The Flow-Pressure and Cardiopulmonary Responses of Manual Chest Percussion with Different Ranges of Oscillation Frequency in Healthy Subjects
DOI:
https://doi.org/10.48048/tis.2024.7345Keywords:
Manual percussion, Chest physical therapy, Airway clearance technique, Convention chest physical therapy, Bronchial hygiene therapyAbstract
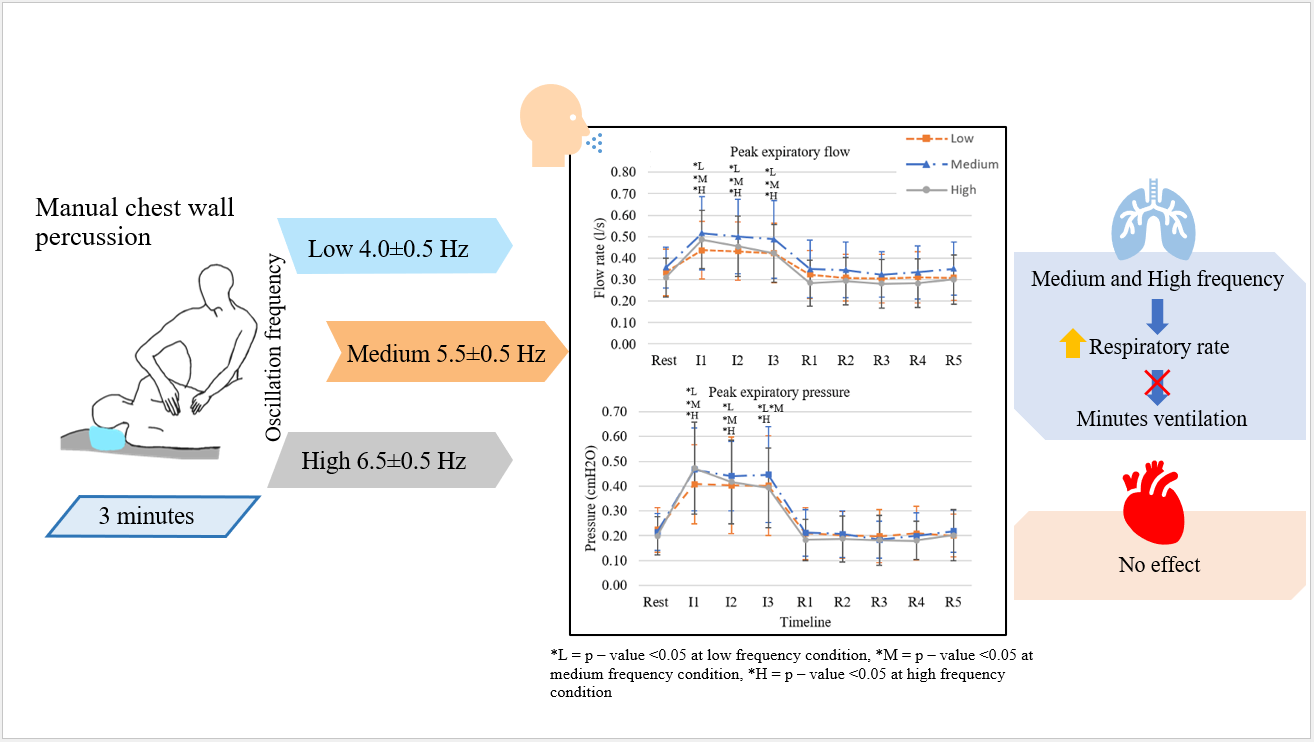
Manual chest wall percussion (MP) is a technique for secretion clearance which commonly use. However, MP is performed by physiotherapists throughout a broad range of the oscillation frequency, which might result in different physical properties and cardiopulmonary responses of MP. Investigate the flow, pressure and cardiorespiratory response during MP with 3 frequencies in healthy subjects. Twenty-one healthy subjects (8 men and 13 women) were recruited into this crossover study. MP was applied with 3 frequency ranges, including low (4.0 ± 0.5), medium (5.5 ± 0.5), and high (6.5 ± 0.5) Hz, for 3 min in the neutral side lying on left side. A flow sensor (Model SS11LA) and a pressure sensor (Model SS13L) were used to measure Inspiratory-expiratory (I-E) flow rate and pressure through mouth. A bedside monitor (BSM 2351k, Nihon Kohden) was used to measure cardiopulmonary response. All dependent variables were measured pre- (resting), during, and post- (recovery) MP application. Both I-E flow rate and pressure were increased from resting significantly in all frequencies MP, but they were not different among the 3 frequency ranges. The E flow rate was increased to 0.41 - 0.44, 0.49 - 0.52 and 0.41 - 0.49 L/s (min-max) during MP application at low, medium, and high frequency compared to resting (0.31 - 0.36 L/s), respectively. The E pressure was increased to 0.40 - 0.41, 0.44 - 0.47 and 0.39 - 0.47 cmH2O (min-max) during MP application at low, medium, and high frequency compared to resting (0.20 - 0.22 cm H2O), respectively. However, the increment of the 3 frequency ranges did not affect the cardiovascular functions except respiratory rate, which was increased only 2 breaths/min from resting. In conclusion, airflow and pressure were slightly increased during MP but did not affect cardiopulmonary functions in healthy subjects. Further study in patients is needed.
HIGHLIGHTS
- Manual chest wall percussion is a secretion clearance technique which commonly used.
- Whether manual chest wall percussion frequency is capable of increasing expiratory flow rate by the same amount.
- The percussion force might be the most prominent factor affecting the expiratory flow rate.
- The frequency of chest wall percussion does not affect cardiovascular response.
- Medium and high frequencies cause a minor rise in the respiratory rate but have no impact on minute ventilation.
GRAPHICAL ABSTRACT
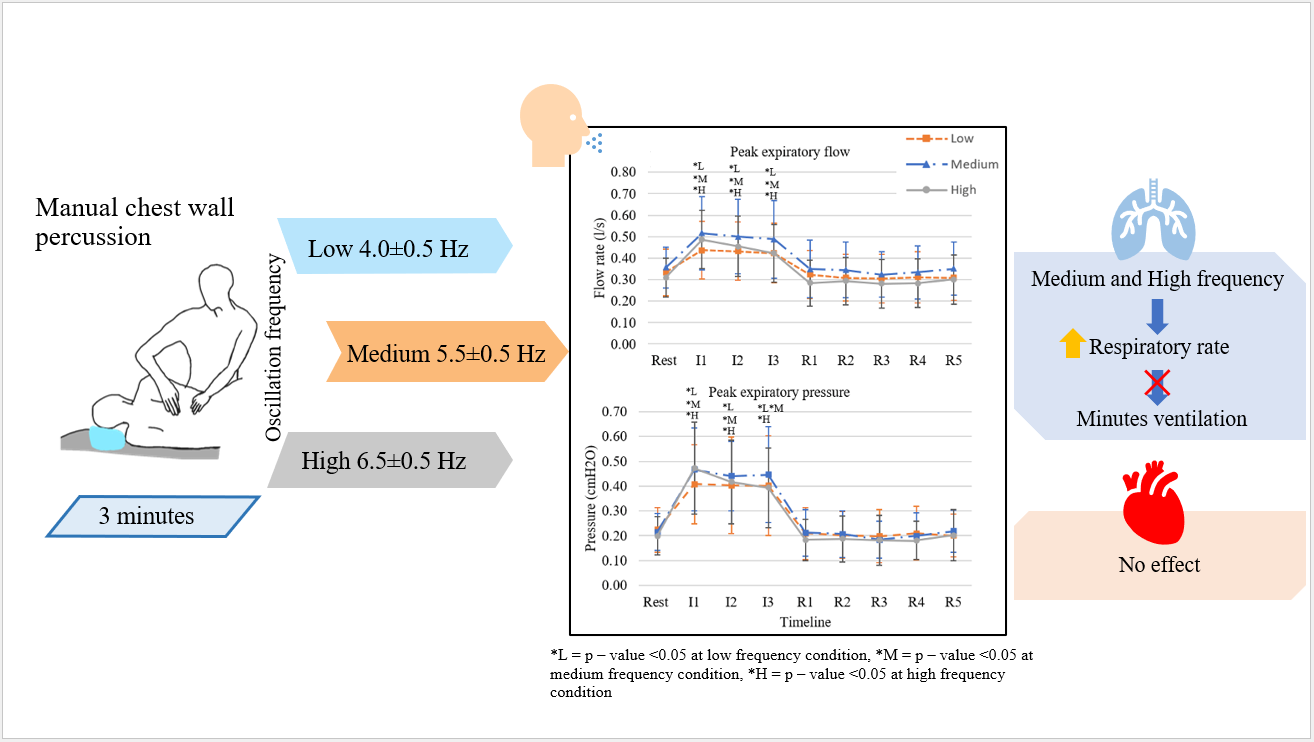
Downloads
References
CPVD Schans. Conventional chest physical therapy for obstructive lung disease. Respir. Care 2007; 52, 1198-206.
J Rodrigues and J Watchie. Cardiovascular and pulmonary physical therapy treatment. In: J Watchie (Ed.). A clinical manual. 2nd eds. WB Saunders, Philadelphia, 2010, p. 298-392.
B Langenderfer. Alternatives to percussion and postural drainage: A review of mucus clearance therapies. J. Cardiopulm. Rehabil. Prev. 1998; 18, 283-9.
JA Pryor. Physiotherapy for airway clearance in adults. Eur. Respir. J. 1999; 14, 1418-24.
CC Zadai. Physical therapy for the acutely ill medical patient. Phys. Ther. 1981; 61, 1746-54.
D Clinkscale, K Spihlman, P Watts, D Rosenbluth and MH Kollef. A randomized trial of conventional chest physical therapy versus high frequency chest wall compressions in intubated and non-intubated adults. Respir. Care 2012. 2012; 57, 221-8.
BK Rubin. Secretion properties, clearance, and therapy in airway disease. Transl. Respir. Med. 2014; 2, 6.
B Button, HP Goodell, E Atieh, YC Chen, R Williams, S Shenoy, E Lackey, NT Shenkute, LH Cai, GR Dennis, RC Boucher and M Rubinstein. Roles of mucus adhesion and cohesion in cough clearance. Proc. Natl. Acad. Sci. 2018; 115, 12501-6.
XM Bustamante-Marin and LE Ostrowski. Cilia and mucociliary clearance. Cold Spring Harb. Perspect. Biol. 2017; 9, a028241.
RP Tomkiewicz, A Biviji and M King. Effects of oscillating air flow on the rheological properties and clearability of mucous gel simulants. Biorheology 1994; 31, 511-20.
KA Flower, RI Eden, L Lomax, NM Mann and J Burgess. New mechanical aid to physiotherapy in cystic fibrosis. Br. Med. J. 1979; 2, 630.
S Blazey, S Jenkins and R Smith. Rate and force of application of manual chest percussion by physiotherapists. Aust. J. Physiother. 1998; 44, 257-64.
WP Wong, JD Paratz, K Wilson and YR Burns. Hemodynamic and ventilatory effects of manual respiratory physiotherapy techniques of chest clapping, vibration, and shaking in an animal model. J. Appl. Physiol. 2003; 95, 991-8.
B Audsavachulamanee, S Aueyingsak, C Ubolsaka-Jones, N Kosura, J Chanapon, N Yubonpan and C Phimphasak. Thai physiotherapists’ performance of manual chest wall percussion on an artificial lung: Frequency, force, and fatigue perception. Arch. Med. Health Sci. 2023; 35, 23-34.
B McCarren and J Alison. Physiological effects of vibration in subjects with cystic fibrosis. Eur. Respir. J. 2006; 27, 1204-9.
P Imle. Percussion and vibration. In: CF Mackenzie, PC Imle and M Ciesla (Eds.). Chest physiotherapy in the intensive care unit. 2nd eds. Williams and Wilkins, Baltimore, 1989, p. 134-52.
AF Connors, WE Hammon, RJ Martin and RM Rogers. The immediate effect on oxygenation in acutely ill patients. Chest 1980, 78, 559-64.
WE Hammon, DR McCaffree and AJ Cucchiara. A comparison of manual to mechanical chest percussion for clearance of alveolar material in patients with pulmonary alveolar proteinosis (phospholipidosis). Chest 1993; 103, 1409-1412.
C Jones. Physical therapy respiratory system techniques and assessment. Klungnana Vitthaya Press, Khon Kaen, Thailand, 2014, p. 101-25.
J Leelarungrayub. Clinical chest physiotherapy. Thammasat Book, Bangkok, Thailand, 2014, p. 133-95.
K Dallimore, S Jenkins and B Tucker. Respiratory and cardiovascular responses to manual chest percussion in normal subjects. Aust. J. Physiother. 1998; 44, 267-74.
D Vines and D Gardner. Airway clearance therapy (ACT). In: RM Kacmarek, JK Stoller and AJ Heuer (Eds.). Egan’s fundamental of respiratory care. 11th eds. Elsevier, Missouri, 2017, p. 951-70.
BL Graham, I Steenbruggen, MR Miller, IZ Barjaktarevic, BG Cooper, GL Hall, TS Hallstrand, DA Kaminsky, K McCarthy, MC McCormack, CE Oropez, M Rosenfeld, S Stanojevic, MP Swanney and BR Thompson. Standardization of spirometry 2019 update. An official American thoracic society and European respiratory society technical statement. Am. J. Respir. Crit. Care Med. 2019; 200, e70-e88.
BM Button and B Button. Structure and function of the mucus clearance system of the lung. Cold Spring Harb. Perspect. Med. 2013; 3, a009720.
W Poncin, G Reychler, M Liistro and G Liistro. Comparison of 6 oscillatory positive expiratory pressure devices during active expiratory flow. Respir. Care 2020; 65, 492-9.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2023 Walailak University

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.






