Heidarzadeh-Rad, H Gokmen-Ozel, A Kazemi, N Almasi and K Djafarian. Effects of a psychobiotic supplement on serum brain-derived neurotrophic factor levels in depressive patients: A post hoc analysis of a randomized clinical trial. Journal of Neurogastroenterology and Motility 2020; 26(4), 486-495.
QX Ng, YL Lim, CYL Yaow, W Ng, J Thumboo and TM Liew. Effect of probiotic supplementation on gut microbiota in patients with major depressive disorders: A systematic review. Nutrients 2023; 15(6), 1351.
Y Guo, JP Xie, K Deng, X Li, Y Yuan, Q Xuan, J Xie, XM He, Q Wang, JJ Li and HR Luo. Prophylactic effects of bifidobacterium adolescentis on anxiety and depression-like phenotypes after chronic stress: A role of the gut microbiota-inflammation axis. Front Behav Neurosci 2019; 13, 126.
M Sikorska, AZ Antosik-Wojcinska and M Dominiak. Probiotics as a tool for regulating molecular mechanisms in depression: A systematic review and meta-analysis of randomized clinical trials. International Journal of Molecular Sciences 2023; 24(4), 3081.
MS Cepeda, EG Katz and C Blacketer. Microbiome-gut-brain axis: Probiotics and their association with depression. The Journal of Neuropsychiatry and Clinical Neurosciences 2017; 29(1), 39-44.
H Zulfiqar and U Aslam. Should probiotics be administered as an adjunctive treatment along with antidepressants for major depressive disorder?. Journal of the Pakistan Medical Association 2023; 74(1), 197.
X Li, JM Huan, L Lin and Y Hu. Association of systemic inflammatory biomarkers with depression risk: Results from national health and nutrition examination survey 2005-2018 analyses. Frontiers in Psychiatry 2023; 14, 1097196.
F Giannotta, KW Nilsson, C Aslund and P Larm. Among the swedish generation of adolescents who experience an increased trend of psychosomatic symptoms. Do they develop depression and/or anxiety disorders as they grow older?. BMC Psychiatry 2022; 22, 779.
M Clapp, N Aurora, L Herrera, M Bhatia, E Wilen and S Wakefield. Gut microbiota’s effect on mental health: The gut-brain axis. Clinics and Practice 2017; 7(4), 987.
C DʼMello, N Ronaghan, R Zaheer, M Dicay, T Le, WK MacNaughton, MG Surrette and MG Swain. Probiotics improve inflammation-associated sickness behavior by altering communication between the peripheral immune system and the brain. Journal of Neuroscience 2015; 35(30), 10821-10830.
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






